Analgesia after onychectomy in cats
In this article, we offer guidance on what drug or combination of drugs to use, concentrating mainly on postoperative analgesia.
Roughly 14 million cats are declawed each year in the United States.1 Although many receive medications for postoperative pain, defining the most effective protocol is limited by the inability to compare analgesic regimens. Interpreting behavior in cats to assess pain has been notoriously difficult.2-9 And interpreting objective physiological parameters has not been consistent because of confounding factors such as stress or drug effects.2,3,7-13 Additionally, veterinarians perform several different onychectomy techniques at very different skill levels. And because of the ethical considerations that surround this procedure, providing both the owner and the cat with effective perioperative and postoperative analgesic options is critical. In this article, we offer guidance on what drug or combination of drugs to use, concentrating mainly on postoperative analgesia.
MEASURING THE EFFECT OF ANALGESICS
Historically, pain studies in animals have used visual analog scales, numerical rating scales, and physiological indices to evaluate the efficacy of drugs and procedures at reducing pain.2,9,11,12 These methods have shown great diversity in results.2,10,12-14 Regardless of the method, a subjective evaluation is based on interpreting an animal's behavior. Behavioral characteristics such as vocalization, depression, or aggression that may be associated with animal pain can be difficult to differentiate from drug effects, anxiety induced from the anesthetic or surgical experience, or an animal's nature.3,15,16 Additionally, animals exhausted from surgery or obtunded may be incapable of displaying painful responses, and some animals do not display painful behavior until the severity reaches a high threshold.15 Behavior changes due to pain in cats may even be more subtle than those in dogs, so pain in cats is likely underestimated.2,3,17 Furthermore, both forelimbs are usually operated on in most studies involving onychectomy in cats, requiring the cats to use their paws despite pain. This forced usage may further hide painful behavior. In an effort to reduce the variability of pain scoring, grading scales may be assigned that use strict definitions for mild, moderate, and severe pain. However, these scores are still subjective.
Physiological indices are arguably better than subjective measures for pain evaluation. Heart rate, blood pressure, pupil size, and blood catecholamine, glucose, β-endorphin, and cortisol concentrations have all been used for pain evaluation.2,3,7-13 Unfortunately, they do not correlate well with subjective pain evaluations and are affected by environmental stresses unrelated to pain.2,7-13 Cortisol concentrations, although highly variable, may be the most useful of these physiological indicators.3,11 However, in one study in cats undergoing onychectomy, the control group, which did not receive surgery but was bandaged, did not have significantly different blood cortisol concentrations from the surgery group.3
More recently, pressure platform gait analysis, an objective, reliable, noninvasive method of measurement, has been used to quantify postoperative pain in cats after onychectomy.18 Precise and accurate measurement of limb function after unilateral onychectomy allows objective conclusions to be made regarding which methods provide the most effective pain management.18 This methodology is similar to force platform gait analysis, which is the gold standard for measuring limb function in dogs.19-22 Most clinicians would agree that after elective surgery on a limb, a reasonable estimation of pain is the willingness of the patient to use the affected leg.
INFLUENCE OF ONYCHECTOMY TECHNIQUES ON PAIN
Various surgical techniques have been used to declaw cats, including the scalpel, guillotine, and laser.1,23,24 One study that compared the laser technique with the scalpel technique found that although the cats declawed with the laser had significantly lower pain scores within the first 24 hours, the difference was not clinically significant.23 These pain scores were assessed purely by subjective means.23 Another study that evaluated cortisol concentrations as a determinant of pain found that in the first 24 hours, cats in the scalpel group had increased blood and urine cortisol concentrations; however, complication rates for the laser group were higher than those for the scalpel group.25 This finding conflicts with the results of previous studies and most empirical claims.1,24,25
Another study compared scalpel and guillotine methods retrospectively by using observational data from students.26 This study is difficult to interpret because multiple students performed the surgeries and recorded the observations.26 Additionally, the closure method was not controlled in the comparison.26 Although specific technique in the hands of an experienced surgeon may not cause more pain than another technique, inexperienced surgeons may cause more trauma to surrounding tissues and cause more pain with any technique. Regardless of the technique or skill level, the patient should receive perioperative and postoperative analgesia.
PAIN MANAGEMENT OPTIONS
Several different classes of drugs are used for perioperative analgesia in cats undergoing onychectomy. Opioids, local anesthetics, nonsteroidal anti-inflammatory drugs (NSAIDs), and α2-agonists have all been used in cats with some benefit. N-Methyl-D-aspartate antagonists, such as ketamine, are often used for anesthesia in cats, but specific studies on the analgesic effects postoperatively are not available. Table 1 summarizes some of the most common analgesics used perioperatively. Choosing an analgesic protocol may be confusing because of the multiple advantages and disadvantages of each drug. The duration of action, dosage, cost, side effects, and method of administration vary for all analgesics. Ideally, the protocol should be tailored to the individual patient, and multimodal therapy is likely the most beneficial.

Table 1. Common Drugs and Dosages for Perioperative Analgesics for Feline Onychectomy
Opioids
In general, opioids inhibit neurotransmitters centrally. Opioids are further classified as partial or full agonists or antagonists of the µ or k receptors.8,9 Side effects of opioids include bradycardia, vomiting, respiratory depression, decreased gastrointestinal motility, and dysphoria.8,9 Although µ-receptor agonists are accompanied by more side effects, they provide more profound analgesia. The more commonly used µ agonists in veterinary medicine include hydromorphone, oxymorphone hydrochloride, morphine, and fentanyl citrate. Kappa agonists such as butorphanol, which also has µ antagonistic effects, are associated with less cardiac or respiratory depression or gastrointestinal upset than µ agonists.8,9 Sedation may still occur. Intravenous, intramuscular, or subcutaneous administration typically produces consistent systemic drug concentrations; however, transdermal and oral treatment with opioids produces more variable results in cats.7-11,19,27,28
The most common opioid analgesics studied in cats include butorphanol, buprenorphine hydrochloride, fentanyl, and morphine. One study found that butorphanol (0.4 mg/kg intravenously at extubation and subcutaneously every four hours postoperatively) subjectively provided significantly better analgesia over the control group in cats that had undergone onychectomy.3 Buprenorphine is a partial µ agonist that also has limited side effects; however, the analgesic effects may also have a maximum limit despite increasing doses.8,9 Another disadvantage is that it has a relatively slow onset of action of about one hour.8,9,29 Another study that used subjective pain scoring and cortisol concentrations within 12 hours of surgery found that buprenorphine (0.01 mg/kg intramuscularly) was significantly more effective at pain relief at four hours than oxymorphone (0.05 mg/kg intramuscularly), ketoprofen (2 mg/kg intramuscularly), and saline solution in cats.4 The dose may be important since in a similar study ketoprofen given at a dose of 2 mg/kg intramuscularly outperformed buprenorphine given at a dose of 0.006 mg/kg intramuscularly.29 In another study, buprenorphine (0.01 mg/kg intramuscularly), morphine (0.2 mg/kg intramuscularly), and butorphanol (0.2 mg/kg intramuscularly) raised the thermal threshold of cats, but no difference in degree of temperature tolerated was found among the groups.30 However, buprenorphine and morphine displayed analgesic effects four hours or more after administration, whereas butorphanol had almost immediate effects.30 The analgesic effect of butorphanol and morphine lasted only two hours compared with eight hours provided by buprenorphine.30 These findings are similar to those of another study in which buprenorphine provided better analgesia than morphine more than two hours after administration.31 One study reports the advantage of combining hydromorphone (0.1 mg/kg intramuscularly) and butorphanol (0.4 mg/kg intramuscularly) to increase the duration of action of both drugs.32 Analgesia was decreased over hydromorphone alone, but the duration of action was measured up to nine hours.32
Transdermal fentanyl patches (25 µg/hr) have the advantage of being easily applied; however, a large variation exists in blood fentanyl concentrations among cats, and patches must be applied several hours in advance.5,8,9,16 In a critical review in which several pharmacokinetic studies were compared, it was recommended that the patch be applied seven hours before surgery. The dose recommendation was one 25-µg/hr patch per cat or kitten.28 Studies comparing butorphanol and fentanyl in cats after onychectomy have yielded mixed results.3,4,7,16,18 In one study, cats that received transdermal fentanyl after onychectomy had lower subjective pain scores eight hours after surgery than those that received butorphanol, although both groups had significantly lower mean plasma cortisol concentrations after surgery than before.7 In contrast, another study found that there was no difference in the analgesic effect between fentanyl and butorphanol with subjective evaluation as well as standing foot pressure.16 Recently, gait analysis on unilaterally declawed cats was used to compare butorphanol and transdermal fentanyl after onychectomy.18 All cats were significantly lamer postoperatively with no difference between protocols 24 hours after surgery.18 Forty-eight hours after surgery, cats receiving fentanyl or butorphanol were significantly less lame than those receiving topical bupivacaine. Additionally, cats receiving butorphanol were more lame on Day 2 than those receiving fentanyl based on a ratio calculated for the peak vertical force of the affected leg to the combined peak vertical forces of the remaining three limbs.18 On Days 3 and 12 no significant differences between the groups were present; however, even 12 days after surgery the cats had not returned to normal function.18 This delayed return to normal function may mean that analgesic therapy should be continued past the initial postoperative period. Likely, the length of recovery after onychectomy has been underestimated because of bilateral surgeries.
Continuing analgesia after a cat leaves the hospital is challenging because of difficulty with drug administration. Oral butorphanol has variable uptake and may be metabolized by the gastrointestinal tract and liver, reducing the chances of a therapeutic effect.27 Transdermal fentanyl patches must be replaced every three days, necessitating frequent trips to the veterinarian, and the patches have variable absorption. Buprenorphine is a long-acting opioid commonly given in cats.8,27,29 The pharmacokinetics of oral mucosal administration (i.e. placing drops in the side of the cat's mouth) of the injectable compound suggests that buprenorphine would provide excellent analgesia in a convenient dosing format.27 Although to our knowledge oral buprenorphine has not been evaluated for analgesic properties, the intramuscular route of administration has shown advantages in analgesia compared with butorphanol and morphine.27,29-31
Local anesthetics
Local anesthetics such as lidocaine (up to 4 mg/kg perineurally) or bupivacaine (up to 1 mg/kg perineurally) are commonly used to complement other forms of analgesia or sedation.8,9 They can be applied topically or as a nerve block.8,9,33 The risk of seizures, one side effect of local anesthetics, in cats increases with greater total doses of either drug. In small kittens, saline solution can be added to increase the volume of administration without increasing risk.
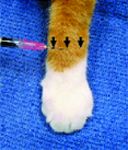
Figure 1. A ring block for the dorsal paw. Arrows show where the local anesthetic should be infused subcutaneously on the dorsal carpus to block the branches of the radial nerve.
Briefly, the mechanism of action of local anesthetics is to block the sodium channels imperative for nerve conduction.8,9 Efficacy likely varies with administration technique and location. Topical bupivacaine was less effective at preventing lameness when compared with opioids in one study.18 Similarly, topical bupivacaine did not improve pain scores when compared with placebo.33 Although randomized, prospective studies have not been performed, ring blocks around the carpus (radial, ulnar, and median nerves) have been advocated (Figures 1 & 2).8,9 The duration of action may be anywhere from three to 10 hours, depending on the local absorption.33 Lidocaine has a shorter duration of action, lasting only one or two hours.8,9 Optimally, we recommend combining regional or topical nerve blocks with other modes of analgesia.
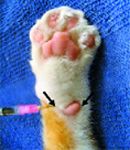
Figure 2. A ring block for the palmar paw. Arrows show where the local anesthetic should be infused subcutaneously on the palmar surface to block the median nerve and palmar branch of the ulnar nerve medial to the accessory carpal pad and the dorsal branch of the ulnar nerve laterally.
NSAIDs
NSAIDs provide analgesia by decreasing inflammation. Moreover, some NSAIDs also decrease central pain perception.8,9 An additional advantage of NSAIDs is that they can be used in conjunction with opioids to provide analgesia.
In cats, the pharmacokinetics varies for different NSAIDs. Additionally, large variation from cat to cat and a potentially small safety margin make dosing difficult.8,9
Adverse effects, including vomiting and diarrhea, are typically self-limiting when an NSAID is discontinued; however, more serious adverse effects may include renal or hepatic necrosis or gastrointestinal ulceration. Drugs that preferentially block the cyclooxygenase 2 (COX-2) inflammatory pathway may have a larger safety margin when considering the probability of gastrointestinal side effects but provide no additional margin of safety for renal side effects.8,9 Because of these side effects, NSAIDs are generally contraindicated in animals that have compromised renal function or underlying gastrointestinal disease and in those that receive corticosteroids. Although directly monitoring renal blood flow is not routine, patients given NSAIDs preoperatively should be monitored closely to decrease the probability of interrupting blood flow to the kidneys.
Thus, drugs that are COX-2 selective are preferred to drugs that are COX-1 selective or nonselective. But even COX-2 selective NSAIDs should be used with caution.
Carprofen, ketoprofen, and meloxicam have been compared in cats after ovariohysterectomy by using subjective measures.29,34 All cats received one dose and were subjectively compared; no significant difference among the groups was found. A study directly comparing the pain scores of cats after ovariohysterectomy concluded that carprofen was preferred to butorphanol because the cats returned to normal interactions earlier with the carprofen at recommended doses.35 Carprofen injectable has been approved in Europe for use in cats at a single perioperative dose of 4 mg/kg given subcutaneously, but oral carprofen is not recommended.36 Meloxicam has been used orally in cats in Europe (0.1 to 0.2 mg/kg every three or four days) for acute and chronic pain.8 A single, one-time dose of 0.3 mg/kg given subcutaneously has recently been approved for cats in the United States. Meloxicam and carprofen are both COX-2 selective, whereas ketoprofen is a nonspecific COX inhibitor. The recommended dosage of ketoprofen in cats is 2 mg/kg given subcutaneously once. The efficacy of ketoprofen (2 mg/kg intramuscularly) has been compared with oxymorphone (0.05 mg/kg intramuscularly) and buprenorphine (0.01 mg/kg intramuscularly) after onychectomy.4 Ketoprofen was no better than oxymorphone or buprenorphine at any time within 12 hours postoperatively.4 However, in a study comparing ketoprofen (2 mg/kg subcutaneously) and buprenorphine (0.006 mg/kg intramuscularly) after ovariohysterectomy, ketoprofen subjectively provided better analgesia within the first 24 hours.29 This discrepancy may be due to the difference in doses.
Alpha-2 agonists
Alpha-2 agonists are most commonly used for sedation or as a premedication. They decrease excitation at presynaptic and postsynaptic junctions.8 Decreased heart rate and contractility occur secondarily to profound peripheral vasoconstriction, and arrhythmias may arise. Alpha-2 agonists are used cautiously to decrease dysphoria that may accompany opioid administration because the sedative effects are synergistic.8 A single dose of medetomidine (15 µg/kg intramuscularly) alone was given after ovariohysterectomy and compared with intramuscular butorphanol and placebo.37 Although subjectively the butorphanol was more effective than the medetomidine, the medetomidine outperformed the placebo.37 However, this effect may have been sedation-related since only subjective determinations of pain were made based on the cats' behavior.37 Therefore, medetomidine alone cannot be recommended as a postoperative analgesic.
CONCLUSION
All good analgesic protocols are tailored to the patient and client. The most common protocols used after onychectomy are presented in Table 1. Most of the work done to compare protocols after onychectomy addresses acute pain relief. One study shows that cats are still lame 12 days after surgery.18 Perioperative analgesics are important to prevent pain up-regulation, but additional analgesics should be considered for more long-term use. Veterinarians are somewhat limited to NSAIDs, fentanyl patches, oral butorphanol, or oral buprenorphine. Caution should be used when prescribing any medications long term, as the literature is unclear about what side effects may occur after more than three or four days.
Although it has not been specifically studied, it is intuitive that a multimodal approach should be used to minimize unwanted side effects while providing the most efficacious analgesia after onychectomy. An example would be combining opioids with an NSAID perioperatively. Additionally, at the time of anesthesia, perineural blocks of the radial, ulnar, and median nerves are recommended. A cat's age and four-paw vs. forepaw onychectomies may require special consideration in addition to more prolonged therapy. Since pain is difficult to assess in cats, subjective evaluation and interpretation of a cat's behavior should not preclude aggressive analgesic treatment of pain.
Wanda J. Gordon, DVM
Michael G. Conzemius, DVM, PhD, DACVS
Department of Veterinary Clinical Sciences
College of Veterinary Medicine
Iowa State University
Ames, IA 5001
REFERENCES
1. Patronek GJ. Assessment of claims of short-and long-term complications associated with onychectomy in cats. J Am Vet Med Assoc 2001;219:932-937.
2. Cambridge AJ, Tobias KM, Newberry RC, et al. Subjective and objective measurements of postoperative pain in cats. J Am Vet Med Assoc 2000;217:685-690.
3. Carroll GL, Howe LB, Slater MR, et al. Evaluation of analgesia provided by postoperative administration of butorphanol to cats undergoing onychectomy. J Am Vet Med Assoc 1998;213:246-250.
4. Dobbins S, Brown NO, Shofer FS. Comparison of the effects of buprenorphine, oxymorphone hydrochloride, and ketoprofen for postoperative analgesia after onychectomy or onychectomy and sterilization in cats. J Am Anim Hosp Assoc 2002;38:507-514.
5. Davidson CD, Pettifer GR, Henry JD Jr. Plasma fentanyl concentrations and analgesic effects during full or partial exposure to transdermal fentanyl patches in cats. J Am Vet Med Assoc 2004;224:700-705.
6. Glerum LE, Egger CM, Allen SW, et al. Analgesic effect of the transdermal fentanyl patch during and after feline ovariohysterectomy. Vet Surg 2001;30:351-358.
7. Gellasch KL, Kruse-Elliott KT, Osmond CS, et al. Comparison of transdermal administration of fentanyl versus intramuscular administration of butorphanol for analgesia after onychectomy in cats. J Am Vet Med Assoc 2002;220:1020-1024.
8. Lamont LA. Feline perioperative pain management. Vet Clin North Am Small Anim Pract 2002;32:747-763.
9. Wright BD. Clinical pain management techniques for cats. Clin Tech Small Anim Pract 2002;17:151-157.
10. Conzemius MG, Hill CM, Sammarco JL, et al. Correlation between subjective and objective measures used to determine severity of postoperative pain in dogs. J Am Vet Med Assoc 1997;210:1619-1622.
11. Day TK, Pepper WT, Tobias TA, et al. Comparison of intra-articular and epidural morphine for analgesia following stifle arthrotomy in dogs. Vet Surg 1995;24:522-530.
12. Holton LL, Scott EM, Nolan AM, et al. Relationship between physiological factors and clinical pain in dogs scored using a numerical rating scale. J Small Anim Pract 1998;39:469-474.
13. Rawlings CA, Tackett RL, Bjorling DE, et al. Cardiovascular function and serum catecholamine concentrations after anesthesia and surgery in the dog. Vet Surg 1989;18:255-260.
14. Holton LL, Scott EM, Nolan AM, et al. Comparison of three methods used for assessment of pain in dogs. J Am Vet Med Assoc 1998;212:61-66.
15. Mathews KA. Pain assessment and general approach to management. Vet Clin North Am Small Anim Pract 2000;30:729-755.
16. Franks JN, Boothe HW, Taylor L, et al. Evaluation of transdermal fentanyl patches for analgesia in cats undergoing onychectomy. J Am Vet Med Assoc 2000;217:1013-1020.
17. Benson GJ, Wheaton LG, Thurmon JC, et al. Postoperative catecholamine response to onychectomy in isoflurane-anesthetized cats. Vet Surg 1991;20:222-225.
18. Gordon WJ, Romans C, Evans R, et al. Objective evaluation of the efficacy of bupivacaine, butorphanol, and fentanyl patch after onychectomy using pressure platform gait analysis (abst), in Proceedings. 31st Annu Conf Vet Orthop Soc 2004.
19. Besancon MF, Conzemius MG, Derrick TR, et al. Comparison of vertical forces in normal dogs between the AMTI Model OR6-5 Force Platform and the Tekscan (Industrial Sensing Pressure Measurement System) Pressure Walkway. Vet Comp Orthop Traumatol 2003;16:153-157.
20. Budsberg SC, Verstraete MC, Soutas-Little RW, et al. Force plate analyses before and after stabilization of canine stifles for cruciate injury. Am J Vet Res 1988;49:1522-1524.
21. Budsberg SC. Long-term temporal evaluation of ground reaction forces during development of experimentally induced osteoarthritis in dogs. Am J Vet Res 2001;62:1207-1211.
22. Romans CW, Conzemius MG, Horstman CL, et al. Use of pressure platform gait analysis in cats with and without bilateral onychectomy. Am J Vet Res 2004;65:1276-1278.
23. Mison MB, Bohart GH, Walshaw R, et al. Use of carbon dioxide laser for onychectomy in cats. J Am Vet Med Assoc 2002;221:651-653.
24. Lopez NA. Using CO2 lasers to perform elective surgical procedures. Vet Med 2002;97:302-314.
25. Levy J, Lapham B, Hardie E, et al. Evaluations of laser onychectomy in the cat (abst.), in Proceedings. 19th Annu Meet Soc Laser Med 1999;73.
26. Tobias KS. Feline onychectomy at a teaching institution: A retrospective study of 163 cases. Vet Surg 1994;23:274-280.
27. Robertson SA, Taylor PM, Sear JW. Systemic uptake of buprenorphine by cats after oral mucosal administration. Vet Rec 2003;152:675-678.
28. Hofmeister EH, Egger CM. Transdermal fentanyl patches in small animals. J Am Anim Hosp Assoc 2004;40:468-478.
29. Slingsby LS, Waterman-Pearson AE. Comparison of pethidine, buprenorphine and ketoprofen for postoperative analgesia after ovariohysterectomy in the cat. Vet Rec 1998;143:185-189.
30. Robertson SA, Taylor PM, Lascelles BDX, et al. Changes in thermal threshold response in eight cats after administration of buprenorphine, butorphanol and morphine. Vet Rec 2003;153:462-465.
31. Stanway GW, Taylor PM, Brodbelt DC. A preliminary investigation comparing pre-operative morphine and buprenorphine for postoperative analgesia and sedation in cats. Vet Anaesth Analg 2002;29:29-35.
32. Lascelles BDX, Robertson SA. Antinociceptive effects of hydromorphone, butorphanol, or the combination in cats. J Vet Intern Med 2004;18:190-195.
33. Winkler KP, Greenfield CL, Benson GJ. The effect of wound irrigation with bupivacaine on postoperative analgesia of the feline onychectomy patient. J Am Anim Hosp Assoc 1997;33:346-352.
34. Slingsby LS, Waterman-Pearson AE. Postoperative analgesia in the cat after ovariohysterectomy by use of carprofen, ketoprofen, meloxicam or tolfenamic acid. J Small Anim Pract 2000;41:447-450.
35. Al-Gizawiy MM, Rude EP. Comparison of preoperative carprofen and postoperative butorphanol as postsurgical analgesics in cats undergoing ovariohysterectomy. Vet Anaesth Anal 2004;31:164-174.
36. David A, Simon T. Use of Rimadyl in cats (lett). Vet Rec 1999;25:743.
37. Ansah OB, Vainio O, Hellsten C, et al. Postoperative pain control in cats: Clinical trials with medetomidine and butorphanol. Vet Surg 2002;31:99-103.