Dermatologic manifestations and nutritional management of adverse food reactions
Most practitioners recognize that some dogs and cats with pruritus or gastrointestinal conditions can be managed either in part or fully by feeding a limited-antigen diet.
Most practitioners recognize that some dogs and cats with pruritus or gastrointestinal conditions can be managed either in part or fully by feeding a limited-antigen diet. However, resolution of these patients' clinical signs alone does not confirm an allergic cause since dogs and cats with food intolerances may respond to this approach as well (Table 1). True food allergy is immunologically mediated, whereas food intolerances are not. Because the exact pathogenesis and true incidence of food allergy in dogs or cats have not been fully elucidated, we should refer to affected patients as having an adverse food reaction.

In people, food allergies are most common in infants and young children, and most food allergies are mediated by IgE antibodies. Children with an atopic predisposition are at increased risk for showing signs of food allergies, and in 40% of children with atopic dermatitis, food allergens can trigger disease.1
In a recent evaluation of dogs with atopic dermatitis triggered by environmental allergens, 22 of 96 (23%) had a concurrent adverse food reaction.2 Canine models of food allergy have been reported.3-5 Most are dogs that have been selected for high IgE production and, when sensitized with food allergens by parenteral routes, will mount allergen-specific IgE responses. In most cases, these responses are accompanied by dermatologic or gastrointestinal signs. At North Carolina State University, a unique colony of atopic dogs spontaneously manifests food allergy. When fed soy, chicken, or corn, they develop pruritus, otitis, and, in some cases, gastrointestinal signs.6,7
In this article, I will review the process of diagnosing adverse food reactions and, in particular, indicate how it can be performed successfully. The best method for diagnosing adverse food reaction is to perform a diet trial, and it is vital that the trial be performed correctly.
CLINICAL SIGNS OF FOOD ALLERGY

Table 1: Definitions of Common Food Sensitivity Terms*
The most common cutaneous manifestation of adverse food reaction in dogs and cats is pruritus. But before investigating a possible dietary causality, it is important to rule out other common causes of pruritus, such as parasitic infestations. Furthermore, there should be historical evidence of year-round disease. If perennial disease is present but seasonal worsening is reported, the possibility of concurrent hypersensitivity to dietary and environmental allergens must be considered.
In dogs
Although clinical signs usually become evident in puppies or young adults before 3 years of age, adverse food reactions can develop in dogs at any age.2 Labrador retrievers may be at an increased risk.8,9 There is no sex predisposition.

Figure 1. A 10-month-old female Labrador retriever at initial presentation exhibiting self-induced periocular alopecia and blepharitis secondary to dietary-induced pruritic skin disease. (Reprinted with permission from Foster AP, Foil CS. BSAVA manual of small animal dermatology. 2nd ed. Oxford, UK: Blackwell Publishing, 2003.)
The predominant presenting clinical sign of food allergy in dogs is a nonseasonal pruritus. The pruritus can involve any body region but is often identical to that which we associate with classical canine atopic dermatitis involving the ventral abdomen, axillae, groin, muzzle, and periocular, perianal, and palmar or plantar and dorsal interdigital skin (Figures 1 & 2). A recurrent superficial pyoderma in the absence of pruritic skin disease has also has been recognized in a few cases.9,10 Recurrent otitis externa is a common complaint and may be present in 56% to 80% of cases (Figure 3).8-11

Figure 2. The same dog after four weeks on a limited-antigen diet trial. (Reprinted with permission from Foster AP, Foil CS. BSAVA manual of small animal dermatology. 2nd ed. Oxford, UK: Blackwell Publishing, 2003.)
There is debate over the frequency of concurrent gastrointestinal signs in patients with dermatologic signs of adverse food reaction.8,11 In my clinical experience, intermittent vomiting, diarrhea, colitis, or borborygmus occurs in 50% to 60% of dogs. Secondary cutaneous or otic infections with bacteria or yeast also are common. It has been reported that adverse food reaction may respond poorly to antipruritic doses of glucocorticoids, but most clinicians now agree this distinction is not a useful diagnostic feature.
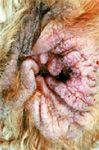
Figure 3. Chronic otitis externa in a dog, a consequence of unmanaged food allergy.
In cats
Cats often present with pruritus of the face and neck (Figures 4-6), although clinical signs can be diverse and include miliary dermatitis, symmetric alopecia, and manifestations of the eosinophilic granuloma complex. Concurrent gastrointestinal signs have been reported in about 30% of cats.12-14 No age, sex, or breed predisposition has been noted in cats.

Figure 4. A 5-month-old cat at initial presentation with facial pruritus suspected to be due to food allergy.

Figure 5. The same cat after 10 weeks on a limited-antigen diet. (Reprinted with permission from Foster AP, Foil CS. BSAVA manual of small animal dermatology. 2nd ed. Oxford, UK: Blackwell Publishing, 2003.)
PERFORMING A DIET TRIAL
The current gold standard method for identifying canine or feline adverse food reaction is to observe improvement of clinical signs when the animal is fed a novel protein diet followed by a recurrence of clinical signs when a previously fed foodstuff is reintroduced. This method generally requires feeding the novel diet for a minimum of six weeks, although some patients may continue to improve for up to eight to 10 weeks, particularly if concurrent secondary infections are present.8
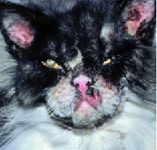
Figure 6. A 4-year-old cat with severe facial pruritus and secondary infections. Subsequent evaluation showed this was caused by adverse food reaction, and the cat was maintained long-term on a limited-antigen diet.
It is important to stress that canine and feline atopic dermatitis and adverse food reaction can present with identical clinical signs and may in fact be concurrent problems. Consequently, I perform a limited-antigen food trial in all animals with nonseasonal pruritus.
Diet selection
Traditionally, the identification of adverse food reaction has relied on feeding a novel protein source (one to which the animal has had little or no previous exposure). This novel protein is usually combined with a carbohydrate and may be fed as a commercial or home-cooked diet. As the variety of protein sources available in over-the-counter commercial pet foods has expanded, the choice of novel protein sources has become more limited. This and other factors have led to the recent development of balanced hydrolyzed protein diets.
In many cases, a commercial diet is selected over a home-cooked diet, as owner compliance is often better with commercial products. Confirmed reports of animals tolerating home-cooked diets and not the commercial equivalent containing similar ingredients are rare (eight dogs and one cat).14-16 Home-cooked diets are often advocated to avoid pet food additives that might have the potential to cause adverse reactions. However, although additives are often incriminated as causing adverse reactions in pets, there are no well-documented reports to support this idea. Forty dogs with adverse food reaction confirmed after being fed home-cooked diets could not subsequently tolerate commercial novel protein diets. However, no attempt was made to identify the problem allergen in those cases.17 Home-cooked diets should not be used at all in growing dogs or in cats for more than four weeks without being nutritionally balanced by an experienced veterinary nutritionist. In these cases, skeletal or organ pathology can result from a poorly balanced diet.
A number of commercial hydrolysate diets are available for both dogs and cats. In these diets, a common protein such as soy or chicken has been digested to produce smaller peptides. In theory, these peptides are too small to initiate an IgE-mediated reaction. The claim for efficacy in veterinary patients therefore assumes that most adverse food reactions in cats and dogs are IgE-mediated. Whether this is the case is currently unknown.

Tips to enhance dietary acceptance by the pet
A further limitation to the use of hydrolyzed diets as test diets is the lack of data documenting whether dogs allergic to the parent protein can tolerate the hydrolyzed product. Nestlé Purina Veterinary Diets HA HypoAllergenic Canine Formula (Nestlé Purina) containing hydrolyzed soy protein and cornstarch has been evaluated in two small studies of dogs with pruritic skin conditions. A randomized blind feeding study demonstrated a reduction in pruritus in soy-and corn-allergic dogs fed this diet of 50% and 80%, respectively.18 When HA Formula was fed to the Maltese-beagle dogs at North Carolina State University, 11 of 14 dogs (78.6%) with soy or corn allergy or both showed no adverse effects.7
However, regardless of whether you select a novel protein, hydrolyzed, or home-cooked diet, your choice of diet should be based on a thorough dietary history that should include not only the main diet but any frequently fed treats or table scraps. This will allow selection of a truly novel protein source. Cost and palatability are also major considerations for many clients (see the boxed text "Tips to enhance dietary acceptance by the pet").
Client compliance
Lack of client compliance is generally the biggest reason for the failure of dietary trials. Often, poor compliance is due to inadequate client education by the attending veterinarian. In fact, one study showed that before improved client education was initiated, 52% of diet trials failed during follow-up, compared with a failure rate of 27% after better client education was instituted.9
Owners must understand that the diet should be fed exclusive of all other foodstuffs. Either the veterinarian or veterinary technician must schedule time with the owner to explain the premise of the test and reasonable expectations from the procedure. It is also useful to provide handouts that detail the protocol. A follow-up visit after two to four weeks will identify any problems or indiscretions and is often needed to encourage the owner to maintain the trial protocol.
Concurrent therapies
It may be necessary to treat secondary complications of adverse food reaction such as superficial pyoderma, Malassezia dermatitis, and ear infections. Secondary complications do not preclude a dietary trial. In fact, if an animal truly has a food allergy, switching to a novel protein diet may actually enhance resolution of a pet's condition.
Under these circumstances, however, the animal should be assessed after three or four weeks to ensure antimicrobial therapy has been adequate. Pruritus typically will have diminished during this time as a result of controlling the secondary infections. The diet trial should be continued for another two to four weeks to demonstrate improvement is maintained before provocative challenge is performed.
How much allergen is too much?
The amount of allergen ingested that provokes an allergic reaction varies with allergen type and among individuals. This has been shown in the case of peanut allergy in people, and there are anecdotal reports of animals that appear to have adverse reactions to flavored medications. In our practice, we routinely prohibit chewable heartworm prophylactics, flavored antibiotics and vitamin tablets, and toothpaste during a diet trial. In an open study, the colony of Maltese-beagle dogs at North Carolina State University was intolerant of flavored milbemycin tablets containing soy and pork. As little as 200 mg/kg of corn (1 g of corn for a 11-lb [5-kg] dog) is sufficient to elicit an allergic reaction in susceptible individuals.7 Clients may better comprehend this small amount if you tell them it is less than the amount of corn in a single corn chip (Figure 7).
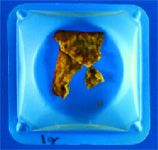
Figure 7. In some dogs with corn allergies, 1 g of nacho chip pieces is enough to trigger an allergic reaction.
Confirming a food allergy
Adverse food reaction is confirmed only when it has been demonstrated that the same clinical signs recur when previously fed foodstuffs are reintroduced. I usually recommend reintroducing the previously fed commercial diet first as 10% to 20% of total food for seven days. If this does not result in a relapse, then commonly fed treats can be reintroduced to determine whether these induce clinical signs. In my experience, gastrointestinal signs, if present, usually resolve first and may be the first to reappear after challenge in an animal with adverse food reaction.
How long it takes for dermatologic signs to reappear is a subject of debate. Most authors agree a patient should relapse between 24 hours and two weeks after challenge, although one recent trial reported that two dogs took up to three weeks to show signs.17 Another study reported a significant difference between dairy and cereal products, with patients showing signs 4.1 and 8.3 days after reintroduction, respectively.10 In most reported cases, time to relapse was reported by the owner (often by phone), and the patient was not examined immediately after the challenge by a veterinarian. Our experience with the Maltese-beagle dogs at North Carolina State University is that clinical signs of erythema may be seen as early as 15 minutes after challenge. If an animal fails to respond to a correctly performed diet trial, I often perform a second diet trial with a different diet to definitively rule out food allergy.

Golden rules for successful diet trials
Identifying specific food allergens
Between 35% and 60% of dogs are reported to be intolerant to more than one foodstuff, which underscores the need for challenge with multiple food sources.10,19,20 Most veterinary professionals agree that beef hypersensitivity has the greatest incidence in dogs in Europe and the United States. Similar information is not available in cats because owners have typically been reluctant to pursue provocative challenge.
Pets with concurrent allergies
As previously discussed, the incidence of concurrent atopic dermatitis and adverse food reaction is unknown in dogs and cats. However, some patients will have a history of year-round pruritus that worsens in the spring and summer. In these cases, it is important to consider the possibility of concurrent adverse food reaction, atopic dermatitis, or flea allergy dermatitis. Depending on the time of year the diet trial is initiated, these patients may not exhibit complete resolution of pruritus, but they should show some improvement with dietary restriction and relapse of pruritus on dietary challenge. Many dermatologists prefer to perform diet trials and challenge during the winter to avoid seasonal increases in pruritus due to environmental allergens, complicating interpretation of the diet trial.
ALTERNATIVE IDENTIFYING TESTS FOR FOOD ALLERGY
Unfortunately, no other reliable tests for identifying food allergies in pets are currently available. Various authors have looked at intradermal testing with food allergens and measurement of food-specific serum IgE. Although dogs with atopic dermatitis are more likely to have positive intradermal test reactivity to foodstuffs than are normal dogs,21 this test is unreliable for identifying food hypersensitivities.7,16 In addition, food-specific serum IgE measurement has not proved to have a useful degree of sensitivity for clinical diagnosis in its current form.7,16 Although these tests are commercially available, I do not recommend their use for diagnosing adverse food reaction in dogs and cats.
NUTRITIONAL MANAGEMENT OF PATIENTS WITH ADVERSE FOOD REACTIONS
Most patients can be managed long-term with a commercial limited-antigen or hydrolysate diet, and many owners elect to continue feeding the trial diet. Home-cooked diets must be balanced for long-term feeding. However, if specific allergens have been identified, it may be possible to extend the choice to diets readily available over the counter. An unanswered question is how often pets develop an allergy to the new diet. This is recognized in dermatologic practice and should be considered in patients that relapse. Typically, changing to an alternative diet with different protein and carbohydrate sources will resolve the clinical signs.
CONCLUSION
Clinical evidence suggests that adverse food reactions occur quite commonly in dogs and cats, and further research with animal models will help elucidate the pathogenesis. Nonetheless, in all animals with a nonseasonal pruritus, consider adverse reaction alone or concurrent with environmental hypersensitivities. With good client education, a valid diet trial confirmed with provocative challenge is a realistic undertaking. Dietary management offers a good long-term prognosis for affected dogs and cats.
Hilary A. Jackson, BVM&S, DVD, DACVD
Dermatology Referral Services
528 Paisley Road West
Glasgow G51 1RN, Scotland
REFERENCES
1. Leung DYM, Bieber T. Atopic dermatitis. Lancet 2003;361:151-160.
2. Jackson HA, Murphy KM, Tater KC, et al. The pattern of allergen hypersensitivity (dietary or environmental) of dogs with non-seasonal atopic dermatitis cannot be differentiated on the basis of historical or clinical information: a prospective evaluation 2003-2004. Vet Dermatol 2005;16:200.
3. de Weck AL, Mayer P, Stumper B, et al. Dog allergy, a model for allergy genetics. Int Arch Allergy Immunol 1997;113:55-57.
4. Ermel RW, Kock M, Griffey SM, et al. The atopic dog: a model for food allergy. Lab Anim Sci 1997;47:40-49.
5. Olson M, Hardin JA, Buret A, et al. Hypersensitivity reactions to dietary antigens in atopic dogs. In: Rheinhart GA, Carey DP, eds. Recent advances in canine and feline nutrition, Vol. 3. Wilmington, Ohio: Orange Frazer Press, 2000;69-77.
6. Jackson HA, Hammerberg B. Evaluation of a spontaneous canine model of immunoglobulin E-mediated food hypersensitivity: dynamic changes in serum and fecal allergen-specific immunoglobulin E values relative to dietary change. Comp Med 2002;52:316-321.
7. Jackson HA, Jackson MW, Coblentz L, et al. Evaluation of the clinical and allergen specific serum immunoglobulin E responses to oral challenge with cornstarch, corn, soy and a soy hydrolysate diet in dogs with spontaneous food allergy. Vet Dermatol 2003;14:181-187.
8. Rosser EJ Jr. Diagnosis of food allergy in dogs. J Am Vet Med Assoc 1993;203:259-262.
9. Chesney CJ. Food sensitivity in the dog: a quantitative study. J Small Anim Pract 2002;43:203-207.
10. Harvey R. Food allergy and dietary intolerance in dogs: a report of 25 cases. J Small Anim Pract 1993;34:175-179.
11. Carlotti D, Remy I, Prost C. Food allergy in dogs and cats. A review and report of 43 cases. Vet Dermatol 1990;1:55-62.
12. Guilford WG, Markwell PJ, Jones BR, et al. Prevalence and causes of food sensitivity in cats with chronic pruritus, vomiting or diarrhea. J Nutr 1998;128(12 suppl):2790S-2791S.
13. Guaguere E. Food intolerance in cats with cutaneous manifestations: a review of 17 cases. Pratique médicale et chirurgicale de l'animal de compagnie 1993;28:451-460.
14. White SD, Sequoia D. Food hypersensitivity in cats: 14 cases (1982-1987). J Am Vet Med Assoc 1989;194:692-695.
15. White SD. Food hypersensitivity in 30 dogs. J Am Vet Med Assoc 1986;188:695-698.
16. Jeffers JG, Shanley KJ, Meyer EK. Diagnostic testing of dogs for food hypersensitivity. J Am Vet Med Assoc 1991;198:245-250.
17. Leistra MHG, Markwell PJ, Willemse T. Evaluation of selected-protein-source diets for management of dogs with adverse reactions to foods. J Am Vet Med Assoc 2001;219:1411-1414.
18. Beale KM, Laflamme DP. Comparison of a hydrolyzed soy protein diet containing corn starch with a positive and negative control diet in corn- or soy-sensitive dogs (abst). Vet Dermatol 2001;12:237.
19. Paterson S. Food hypersensitivity in 20 dogs with skin and gastrointestinal signs. J Small Anim Pract 1995;36:529-534.
20. Jeffers JG, Meyer EK, Sosis EJ. Responses of dogs with food allergies to single-ingredient dietary provocation. J Am Vet Med Assoc 1996;209:608-611.
21. Kunkle G, Horner S. Validity of skin testing for diagnosis of food allergy in dogs. J Am Vet Med Assoc 1992;200:677-680.