Dermatology Update: A new look at ulcerative dermatosis of Shetland sheepdogs and rough collies
Ulcerative dermatosis of Shetland sheepdogs and rough collies is an inflammatory, erosive skin disorder of unknown etiology.
Ulcerative dermatosis of Shetland sheepdogs and rough collies is an inflammatory, erosive skin disorder of unknown etiology. When described in 1995, it was thought to be a variant of canine familial dermatomyositis.1 But in 2001, researchers compared the clinicopathologic findings in five Shetland sheepdogs and three rough collies with this syndrome with those in seven Shetland sheepdogs and one rough collie with dermatomyositis and found that the two diseases were distinct.2,3 First, ulcerative dermatosis of Shetland sheepdogs and rough collies tended to affect older dogs (the mean age of onset was 5 years), while dermatomyositis affected younger dogs (usually dogs less than 6 months old). Second, ulcerative dermatosis of Shetland sheepdogs and rough collies first occurred in the summer months in seven of the eight dogs, while the occurrence of dermatomyositis was not seasonal. Third, the histologic pattern of ulcerative dermatosis of Shetland sheepdogs and rough collies was a lymphocyte-rich interface dermatitis with vesiculation at the dermal-epidermal junction, while the histologic pattern of dermatomyositis was a cell-poor interface dermatitis with follicular atrophy.
The eight dogs with ulcerative dermatosis were presented for evaluation of serpiginous ulcers on their ventral abdomens, groins, and medial thighs (Figure 1).3 Ulcers were noted on the mucocutaneous junctions in six of the dogs, on the inner pinnae in five of the dogs, and in the oral cavity in three of the dogs. Extensive ulceration can also be seen with this disease, and secondary bacterial colonization, bacteremia, and sepsis were described in one dog.3
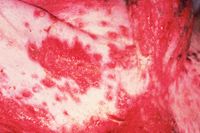
Figure 1 : Ulcerative lesions on a collie's ventral abdomen.
In contrast, the skin lesions associated with dermatomyositis often first develop on areas of mechanical trauma, such as the periocular region, tail tip, face, muzzle, ear tips, and tarsal regions.3 Although oral ulcers may occur, they are rare. The most commonly observed lesions in dogs with dermatomyositis are alopecia, erythema, scaling, and crusting. In some dogs with dermatomyositis, the lesions can be severe and ulceration can occur.
A recent study reported on the clinical treatment of and prognosis in 11 dogs with ulcerative dermatosis of Shetland sheepdogs and rough collies; eight of these dogs were from the 2001 study.4 Three of the 11 dogs were euthanized for reasons related to the disease; one of the three was euthanized before any therapy was initiated. In the remaining eight dogs, a variety of combination therapies were used, and eventually all dogs required systemic therapy. Of the dogs in which follow-up was reported, a 75% to 100% response was seen. The best long-term treatment was achieved with oral prednisone (2 mg/kg/day) and azathioprine (1 to 2 mg/kg/day). Prednisone was administered initially, and azathioprine was added for its corticosteroid-sparing effect or for additional immunosuppressive effects. All of the dogs receiving long-term systemic therapy experienced adverse effects and required long-term topical or systemic antibacterial treatment. Relapses were reported in subsequent summers. In short, this immune-mediated disease was chronic and somewhat debilitating but still manageable.
Commentary
Clinicians have long recognized ulcerative skin diseases in collies and Shetland sheepdogs. The differential diagnoses for ulcerative dermatoses involving the oral mucosa or axillary or inguinal regions include bullous pemphigoid, systemic lupus erythematosus, erythema multiforme, and pemphigus vulgaris. Making a definitive diagnosis can be difficult if no intact ulcers or vesicles are found. It has been suggested that ulcerative dermatosis of Shetland sheepdogs and rough collies be renamed canine vesicular cutaneous lupus erythematosus because of its similarities to a disease in people called subacute cutaneous lupus erythematosus.3-5
Regardless of the disease's name, it is important to recognize that the disease has a breed predilection and may appear similar to the other immune-mediated diseases mentioned above and be treated similarly with a combination of immunosuppressive therapies. The efficacy of cyclosporine in this disease is unknown. Systemic antibiotics are indicated if secondary bacterial colonization of the skin has occurred. Bacteremia and sepsis should be considered and addressed before you initiate immunosuppressive therapy.
This disease needs to be differentiated from other immune-mediated diseases, such as systemic lupus erythematosus, which could involve internal organs. A thorough diagnostic evaluation (medical and dermatologic) can help identify concurrent or potentially complicating problems. As with any immune-mediated disease, every effort should be made to determine a definitive diagnosis because it may affect the drug selection and prognosis.
REFERENCES
1. Ihrke, P.J.; Gross, T.L.: Ulcerative dermatosis of Shetland sheepdogs and collies. Kirk's Current Veterinary Therapy XII Small Animal Practice (J.D. Bonagura, ed.). W.B. Saunders, Philadelphia, Pa., 1995; pp 639-640.
2. Scott, D.W. et al.: Congenital and hereditary defects. Muller and Kirk's Small Animal Dermatology, 6th Ed. W.B. Saunders, Philadelphia, Pa., 2001; pp 913-1003.
3. Jackson, H.A.; Olivry, T.: Ulcerative dermatosis of the Shetland sheepdog and rough collie may represent a novel vesicular variant of cutaneous lupus erythematosus. Vet. Dermatol. 12 (1):19-27; 2001.
4. Jackson, H.A.: Eleven cases of vesicular cutaneous lupus erythematosus in Shetland sheepdogs and rough collies: Clinical management and prognosis. Vet. Dermatol. 15 (1):37-41; 2004.
5. Jackson, H.A. et al.: Immunopathology of vesicular cutaneous lupus erythematosus in the rough collie and Shetland sheepdog: A canine homologue of subacute cutaneous lupus erythematosus in humans. Vet. Dermatol. 15 (4):230-239; 2004.
"Dermatology Update" was contributed by Karen A. Moriello, DVM, DACVD, Department of Medical Sciences, School of Veterinary Medicine, University of Wisconsin, Madison, WI 53706.