A fresh look at identifying sepsis in cats
The incidence of sepsis in cats is unknown, partly because sepsis can be challenging to diagnose in cats.
The incidence of sepsis in cats is unknown, partly because sepsis can be challenging to diagnose in cats. Sepsis should be considered as a potential cause of illness in critically ill cats, whether they present in an emergency situation or are receiving medical care. Diagnosing sepsis in cats depends on maintaining a high index of suspicion and recognizing the risk factors and unique features of the feline response to sepsis. This article applies the recent sepsis classification scheme, PIRO,1 to diagnosing sepsis in cats.
Illustration by Melissa Galitz
DEFINING SEPSIS AND SIRS
At the 1991 American College of Chest Physicians/Society of Critical Care Medicine consensus conference,2 sepsis was defined as evidence of infection plus a clinical picture of systemic inflammatory response syndrome (SIRS)—SIRS being defined as the presence of two of the following clinical criteria: tachycardia, tachypnea, a fever or hypothermia, and leukocytosis or leucopenia.
Severe sepsis is sepsis with evidence of organ dysfunction and hypotension or hypoperfusion. Septic shock is severe sepsis with refractory hypotension.
SIRS LIMITATIONS
Almost any patient that comes into the emergency room will fulfill at least two of the SIRS criteria. Because of its lack of specificity, the definition of SIRS leaves much to be desired in both human and veterinary medical applications (Table 1). In published SIRS criteria recommended for dogs, the sensitivity ranges from 77% to 97% while the specificity is between 64% and 77%.3 No such study has been performed in cats.
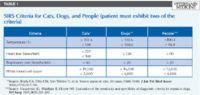
Table 1: SIRS Criteria for Cats, Dogs, and People
PIRO
In 2001, there was a second physicians' consensus conference,1 that expanded the criteria for SIRS by recommending the inclusion of physical parameters and biomarkers (measurable factors in blood or biological samples that can be used to identify or stage disease). Many of the parameters and some of the biomarkers may also prove useful in veterinary species. This newer approach, designated as PIRO, incorporates four factors in the stratification.
- Predisposition. Although many factors can influence susceptibility to disease, predisposing genetic factors are an area of active research in people. While it has long been recognized that certain dog or cat breeds or human families may be more susceptible to diseases than are other breeds or families, individual genetic variations or polymorphisms appear to further contribute to disease susceptibility. Other predisposing factors may be age, concurrent conditions, and sex.
- Infection. Clinically, we recognize that certain bacteria, location of infection, or extent of infection contribute to the risk of developing sepsis or septic shock.
- Response of the host. Our inability to readily identify and monitor biomarkers is the biggest limitation for this component of the stratification scheme. However, if we can determine whether a cat is in an excessively proinflammatory state vs. exhibiting immune paralysis or whether it has evidence of adrenal or coagulation dysfunction, we will be better able to choose appropriate and directed interventions.
- Organ dysfunction. The extent of organ dysfunction will negatively influence the outcome, even more so in cats than in people.
Predisposition
There does not seem to be a breed or sex predilection for sepsis in cats. Cats with pyothorax are more likely to come from multicat households and have a higher incidence of outdoor access.4 In one study of septic peritonitis, male cats outnumbered female cats.5 Diabetes mellitus is reported as a predisposing factor for hepatic abscesses in dogs and people, but no such predisposition has been reported in cats.6 Although there are no epidemiologic reports of the incidence of sepsis associated with immune suppression in cats, it is likely that immunosuppressive diseases, such as feline leukemia virus or feline immunodeficiency virus infection, and immune suppression associated with chemotherapy increase the predisposition for sepsis.
Infection
In a recent study evaluating the safety and efficacy of activated protein C in people with severe sepsis, the respiratory tract was the source of sepsis in more than half of the 1,690 patients.7 The gastrointestinal and urinary tracts were the other major sources, representing 20% and 10% of cases, respectively. No studies in companion animals report the cause of sepsis or the outcome in large populations.
In a study of severe sepsis in 29 cats, the most common causes of sepsis were pyothorax (24%), septic peritonitis (14%), endocarditis (14%), pyelonephritis (7%), osteomyelitis (3%), pyometra (3%), and bite wounds (3%).8 While there is no comparable study in dogs, the most commonly reported cause of sepsis is peritonitis.9-11 Reproductive organs (uterus, prostate) are also common sources of sepsis in dogs. In cats, pyothorax frequently occurs as an extension of pneumonia12 ; however, it appears that pyothorax may lead to sepsis more frequently than pneumonia leads to sepsis.8
Direct comparison of the response of cats to sepsis vs. the response of dogs is challenging. Few studies have provided the same diagnostic criteria or reflect the same basic population; however, several generalizations can be made regarding cats with sepsis. The first is that cats are more likely to have a hypodynamic response. In other words, they are likely to be hypothermic, pale, and bradycardic (heart rate < 140 beats/min; Table 1).8 Anemia is a common finding in septic cats.5,8 Hypoalbuminemia is common in septic dogs and cats.5,8,10
Most cases of sepsis are from bacteria of enteric origin, predominantly Escherichia coli. However, in cases of feline pyothorax, Pasteurella and Clostridium species predominate,4 and in the limited reports of endocarditis in cats, gram-positive bacteria and Bartonella species were the reported causes.13
In some cases of sepsis in cats, the source of infection is readily apparent, such as in cats with severe bite wounds, penetrating trauma, or infected wounds. However, in other cases, determining the source of infection can be more challenging. Potential sources of infection in cats include pneumonia, pyothorax, septic peritonitis, septic pancreatitis, pyelonephritis, bacteremia secondary to severe gastrointestinal disease, pyometra, hepatic abscesses, endocarditis, or meningitis.
In dogs and cats with septic peritonitis, the gastrointestinal tract is the most likely source of infection; however, there are some distinct differences. Cats are more likely to have intestinal neoplasia as a cause of peritonitis.5 Dogs appear more likely than cats to have gastric rupture (ulcers, gastric dilatation-volvulus).10,11 The reproductive organs are a more likely source of infection in dogs than in cats. Cats are more likely to have an undiagnosed source of peritonitis than dogs are5 ; however, a recent study of septic peritonitis in cats reported that trauma and the subsequent disruption of the gastrointestinal tract was an important cause.14
Response
Sepsis is generally more challenging to identify in cats than it is in dogs.8 Dogs classically present with signs similar to those in people: fever, tachypnea, tachycardia, and leukocytosis. Cats are frequently afebrile or hypothermic.8 Severe sepsis in cats can result in bradycardia rather than the expected tachycardia. Abdominal pain was a common physical examination finding in cats with severe sepsis but, curiously, not consistent in cats with septic peritonitis.5 Although hepatic abscesses are relatively uncommon, some reports describe their clinical features in dogs and cats. Cats with hepatic abscesses are less likely to be febrile, more likely to be hypothermic, and less likely to have increased liver enzyme activities.6
Biomarkers. Sepsis biomarkers are an area of active research in human medicine. Several studies have investigated biomarkers in dogs (protein C, endotoxin, tumor necrosis factor, C-reactive protein)9,15-17; however, there are no studies of biomarkers in clinically septic cats. In an experimental study in which cats were given low-dose endotoxin, rectal temperature increased, blood pressure decreased, and tumor necrosis factor activity and interleukin-6, interleukin-10, and chemokine CXCL-8 concentrations increased.18 In addition, white blood cell counts decreased and lactate, glucose, creatinine concentrations and prothrombin time increased.
Clinicopathologic findings in cats with sepsis are nonspecific. Leukocytosis is a variable finding in cats with sepsis, and anemia and hypoalbuminemia are typical findings.5 The pathogenesis of this anemia is complex and multifactorial. Factors such as frequent blood sampling, nutritional deficiencies, gastrointestinal blood loss, mechanical and antibody-mediated hemolysis, and renal or hepatic insufficiency may all play a role. Inflammatory mediators such as tumor necrosis factor and interleukin-1 inhibit erythroid precursor cells, reduce the formation of erythropoetin, and blunt the response of the bone marrow to erythropoetin.19 Feline erythrocytes are particularly susceptible to oxidative damage because the hemoglobin molecule has eight reactive sulfhydryl groups.20
Decreased plasma ionized calcium concentrations are frequently encountered in people with sepsis and have also been documented in septic cats.5,21 Etiologies identified in people include parathyroid gland suppression, inadequate vitamin D concentrations, and parathyroid hormone-vitamin D resistance, but the cause of these changes in patients with sepsis is still unknown.
The general pattern of glucose derangements in patients with acute sepsis consists of early and transient hyperglycemia followed by hypoglycemia. Cats are known to become hyperglycemic in response to stress, but hypoglycemia is often seen in septic cats.8 The factors thought to play a role in the development of hypoglycemia include increased peripheral glucose utilization, impaired gluconeogenesis, and depleted glycogen stores.
In cats with severe sepsis, hypoalbuminemia is common.5 The exact cause is unknown, but hepatic dysfunction, malnutrition, and the shifting of protein production from albumin to acute phase proteins all likely contribute. Hepatic dysfunction can be a serious sequela of sepsis. Blood supply to the liver is impaired in septic shock, resulting in a decrease in oxygen and nutrient delivery. Hepatic dysfunction can result in coagulopathies, mental depression, hypoalbuminemia, and hypoglycemia. Septic cats often have elevated serum bilirubin,5,8 so they may be overtly icteric on physical examination. Red blood cell lysis, sepsis-induced cholestasis, and hepatic dysfunction are thought to contribute to the development of hyperbilirubinemia in these cats.
Organ dysfunction
The lungs are often considered the shock organ in cats. As such, septic cats may be particularly susceptible to fluid overload, and pulmonary edema and pleural effusion are common. This pulmonary compromise occurs because of increased vascular permeability, sepsis-induced myocardial dysfunction, and decreased colloid oncotic pressure due to hypoalbuminemia. That differs from dogs, in which the liver and gastrointestinal tract are the primary shock organs.
DIAGNOSTIC TESTS
Initial diagnostic tests in cases of septic cats generally consist of a complete blood count, a serum chemistry profile, a urinalysis and culture, thoracic and abdominal radiography, and abdominal ultrasonography. Additional diagnostic tests may include blood bacterial cultures, an endotracheal wash and culture, echocardiography, a cerebrospinal fluid tap, or diagnostic peritoneal lavage.
TREATMENT
The goal when treating septic cats is the same as when treating any other critically ill patient: Maximize perfusion and oxygen delivery to the tissues. Cardiac output is calculated as heart rate x stroke volume. Stroke volume can be improved by maximizing preload with fluid administration. The shock bolus in cats is 50 to 60 ml/kg of crystalloid fluids or 5 ml/kg of colloids given intravenously. Start with small crystalloid boluses of 10 to 20 ml/kg given to effect (normalization of blood pressure or central venous pressure).
Drug therapy
In cats that remain hypotensive despite adequate volume replacement and normothermia, exogenous catecholamine therapy may be necessary. Dopamine (2.5 to 15 µg/kg/min intravenously) is a vasopressor with positive inotropic, chronotropic, and vasoconstrictive effects. It is often the first-line drug given to septic cats. At low doses (0.5 to 5 µg/kg/min), dopamine leads to renal vasodilation in dogs; cats lack dopaminergic receptors in their kidneys.22 In cats, dopamine is used predominantly for its beta-adrenergic effects leading to positive inotropy at 2.5 to 10 µg/kg/min and its alpha-adrenergic effects leading to vasoconstriction at > 10 µg/kg/min.22,23 Dobutamine also exhibits positive inotropic and chronotropic effects and improves cardiac output and oxygen delivery in experimental models of sepsis. Cats treated with dobutamine (at continuous infusions between 2 and 20 µg/kg/min intravenously) should be observed closely as seizures may occur in cats treated with dobutamine continuous rate infusions for more than 24 hours.24 In cats with severe hypotension or those that fail to respond to dopamine or dobutamine, norepinephrine (0.1 to 3 µg/kg/min intravenously) or epinephrine (0.1 to 2 µg/kg/min intravenously) are often effective. Vasopressor drugs are administered as a continuous infusion, and the dose is adjusted according to the physiologic response (i.e. blood pressure, heart rate). As the cat is able to maintain its blood pressure, the dose is reduced until the infusion can be discontinued.
Supplemental oxygen
Supplemental oxygen is often necessary in septic cats. Increased inspired oxygen can improve oxygen saturation (SpO2) as well as the partial pressure of oxygen in the blood (PaO2), thereby improving oxygen delivery to the tissues. As discussed previously, fluid overload and pulmonary edema are common in septic cats. Inflammatory lung disease (acute respiratory distress syndrome) and pneumonia can also contribute to hypoxia and decreased oxygen delivery. In most cats, treatment in an oxygen cage or oxygen administration by mask is sufficient, but in severe cases, positive pressure ventilation may be necessary.
Blood transfusion
Septic cats are often anemic and may have a coagulopathy. Administering red blood cells to an anemic patient improves the oxygen-carrying capacity of the blood and, thus, improves oxygen delivery to tissues. In addition, replacing coagulation factors by administering plasma minimizes further blood loss and provides colloidal support. Consider a red blood cell transfusion in any septic cat with clinical signs of decreased oxygen delivery (tachypnea, tachycardia or bradycardia, pale gums) and with a packed cell volume < 20. Administer plasma to cats with prolonged coagulation times. Cats with type B blood have autoantibodies to type A blood,25 so blood typing is essential before any blood transfusion. Cats that have been previously transfused should also only be transfused with blood to which they have been crossmatched.
Antibiotics
Appropriate antibiotic therapy is an integral part of the treatment of septic cats. In people, inadequate antimicrobial therapy has been associated with increased mortality.26 Use bacterial cultures and antimicrobial sensitivity testing to identify effective antibiotics. Administer broad-spectrum intravenous antibiotics pending antimicrobial sensitivity test results. The empiric selection of the initial antibiotic can be guided by the most likely source of sepsis and the commonly associated bacteria. For example, in septic peritonitis, enteric bacteria are the typical source of infection, so gram-negative coverage (e.g. a fluoroquinolone, third-generation cephalosporin, or aminoglycoside) and anaerobic coverage (e.g. metronidazole or penicillins) should be considered. All antibiotic choices must consider the tissue penetration, route of administration, toxicity profile, and origin of infection (i.e. community acquired or nosocomial), so they should be individualized for each patient.
Source control
A critical component of treating the septic patient is removal of the source of infection. Surgical resection of infected tissue is essential. In the case of feline pyothorax, however, placement of thoracostomy tubes to allow lavage and drainage is effective.12
Nutritional support
Nutritional support is extremely important in septic patients. The systemic inflammatory response in septic cats results in a catabolic state that can rapidly result in severe nutritional deficiency. Nutritional needs should be addressed early in the course of hospitalization. This support can be provided enterally by a nasoesophageal, esophagostomy, or percutaneous endoscopic gastrostomy tube if the patient is not vomiting and is normothermic. In cats that cannot tolerate enteral feeding, total parenteral nutrition may be necessary.
Recent studies in people have shown that maintaining normoglycemia significantly improves the outcome in some critically ill patients.27 Many septic cats are hypoglycemic on presentation, and higher mortality may be associated with hypoglycemia than with hyperglycemia. However, during hospitalization, particularly in patients receiving total parenteral nutrition, you must carefully monitor for hyperglycemia and treat with low doses of insulin when appropriate.
Pain management
Pain management is also important in patients with sepsis. Pain can be difficult to recognize in veterinary patients, particularly in critically ill cats. The severity of illness in these cases often results in a reluctance to treat with analgesic agents. Untreated pain in these cats leads to depression, inappetence or anorexia, decreased mobility, and an increase in stress hormones. Appropriately administering analgesics is an essential part of appropriately managing septic cats.
Depending on the case, analgesia can be maintained with either local (nerve blocks, epidural analgesia) or parenteral analgesics. In septic cats, nonsteroidal anti-inflammatory drugs carry a high risk of renal damage and should be avoided. Constant-rate infusions of analgesics may be helpful to maintain adequate pain control. Common analgesics that can be used in critically ill cats include buprenorphine (1 to 3 µg/kg/hr or 0.005 to 0.02 mg/kg intravenously or intramuscularly every four to eight hours), butorphanol (0.1 to 0.4 mg/kg intramuscularly or subcutaneously every one-and-a-half to four hours), fentanyl (2 to 4 µg/kg/hr), and morphine or methadone (0.1 to 0.5 mg/kg intramuscularly or subcutaneously every two to six hours).28-30
Corticosteroids
Corticosteroid use in the treatment of sepsis and septic shock has been an area of controversy since the 1950s. Although placebo-controlled trials failed to document beneficial effects of high-dose corticosteroids for the treatment of septic shock in people, recent studies have suggested that some septic human patients may benefit from physiologic doses of corticosteroids.31 A study evaluating adrenal function in critically ill cats with a variety of disease processes failed to document adrenal insufficiency in any of the patients.32 It is important to note that the low number of septic cats in this study (n=3) limits the conclusions that may be drawn and warrants further investigation.
In people, the recommendation is to administer replacement doses of glucocorticoids in patients with refractory septic shock. Without further investigation, this recommendation cannot be made in cats.
CONCLUSION
Cats with sepsis can be challenging to identify. Unlike dogs and people, cats often present with bradycardia and hypothermia. Although the prognosis in sepsis for any species is guarded, early recognition, early institution of appropriate antibiotics, and supportive care to maintain perfusion and function of key organs have been recognized as critical components of therapy.
To continue to make progress in the treatment of cats with sepsis, ongoing research is necessary to identify 1) additional predisposing factors, 2) the types of infections and their evolving antibiotic sensitivity, and 3) the unique features of cats' response to sepsis that can be used in the diagnosis and prognosis. Prospective clinical trials are also needed to optimize organ support and survival in cats with sepsis.
Cynthia M. Otto, DVM, PhD, DACVECC
Department of Clinical Studies
School of Veterinary Medicine
University of Pennsylvania
Philadelphia, PA 19104
Merilee Costello, DVM, DACVECC
Allegheny Veterinary Emergency Trauma & Specialty
4224 Northern Pike
Monroeville, PA 15146
REFERENCES
1. Levy MM, Fink MP, Marshall JC, et al. 2001 SCCM/ESICM/ACCP/ATS/SIS international sepsis definitions conference. Intensive Care Med 2003;29(4):530-538.
2. American college of chest physicians/society of critical care medicine consensus conference: definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Crit Care Med 1992;20(6):864-874.
3. Hauptman JG, Walshaw R, Olivier NB. Evaluation of the sensitivity and specificity of diagnostic criteria for sepsis in dogs. Vet Surg 1997;26(5):393-397.
4. Waddell LS, Brady CA, Drobatz KJ. Risk factors, prognostic indicators, and outcome of pyothorax in cats: 80 cases (1986-1999). J Am Vet Med Assoc 2002;221(6):819-824.
5. Costello MF, Drobatz KJ, Aronson LR, et al. Underlying cause, pathophysiologic abnormalities, and response to treatment in cats with septic peritonitis: 51 cases (1990-2001). J Am Vet Med Assoc 2004;225(6):897-902.
6. Sergeeff JS, Armstrong PJ, Bunch SE. Hepatic abscesses in cats: 14 cases (1985-2002). J Vet Intern Med 2004;18(3):295-300.
7. Bernard GR, Vincent JL, Laterre PF, et al. Efficacy and safety of recombinant human activated protein C for severe sepsis. N Engl J Med 2001;344(10):699-709.
8. Brady CA, Otto CM, Van Winkle TJ, et al. Severe sepsis in cats: 29 cases (1986-1998). J Am Vet Med Assoc 2000;217(4):531-535.
9. de Laforcade AM, Rozanski EA, Freeman LM, et al. Serial evaluation of protein C and antithrombin in dogs with sepsis. J Vet Intern Med 2008;22(1):26-30.
10. King LG. Postoperative complications and prognostic indicators in dogs and cats with septic peritonitis: 23 cases (1989-1992). J Am Vet Med Assoc 1994;204(3):407-414.
11. Bentley AM, Otto CM, Shofer FS. Comparison of dogs with septic peritonitis: 1988-1993 versus 1999-2003. J Vet Emerg Crit Care 2007;17(4):391-398.
12. Barrs VR, Allan GS, Martin P, et al. Feline pyothorax: a retrospective study of 27 cases in Australia. J Feline Med Surg 2005;7(4):211-222.
13. Malik R, Barrs VR, Church DB, et al. Vegetative endocarditis in six cats. J Feline Med Surg 1999;1(3):171-180.
14. Parsons KJ, Owen LJ, Lee K, et al. A retrospective study of surgically treated cases of septic peritonitis in the cat (2000-2007). J Small Anim Pract 2009;50(10):518-524.
15. de Laforcade AM, Freeman LM, Shaw SP, et al. Hemostatic changes in dogs with naturally occurring sepsis. J Vet Intern Med 2003;17(5):674-679.
16. Gebhardt C, Hirschberger J, Rau S, et al. Use of C-reactive protein to predict outcome in dogs with systemic inflammatory response syndrome or sepsis. J Vet Emerg Crit Care 2009;19(5):450-458.
17. Otto CM, Drobatz K, Soter C. Endotoxemia and tumor necrosis factor activity in dogs with naturally occurring parvoviral enteritis. J Vet Intern Med 1997;11(2):65-70.
18. DeClue AE, Williams KJ, Sharp C, et al. Systemic response to low-dose endotoxin infusion in cats. Vet Immunol Immunopathol 2009;132(2-4):167-174.
19. Moldawer LL, Marano MA, Wei H, et al. Cachectin/tumor necrosis factor-alpha alters red blood cell kinetics and induces anemia in vivo. FASEB J 1989;3(5):1637-1643.
20. Harvey JW, Kaneko JJ. Oxidation of human and animal haemoglobins with ascorbate, acetylphenylhydrazine, nitrite, and hydrogen peroxide. Br J Haematol 1976;32(2):193-203.
21. Holowaychuk MK, Martin LG. Review of hypocalcemia in septic patients. J Vet Emerg Crit Care 2007;17(4):348-358.
22. Wohl JS, Schwartz DD, Flournoy WS, et al. Renal hemodynamic and diuretic effects of low-dosage dopamine in anesthetized cats. J Vet Emerg Crit Care 2007;17(1):45-52.
23. Pascoe PJ, Ilkiw JE, Pypendop BH. Effects of increasing infusion rates of dopamine, dobutamine, epinephrine, and phenylephrine in healthy anesthetized cats. Am J Vet Res 2006;67(9):1491-1499.
24. Pachtinger GE, Drobatz K, Assessment and treatment of hypovolemic states. Vet Clin North Am Small Anim Pract 2008;38(3):629-643.
25. Bücheler J, Giger U, Alloantibodies against A and B blood types in cats. Vet Immunol Immunopathol 1993;38(3-4):283-295.
26. Dellinger RP, Levy MM, Carlet JM, et al. Surviving sepsis campaign: international guidelines for management of severe sepsis and septic shock: 2008. Crit Care Med 2008;36(1):296-327.
27. Van Den Berghe G, Wouters P, Weekers F, et al. Intensive insulin therapy in critically ill patients. N Engl J Med 2001;345(19):1359-1367.
28. Hansen B. Analgesia for the critically ill dog or cat: an update. Vet Clin North Am Small Anim Pract 2008;38(6):1353-1363.
29. Dyson DH. Analgesia and chemical restraint for the emergent veterinary patient. Vet Clin North Am Small Anim Pract 2008;38(6):1329-1352.
30. Robertson SA. Assessment and management of acute pain in cats. J Vet Emerg Crit Care 2005;15(4):261-272.
31. Annane D, Bellissant E, Bollaert PE, et al. Corticosteroids in the treatment of severe sepsis and septic shock in adults: a systematic review. JAMA 2009;301(22):2362-2375.
32. Prittie JE, Barton LJ, Peterson ME, et al. Hypothalamo-pituitary-adrenal axis function in critically ill cats, in Proceedings. 9th Int Vet Emerg Crit Care Symp 2003:771.