Be the life of the party! Make radiology friends and influence ER visits
OK, so you're not much of a party animal? No worries. Dr. Rachel Pollard offers some friendly radiology tips for life in the ER.

Getty ImagesLike successful socializing at a cocktail party, radiology in the ER benefits from a planned strategy of attack. Consider these hacks and facts from Rachel Pollard, DVM, PhD, DACVR, at her recent talk on imaging in the ER at CVC:
Let's get ready to mingle!
“Hey, who's here?” When you go to a party, where's the first place you go? Probably the bar. But then after that you look for people you know. Find the things that are supposed to be there. This is the "find your friends" tactic. For example, if you are looking at the abdomen, find the stomach (the most cranial gas bubble); identify the liver, spleen, kidneys and bladder; and follow the intestinal loops as best you can. It helps to identify the familiar structures you know are supposed to be there first, says Dr. Pollard.
Next note if there is anyone who doesn't look like they should be there. Who's the weird old guy at the party (e.g. that suspicious lump in the abdomen)?
“Weren't Bill and Ted supposed to come?” If a couple of your friends are missing (or you can't see them very well), consider where they may have gone. This might indicate what's wrong.
Say you're evaluating the abdomen and you can't find the spleen or the bladder. This could indicate there's fluid in the abdomen-reduced abdominal serosal detail results in boarder effacement. It's common to not see the right kidney in a bigger dog, says Dr. Pollard.
Next, note if there's a reason the friends are absent. Could they have a good reason for not being there, such as a possible splenectomy? Bladder trauma could cause the bladder to be missing, resulting in a uroabdomen. What about hemorrhage? In a trauma patient, these two are the most likely reasons for your friends to be missing.
What to drink? 2 urinary tract tips
1. In the case of a ruptured bladder it's very hard to identify a tear in the bladder ultrasonographically. Why? Because after a tear or rupture, the bladder can come back together or fold on itself. So if you don't see a hole in the bladder wall on an ultrasonographic examination, and especially for ureteral ruptures, it doesn't mean it's not there, says Dr. Pollard. If you're unsure of the integrity of the urinary tract, a radiographic contrast study would be best. For contrast material, nonionic iodinated contrast is more expensive than ionic iodine contrast material. However, nonionic contrast material is less irritating to the organs and tissues and should be used when you're worried about ruptures.
2. When obtaining urethrograms, it's best to take a series, because one view can be difficult to interpret on its own. Dr. Pollard's advice: Inject some contrast, take a radiograph, move the catheter, inject some more, take another radiograph, and so on. Take at least three views to help interpret your urethrograms.
Go with your gut impression-6 abdominal tips
1. Obtain three views of the abdomen including right lateral, left lateral and ventrodorsal projections. Dr. Pollard says she used to find this cumbersome, but now she appreciates the information gained from the left lateral, particularly when trying to evaluate the pylorus. She says it's essential for identifying foreign material and masses in the stomach and really helps confirm diagnoses.
2. Consider two big causes of a portion of bowel looking spastic or corrugated (angry): There's either inflammation inside (enteritis) or outside (e.g. peritonitis, pancreatitis) Do not confuse this with plication.
3. A mass in the abdomen that contains gas patterns is almost always an abscess or is intestinal in origin (possibly a hepatic abscess, splenic abscess or intestinal mass).
4. Gas with sharp edges is likely a pocket of gas, which is not contained in bowel. If you see gas with sharp edges, especially near the diaphragm, be suspicious of free abdominal air (Figure 1, below). Free abdominal air is typically emergent and arises from penetrating wounds or ruptured bowel. You can use ultrasound to confirm the presence of free abdominal air. Gas interface has a hyperechoic interface with a dirty grey shadow, not a black shadow as you would see with a mineral origin shadow.
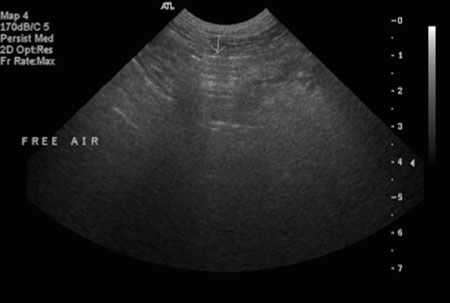
Figure 1: Free air
5. When performing abdominal ultrasonographic examinations, try to look at every organ every time. The only time that you image a single organ is at rechecks.
6. When you're using horizontal beam radiography (Figure 2 below), the x-ray source is rotated so that it shoots horizontally across the table. The detector is also moved to the opposite side of the table and must be secured or held in place. This technique can be performed with the patient in sternal recumbency (to look for fluid lines in pulmonary lesions as might be seen with an abscess) or in left lateral recumbency (to look for free abdominal air).
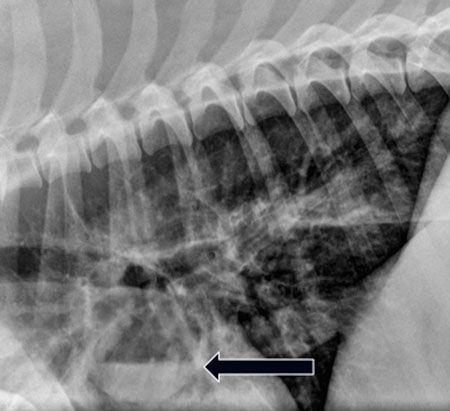
Figure 2: Horizontal beam radiography
Get everything off your chest-14 thoracic tips
1. For pulmonary patterns, Dr. Pollard uses a process of elimination instead of the find your friends tactic mentioned above (although you can also use this method). Her process of elimination involves:
• First look for an alveolar pattern. The two hallmarks are air bronchograms (think trees in the fog) and a clearly defined lung lobe margin (lobar sign).
• Then look for a bronchial pattern. Think donuts and tram lines.
• Lastly, look for an interstitial pattern, where you see too much opacity in the lungs but it is not an alveolar or bronchial pattern. A hallmark of this pattern is the loss of small vessel visibility in the periphery.
2. If you do try the "find your friends" approach in the chest, find the heart, lungs and pulmonary vasculature (artery, bronchus and veins-the veins are central and ventral).
3. Always take three radiographic views of the chest as well-a right lateral, a left lateral and ventrodorsal or dorsoventral.
4. Pneumonitis is a vascular permeability issue from a systemic inflammatory process, such as leptospirosis or pancreatitis. It results in noncardiogenic pulmonary edema. Edema typically forms in the caudodorsal and perihilar regions of the lungs, whether it's cardiogenic or not, says Dr. Pollard.
5. Aspiration pneumonia can affect any of the cranial lung lobes. It tends to be ventral.
6. With acute-onset heart failure, the lung pattern can be more diffusely distributer, but edema still tends to be heaviest in the caudodorsal lung.
7. When you take lateral views of the lungs, the left lateral view shows the right lung (or the up lung) and vice versa.
8. Pulmonary vasculature is better outlined on a dorsoventral view. With a dorsoventral view, the cardiac silhouette also sits at a more normal position. In fact, for cardiac assessment, dorsoventral views are better for evaluation.
9. With lung lobe torsion you can see an alveolar pattern in the torsed lung lobe. The hallmark of lung lobe torsion (or abscessed lung lobe) is the vesiculated gas pattern in the lung, sort of like a sponge. Often a hemorrhagic component is present within the pleural fluid when lung lobe torsion is present.
10. If ventrodorsal and dorsoventral views are taken and the thoracic opacity changes in location, it's most likely pleural effusion (fluid), says Dr. Pollard. And if the opacity doesn't change, then you're more likely dealing with pulmonary infiltrate.
11. When there is a heavy alveolar pattern affecting all lobes on one side of the thorax, pulmonary hemorrhage should be very high on your differential list.
12. Rodenticide toxicosis likes to hemorrhage into “potential spaces,” says Dr. Pollard, such as the mediastinum, the tracheal wall and the retroperitoneum.
13. In deep-chested dogs the trachea should deviate away from the spinal column. This is not true for all dogs, but definitely for deep-chested big dogs.
14. Finally, Dr. Pollard says to remember that a chest radiograph can still look normal in a coughing dog with infectious or non-infectious inflammatory airway disease (bronchitis).
Hilal Dogan, BVSc, is an associate at At Home Animal Hospital in Maui, Hawaii. She started the Veterinary Confessionals Project as a senior veterinary student at Massey University in New Zealand.