The eyes have it: Conjunctivitis as a window to the body
What seems like simple conjunctivitis may indicate something more serious, with the eyes providing a view into possible systemic disease. Its also essential that veterinarians treat this common condition individually by species.
We've all experienced the discomfort of conjunctivitis, or “pinkeye.” Usually the red, itchy eyes are gone after a day or two, but they can persist, driving us to the doctor for medical relief. In humans, conjunctivitis is usually allergic or infectious in nature. Treatment ranges from simple over-the-counter or at-home remedies to prescriptions for antihistamines, antivirals or antibiotics to be applied topically or even taken orally.
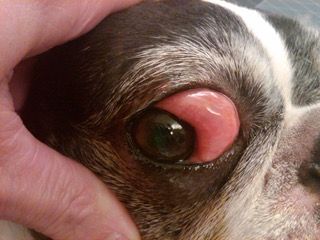
A 10-year-old Boston terrier that presented for a red eye. Note the swelling and redness of the conjunctiva. This was secondary to a cancerous tumor growing under the conjunctiva. A biopsy of the tissue revealed a mast cell tumor. The dog was sent to an oncologist and unfortunately had a poor prognosis for long-term survival. All photos courtesy of Dr. Brad Holmberg. We might assume that conjunctivitis in companion animals is also easily diagnosed and treated, but our patients' eyes can provide hints to other disorders in the body that are much more serious. Those may include inflammatory diseases, bleeding disorders or even cancer that first shows up on or in the eye.
By performing a thorough eye exam and complete diagnostics, we may find disease that will cause greater harm if allowed to go untreated. We must ensure that conjunctivitis is not a sign of something more serious.
One sign, many causes
Because every animal is different and every species has unique physiology, anatomy and immune responses, we need to assess each case individually. Conjunctivitis is very common in dogs and cats, but the underlying cause and treatment options can vary greatly. That means it's critical for us to diagnose correctly, know about the underlying causes and understand treatment options for each species.
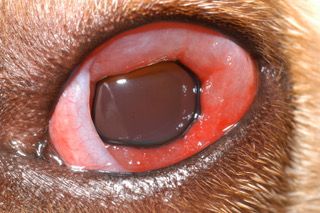
A 6-year-old Labrador retriever that initially presented to the referring veterinarian for a red left eye. After one day of treating with a triple antibiotic ointment, the conjunctivitis got much worse, with extensive redness and swelling as noted in the image. This is secondary to a toxic reaction to neomycin, a common antibiotic in several ophthalmic medications. Stopping the neomycin and treating with a topical corticosteroid anti-inflammatory helped resolve the clinical signs. The cause of the first-noticed conjunctivitis was unknown and suspected to be allergic.Dogs and cats often present with similar clinical signs during an exam, including red, puffy eyes and, frequently, ocular discharge. This discharge may be watery or it may have a mucoid or pus-like consistency. The type of discharge may suggest the underlying cause, but it's by no means definitive.
If a patient has had conjunctivitis for a day or two, that's fairly common and we may let it run its course. If it's been going on for several days and there's significant discharge, redness, squinting or cloudiness of the cornea, it's time for a thorough examination.
Diagnostic rundown
When I am presented with a dog or cat with clinical signs of conjunctivitis, I conduct a series of diagnostic tests to try to determine the underlying cause. These tests include measuring tear levels with a Schirmer tear test, performing tonometry to assess intraocular pressure to look for glaucoma, placing a special stain on the cornea to look for corneal ulceration and, most important, performing a thorough exam using slit lamp biomicroscopy.
This exam and the test results may definitively diagnose the cause of the conjunctivitis or suggest other causes, such as allergy or infection. If I suspect infectious conjunctivitis, I'll conduct further testing, including taking conjunctival samples, blood samples or both to confirm the presence of an infectious cause.
The canine window
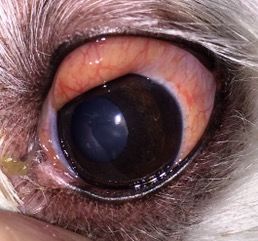
An 8-year-old mix-breed dog that presented for conjunctivitis. Note the swelling along the top of the eye with an orange-appearing mass effect. A tissue biopsy revealed lymphoma. Treatment by an oncologist involved oral and intravenous chemotherapy, which helped resolve the signs and prolonged the dog's life for several years.When dogs get conjunctivitis, it's most frequently allergic and rarely infectious. It may be a response to an irritant in the environment, such as pollen or dust. I see allergic conjunctivitis more often in allergy-prone breeds such as cocker spaniels and bulldogs. In these cases the pet may also show other signs of allergy, including paw licking, excessive scratching and red areas on the skin.
Dogs with simple allergic conjunctivitis can be treated with a topical antihistamine. In cases that don't respond, I question my diagnosis of simple allergic conjunctivitis and explore other causes further. If I don't find any, I may use a stronger topical anti-inflammatory, specifically a corticosteroid. Topical corticosteroids have been a mainstay of the treatment of conjunctivitis in dogs for decades.
Dogs can also have conjunctivitis due to concurrent corneal or intraocular disease. In these cases the conjunctivitis is not the primary abnormality but a sign of something else wrong with the eye. Possibilities include:
- An inappropriate tear film in dogs with dry eye
- Corneal ulceration in dogs that have sustained trauma to the cornea
- Glaucoma
- Intraocular inflammation.
If we treat these animals for simple conjunctivitis, we may delay treatment for the true underlying cause, which can result in permanent eye damage or vision loss.
The feline window
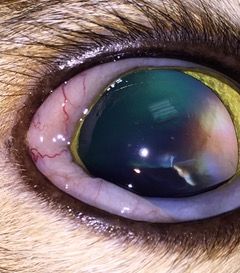
A 2-year-old cat with significant conjunctivitis secondary to Chlamydophila infection. Both eyes were affected. Treatment involved the use of an oral antibiotic, which cleared the infection and led to resolution of the conjunctivitis.Cats are quite different from dogs when it comes to conjunctivitis. They rarely get allergic conjunctivitis. Instead, most cases are infectious. The most common infectious agent is feline herpesvirus, but several bacteria can also be involved, including Chlamydophila, Bartonella and Mycoplasma species. Sometimes the clinical exam and history can differentiate among these causes. Other times, we have to perform additional laboratory testing to definitively diagnose the cause.
Herpesvirus is ubiquitous, with nearly all cats exposed at some point in life. Many cases of herpesviral conjunctivitis in cats are self-limiting, lasting just a few days. For cases that persist, antiviral therapy is the treatment of choice.
I used to recommend topical treatment exclusively. But while some cats tolerate this therapy well, it can be stressful for other patients-as well as their owners-especially when prescribed three to four times daily. Recently a new oral antiviral, famciclovir, has become available that is very effective at controlling herpesvirus and reducing associated clinical signs.
While the infectious organisms that cause conjunctivitis in cats can be transmitted from cat to cat, the development of clinical disease depends on a cat's immune system, the underlying cause and the cat's previous exposure to that pathogen. Fortunately, I don't often see an outbreak in groups of cats in multipet households-it's usually just one animal affected. However, in areas with high cat populations, such as shelters, it's common for numerous cats to be affected, especially those that are young or have a concurrent systemic disease that stresses the immune system.
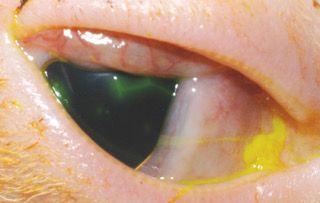
A 4-year-old cat that presented for squinting, discharge and redness of the right eye. Examination revealed significant inflammation of the conjunctiva. In addition, fluorescein stain applied to the cornea revealed a dendritic (linear, branching) superficial corneal ulcer. These signs are pathognomonic for feline herpesvirus. Topical and oral antiviral therapy led to resolution of the clinical signs.Because cats don't tend to get allergic conjunctivitis, corticosteroid medications are almost always contraindicated. In fact, using corticosteroids for common conjunctivitis in a cat may make the patient much worse. Instead I usually prescribe antivirals, either topically or systemically, and may recommend topical and oral antibiotics as well depending on the underlying cause.
A note on dogs: While antiviral and antibiotic therapy usually won't hurt in cases of conjunctivitis in dogs, they also may not help. The danger in dogs is missing the underlying cause in a dog and not treating appropriately-this can have profound long-term effects. This makes determining the most likely cause of conjunctivitis and choosing the right treatment for the species especially important.
Other window considerations
Conjunctivitis in all species can be quite irritating and cause significant discomfort. Many animals respond to this discomfort by rubbing or scratching at their eyes. As a result, I often see corneal ulcers, or secondary abrasions on the surface of the eye. Left untreated, these abrasions can get infected and possibly progress to perforation of the eye, leading either to emergency surgery or permanent blindness in that eye.
So what's the most important thing to remember about conjunctivitis? That it's not as simple as we might think. We should always use diagnostic testing to either rule out something more serious or confirm that the condition can be easily treated. Without that due diligence, we run the risk of allowing further harm to occur.
By following through with a proper examination, complete diagnostics and appropriate treatment of conjunctivitis, we can continue to use those “windows” to provide a unique look into the well-being of our patients and keep them healthy for years to come.
Dr. Brad Holmberg is a board-certified

veterinary ophthalmologist with extensive experience in the diagnosis and treatment of all animal eye diseases. He provides services at AERA's Animal Eye Center of New Jersey, a Compassion-First Pet Hospital.