A challenging case: Blindness and a history of cutaneous nodules in a cat
A 12-year-old 8-lb (3.6-kg) castrated male domestic shorthaired cat was evaluated initially at Bissonnet/Southampton Veterinary Clinic followed by evaluation at Gulf Coast Animal Eye Clinic and Gulf Coast Veterinary Specialists for blindness of one month's duration.
A 12-year-old 8-lb (3.6-kg) castrated male domestic shorthaired cat was evaluated initially at Bissonnet/Southampton Veterinary Clinic followed by evaluation at Gulf Coast Animal Eye Clinic and Gulf Coast Veterinary Specialists for blindness of one monthduration. The owner had observed the cat walking along the perimeter of rooms and showing a reluctance to jump up on things. The cat's activity level had decreased as well. The cat's appetite was normal initially but began to decrease over the subsequent weeks. The owner had not noticed any coughing, sneezing, nasal discharge, vomiting, or abnormal stools.
The cat was indoor-only; another cat in the household was indoor-outdoor. About a month before presentation, the cat was vaccinated by its previous veterinarian against rabies, feline rhinotracheitis, feline panleukopenia, and calicivirus, feline leukemia virus (FeLV), and feline immunodeficiency virus (FIV) infections.

Vital Stats
HISTORY
Five months before this presentation, another veterinarian had evaluated the cat for recurrent ulcerated nodules on its head. A biopsy and histologic examination of the initial lesions had revealed chronic nodular pyogranulomatous dermatitis and panniculitis. No infectious agents had been identified. The lesions resolved after treatment with penicillin and dexamethasone followed by enrofloxacin. However, the lesions reappeared about two months later and were treated with the same regimen. The lesions appeared to resolve a second time.
PHYSICAL AND OPHTHALMIC EXAMINATIONS
At presentation, physical examination findings were unremarkable except for a few small excoriations rostral to the right ear. The owner had not noted pruritus, so the excoriations were attributed to trauma, possibly from the other cat in the household.
An ophthalmic examination revealed changes consistent with granulomatous chorioretinitis and pan uveitis in both eyes. Other ophthalmic findings included bilateral conjunctival hyperemia, moderate corneal stromal edema, keratic precipitates (left eye), bilateral moderate aqueous flare and cells, dilated and fixed pupils, nuclear sclerosis, marked vitreous cellular infiltrates and fibrin clumps, bilateral exudative detachment affecting the inferior portion of the retinas, and numerous intraretinal and subretinal granulomas. Intraocular pressures were normal at 14 mm Hg, and iridocorneal angles exhibited moderate narrowing. Dazzle light reflexes were present in both eyes but were markedly reduced.
DIAGNOSTIC TESTING
Abnormalities detected on a complete blood count and serum chemistry profile included anemia (packed cell volume 24%; reference range = 29% to 48%), eosinophilia (absolute eosino phils 1,365 units/μl; reference range = 0 to 1,000 units/μl), hyperglobulinemia (7.1 g/dl; reference range = 2.3 to 5.3 g/dl), mildly elevated blood urea nitrogen (BUN) concentration (38 mg/dl; reference range = 14 to 36 mg/dl), mildly elevated amylase activity (1,225 IU/L; reference range = 100 to 1,200 IU/L), and elevated creatinine kinase activity (1,553 IU/L; reference range = 56 to 529 IU/L). Urinalysis revealed a low urine specific gravity (1.023). Urine bacterial culture results were negative. Tests to detect FeLV and FIV infection were recommended after the blood test results were evaluated, but attempts to contact the owner to obtain permission failed.
DIFFERENTIAL DIAGNOSES
Differential diagnoses for the anemia include anemia of chronic renal disease, anemia secondary to inflammation or infection, FeLV infection, FIV infection, bone marrow disorders, and neoplasia. Differential diagnoses for the eosinophilia include allergic disease, parasitic diseases, neoplasia, fungal infection, and viral infection such as FeLV infection. Differential diagnoses for the hyperglobulinemia include infectious disease and neoplasia. Differential diagnoses for the elevated BUN concentration with concurrent low urine specific gravity include chronic or acute renal insufficiency and pyelonephritis. The elevated amylase activity was attributed to renal insufficiency. Differential diagnoses for the mild creatinine kinase activity elevation include restraint, physical activity, and trauma. The increase was considered too small to be attributed to a primary myositis. Differential diagnoses for the ocular lesions include ocular mycoses and mycobacterial infection.
ADDITIONAL DIAGNOSTIC PROCEDURES
To rule out systemic fungal disease, thoracic radiography and abdominal ultrasonography were performed. The thoracic radiographic examination results were normal. Abdominal ultrasonography revealed a small amount of echogenic gravity-dependent debris in the bladder and evidence of chronic renal disease with multiple renal infarcts. The spleen was subjectively enlarged but exhibited normal echogenicity and was homogeneous. No evidence of systemic fungal infection or neoplasia was found on imaging studies.
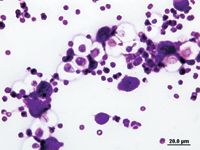
Figure 1. Cytologic examination of the vitreous fine-needle aspirate stained with Diff-Quik (Dade Behring) revealed multiple Cryptococcus species organisms. Cryptococcus species appear as a yeast organism surrounded by a thick nonstaining capsule that can reach up to 30 õm thick.
To rule out ocular mycoses, the cat was anesthetized, the left eye was routinely prepared for surgery, and vitreous paracentesis of the left eye was performed. A focus of vitreous debris was localized using indirect ophthalmoscopy. A 20-ga needle was used to puncture the bulbar conjunctiva and underlying sclera about 7 mm posterior to the limbus at the 1-o'clock position. The needle was directed caudomedially to the debris focus, and a vitreous sample was obtained by aspiration. Cytologic examination of the aspirate revealed occasional neutrophils and monocytes and numerous Cryptococcus species organisms (Figures 1 & 2).
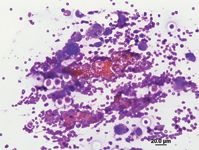
Figure 2. Cytologic examination of the vitreous fine-needle aspirate stained with Diff-Quik revealing multiple red and white blood cells and Cryptococcus species organisms.
TREATMENT AND FOLLOW-UP
The cat was treated for ocular cryptococcosis with 10 mg/kg itraconazole orally once daily.
The cat was presented for a recheck ophthalmic examination about three weeks after treatment was initiated. The examination revealed improvement of intraocular inflammation characterized by decreased aqueous flare and the absence of aqueous cellular debris. The retinal detachment and granulomatous infiltrates were resolved in the left eye, and perivascular edema was still present. However, both pupils remained dilated and fixed, and marked vitreous debris present in the right eye prevented visualization of the retina. Dazzle reflexes remained poor bilaterally. Intraocular pressure results were low normal (right eye = 8 mm Hg, left eye = 7 mm Hg). The owner was advised to continue the itraconazole.
The patient was not presented for subsequent recommended recheck examinations but was presented three months later for euthanasia. The cat now weighed 3.8 lb (1.7 kg), having lost 4.2 lb (1.9 kg), and was no longer eating or drinking. Physical examination revealed severe cachexia and generalized weakness, dehydration, absent menace response, and fixed and dilated pupils. On neurologic examination, the cat appeared to have normal mentation, but the severe muscle weakness made it difficult to assess ambulation and reflexes. The owner declined further diagnostic tests, and a postmortem examination was not performed.
DISCUSSION
Cryptococcosis is the most commonly diagnosed systemic mycosis in cats.1 The specific variety or serotype of Cryptococcus neoformans is rarely identified in affected patients in North America.2 Cryptococcus species can be found worldwide in temperate, tropical, and subtropical climates (cryptococcosis, unlike most fungal diseases, does not have a specific geographic distribution).1 Cryptococcus neoformans var neoformans is found in soil and pigeon excreta.3 Cryptococcus neoformans var gattii is associated with eucalyptus trees and had been considered a problem only in subtropical regions of Australia and South America. However, a recent retrospective study of an outbreak of cryptococcosis in a variety of animals in southwestern British Columbia reported that 13 of the 15 cultures obtained revealed C. neoformans var gattii.2
Pathogenesis
Unlike Blastomyces, Histoplasma, and Coccidioides species, which typically colonize the lungs first, Cryptococcus species initially colonize the nasal passages.4 Once inside the host, the cryptococcal organism regenerates its thick capsule, making it too large (5 to 20 μm) to enter smaller airways. Because of that, spread to the lower respiratory tract is rare.1 However, two retrospective studies in North America described three of six cats and six of nine cats, respectively, with cryptococcal invasion of lung tissue.2,5 Hematogenous or local spread to the central nervous system (CNS), skin, or eyes can also occur.1
In people, immunosuppression is a common predisposing factor in the development of cryptococcosis. In cats, immunosuppression secondary to FeLV and FIV infection has been suggested as a contributing factor in the development of cryptococcosis. However, one study reported the seroprevalence of FeLV and FIV in a population of Cryptococcus species-infected cats to be the same as or less than that of a normal population of cats.1 In a study evaluating the fungal flora on the skin and mucous membranes of 35 retroviral-infected cats and 50 FeLV- and FIV-seronegative cats, C. neoformans was isolated from only one cat that was asymptomatic and seronegative for retrovirus infection.6 It has been suggested that cats seropositive for FeLV and FIV infection are more severely affected by the disease and have poorer response to treatment.7
Because the cat in this case was previously vaccinated for FIV, testing for FIV would likely have yielded a positive antibody test and would have been of questionable value. However, antigen testing or FeLV testing would have been valuable for determining the prognosis in this case.
Typical clinical findings
Clinical signs are typically manifestations of nasal, cutaneous, ocular, or CNS involvement. Nonspecific signs including depression and anorexia leading to weight loss are common. Although the cat in this case presented with no upper respiratory signs, sneezing, snuffling, and nasal discharge occur in 50% to 80% of affected cats. The nasal discharge can be bilateral or unilateral and serous, mucopurulent, or hemorrhagic. Proliferative masses or ulcerated lesions of the nasal cavity can also occur.7
Skin lesions are present in about 40% to 50% of affected cats and include papules and nodules that may or may not become ulcerated or drain.1 The cat in this case had a history of nodular skin lesions. However, it is unclear if the lesions resulted from cryptococcosis because no organisms were found on histologic examination and the lesions resolved with antibiotics and low doses of glucocorticoids.
Ocular signs occur in about 20% to 25% of feline cryptococcosis cases and include chorioretinitis, optic neuritis, and anterior uveitis.7 Chorioretinitis, as seen in this case, is caused by the formation of pyogranulomatous lesions beneath the retina, which appear as poorly marginated grayish-white masses. Extensive exudate between the neurosensory retina and the retinal-pigmented epithelium can lead to retinal detachments and blindness.3
CNS disease occurs in about 20% of affected cats; CNS signs include depression, circling, seizures, ataxia, head pressing, paresis, behavior changes, and cranial nerve deficits. Hematogenous spread or invasion through the cribriform plate are possible routes of spread to the CNS.7 The cat in this case appeared normal on neurologic examination; however, its decreased appetite and activity level may have been manifestations of neurologic involvement.
Diagnosis
Definitive diagnosis is best obtained by organism identification either through cytologic or histologic examination of affected sites. Organisms are commonly found in nasal and skin exudates, nodule aspirates, cerebrospinal fluid, or subretinal or vitreous aspirates.7 A cytologic specimen is best examined using Gram's stain or new methylene blue stain. Wright's stain is also often used but can cause the organism to shrink, distorting the capsule.1 Diff-Quik (Dade Behring) was used in this case. Cryptococcus neoformans can be cultured from exudates, cerebrospinal fluid, urine, joint fluid, or tissue samples if the sample is large enough. The organism grows readily on Sabouraud's dextrose agar, with yeast appearing in two days to six weeks.7
Serologic testing with latex agglutination to detect cryptococcal capsular antigen can be used if no organisms are found on cytologic or histologic examination. Antigen can be detected in the serum, aqueous humor, or cerebrospinal fluid of infected animals.8 Although not used in this case, antigen titers can be used to monitor response to therapy.4 One study showed that Cryptococcus species capsular antigen titers drop to less than 10% of the initial titer within two months if the therapy is effective.4,9
Prognosis
Cryptococcosis in cats without CNS or ocular disease typically has a favorable prognosis.8 Cases with only nasal or cutaneous involvement generally resolve with treatment.8 When extensive chorioretinitis is present, especially with concurrent retinal detachments, the prognosis for vision is poor. Secondary glaucoma can also develop.3
Treatment
Treatment for cryptococcosis with a triazole antifungal, such as fluconazole (50 mg/cat orally twice a day) or itraconazole (10 mg/kg orally once a day),7 is typically recommended for an average of eight and a half months, or at least for one or two months after clinical signs resolve.1,8 Fluconazole is the most effective.7 But because itraconazole is dosed once a day, it may be preferred in cats that are difficult to medicate. Fluconazole has low protein binding and readily crosses the blood-brain barrier.5 Itraconazole has high protein binding and only develops low concentrations in the CNS; however, both fluconazole and itraconazole are effective for treating CNS disease.8 Because of its low protein binding, fluconazole also readily crosses the blood-aqueous and blood-retinal barriers, making it an ideal choice for ocular disease as well.10 Ketoconazole is not recommended because of its decreased efficacy and increased potential for adverse effects.7
Amphotericin B and flucytosine have synergistic effects against fungal organisms and appear to be useful in treating CNS disease. Flucytosine crosses the blood-brain barrier better than amphotericin B or ketoconazole.8 Flucytosine (25 to 50 mg/kg) is given orally four times daily.7 Amphotericin B (0.5 to 0.8 mg/kg) diluted in 400 ml of 0.45% saline solution containing 2.5% dextrose is administered subcutaneously two to three times weekly. Take care to properly dilute the amphotericin B because subcutaneous administration of more concentrated amphotericin B can lead to sterile abscess formation. Amphotericin B can also be used in conjunction with a triazole antifungal.7 Because of higher incidences of adverse effects, amphotericin B and flucytosine are recommended only in patients that fail to respond to azoles.8
Public health
Cryptococcosis is not considered a public health threat. The organism cannot spread from one animal to another through contact with tissue or body fluids, and the organism does not aerosolize from infected tissues. Animals can serve as sentinel species for monitoring the disease in a geographic area.2 A hydrated lime solution (40 g/L water) at 1.36 L/m2 can be used to treat the environment, such as areas with a high concentration of pigeon droppings.8
SUMMARY
As the most commonly diagnosed systemic mycosis in cats, cryptococcosis should be considered in the differential diagnoses for any cat with upper respiratory, ocular, dermatologic, or neurologic signs. Definitive diagnosis is best obtained by cytologic or histologic organism identification. Antigen titers are an essential diagnostic test to monitor response to treatment. Treatment with fluconazole or itraconazole is the first choice. Life-threatening cases can be treated with amphotericin B and flucytosine if they fail to respond to a triazole antifungal. Treatment continues for one to two months after clinical signs resolve. Treatment fails more often in patients with ocular and CNS disease.3
Acknowledgment
The authors thank Theresa E. Rizzi, DVM, DACVP, at the Boren Veterinary Medical Teaching Hospital at Oklahoma State University for photographing the fine-needle aspirate microscope slides.
Holly Polf, DVM*
Bissonnet/Southampton Veterinary Clinic
2028 Bissonnet St.
Houston, TX 77005
Michelle Fabiani, DVM, DACVR
Gulf Coast Veterinary Specialists
Diagnostic Imaging
1111 West Loop South
Houston, TX 77027
James F. Swanson, DVM, MS, DACVO
Gulf Coast Animal Eye Clinic
1551 Campbell Road
Houston, TX 77055
*Dr. Polf's current address is Gulf Coast Veterinary Specialists, Diagnostic Imaging, 1111 West Loop South, Houston, TX 77027.
REFERENCES
1. Jacobs GJ, Medleau L. Cryptococcosis. In: Green CE, ed. Infectious diseases of the dog and cat. 2nd ed. Philadelphia, Pa: WB Saunders Co, 1998;383-390.
2. Lester SJ, Kowalewich NJ, Bartlett KH, et al. Clinicopathologic features of an unusual outbreak of cryptococcosis in dogs, cats, ferrets, and a bird: 38 cases (January to July 2003). J Am Vet Med Assoc 2004;225:1716-1722.
3. Ward DA. Oculomycosis. In: Bonagura J, ed. Kirk's current veterinary therapy XII: small animal practice. Philadelphia, Pa: WB Saunders Co, 1995;1257-1261.
4. Legendre AM, Toal RL. Diagnosis and treatment of fungal diseases of the respiratory system. In: Bonagura J, ed. Kirk's current veterinary therapy XIII: small animal practice. Philadelphia, Pa: WB Saunders Co, 2000;815-819.
5. Gerds-Grogan S, Dayreli-Hart B. Feline cryptococcosis: a retrospective evaluation. J Am Anim Hosp Assoc 1997;33:118-122.
6. Sierra P, Guillot J, Jacob H, et al. Fungal flora on cutaneous and mucosal surfaces of cats infected with feline infectious immunodeficiency virus or feline leukemia virus. Am J Vet Res 2000;61:158-161.
7. Taboada J, Grooters AM. Systemic mycoses. In: Ettinger SJ, Feldman EC, eds. Textbook of veterinary internal medicine. 6th ed. St Louis, Mo: Elsevier, 2005;671-690.
8. Lappin MR. Infectious upper respiratory diseases I and II, in Proceedings. West Vet Conf 2003.
9. Jacobs GJ, Medleau L, Calvert C, et al. Cryptococcal infection in cats: factors influencing treatment outcome, and results of sequential serum antigen titers in 35 cats. J Vet Intern Med 1997;11:1-4.
10. Krohne SG. Canine systemic fungal infections. Vet Clin North Am Small Anim Pract 2000;30:1063-1090.