Identifying and treating 3 tick-borne diseases in dogs
Diagnosis of canine tick-related disease has been occurring with greater frequency, making knowledge of all tick-borne diseases increasingly important. This detailed overview of anaplasmosis, ehrlichiosis and Rocky Mountain spotted fever will help you be prepared when these diseases make an appearance in your veterinary clinic.

Shutterstock.com
Anaplasmosis, ehrlichiosis and Rocky Mountain spotted fever (RMSF) are three tick-borne diseases commonly diagnosed in dogs. Ehrlichiacanis, Ehrlichia chaffeensis and Ehrlichia ewingii cause ehrlichiosis. These organisms belong to the family Anaplasmataceae along with Anaplasma platys and Anaplasma phagocytophilum, which cause anaplasmosis. RMSF is caused by the organism Rickettsia rickettsii (Table 1, below).
With any of these diseases, co-infections with more than one type of tick-borne organism is possible, potentially altering the signs of illness in the affected patient. It is also possible for patients to be infected with any of these tick-borne diseases but have a predominance of signs related to co-existing non-tick-borne disease.
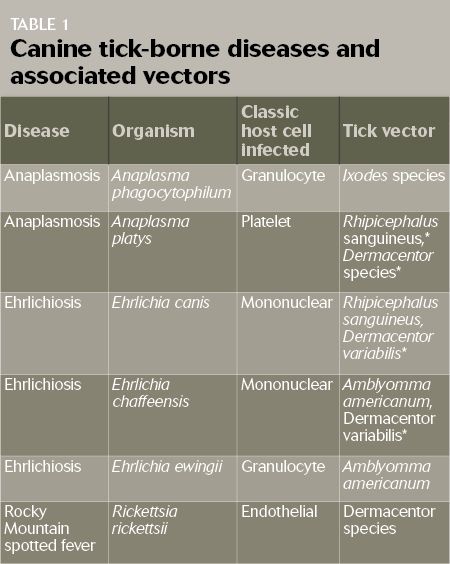
*Suspected tick vector
Geographic distribution
The organisms causing ehrlichiosis and RMSF have been reported in various parts of the United States. These organisms and related diseases are commonly reported in dogs from southeastern (E. canis, E. chaffeensis, E. ewingii, R. rickettsii), south-central (E. chaffeensis, E. ewingii, R. rickettsii), southwestern (E. canis), south Atlantic (R. rickettsii), and mid-Atlantic (E. chaffeensis) states.1 The fact that E. canis may produce a subclinical chronic disease phase can alter the typical geographic distribution since an infection may not be diagnosed until the animal manifests clinical signs after being transported to a nonendemic area. Anaplasmaphagocytophilum has an increased geographic presence on the west coast and in the northeast and upper midwest of the United States. Although the intermediate hosts and tick vectors of A. platys have not been fully confirmed, the organism could potentially have a widespread distribution in the United States in association with the suspected tick vectors.
The prevalence of tick-borne disease in any particular region is dependent upon multiple factors, including the presence of associated intermediate hosts and tick vectors as well as elements such as weather conditions. Diagnosis of ehrlichiosis, anaplasmosis and RMSF in the United States has increased over the last several years. It is possible that the rise in diagnosis of these tick-borne diseases could be the result of an increase in the overall population of the associated tick vectors and/or spread of tick vectors into previously nonendemic areas. However, elevated awareness of these tick-borne diseases and improved diagnostic methods could also contribute to the increase in the number of positive canine cases. To more accurately determine the prevalence of canine ehrlichiosis and anaplasmosis down to the county level of individual states, veterinarians can consult the Companion Animal Parasite Council website (www.capcvet.org), which provides user-friendly parasite prevalence maps as well as other up-to-date information about tick-borne diseases.
Signalment
Anaplasmosis and RMSF do not appear to have an age, breed or sex predisposition. However, E. canis seems to have a predilection for infecting German shepherds.
History and clinical signs
Dogs with anaplasmosis, ehrlichiosis or RMSF often have a history of tick exposure. Petechiae or ecchymoses may be observed in patients with these diseases.
Rocky Mountain spotted fever and ehrlichiosis. Other historical signs frequently reported with RMSF and ehrlichiosis are lethargy, hyporexia or anorexia, weight loss, lameness with neurologic abnormalities, tissue swelling, epistaxis, ocular and nasal discharge, and dyspnea.
Physical examination of patients with ehrlichiosis or RMSF can reveal evidence of the historical signs listed above as well as fever; muscle, neck, or joint pain; generalized lymphadenopathy; splenomegaly; icterus; and pale mucous membranes. The tissue swelling mentioned as a potential historical finding may be identified on physical examination as joint swelling or edema of the face, limbs, ventral body, scrotum or prepuce.
Erythematous skin lesions or necrotic lesions involving the distal extremities, ear margins or nasal planum may be found in some of these patients, especially in RMSF cases.
A variety of ocular lesions can be present, including serous to mucopurulent discharge, conjunctivitis, anterior uveitis and evidence of a primary hemostatic defect in the form of hyphema or conjunctival, scleral or retinal petechiation or hemorrhage.
Neurologic abnormalities such as vestibular or cerebellar signs (e.g. head tilt, ataxia, nystagmus, tremors, paresis, stupor, seizures, hyperesthesia and various cranial nerve deficits) can be observed.
Anaplasmosis. Patients infected with A. phagocytophilum most commonly have lethargy associated with fever and musculoskeletal pain. Patients infected with A. platys typically do not show any systemic signs of illness but occasionally may have mild fever, uveitis, petechiae or ecchymoses.
Seasonality
Patients with ehrlichiosis, anaplasmosis and RMSF most frequently present from the spring through early fall in association with the activity of the tick vectors. However, tick season can extend into late fall or even last year-round in some areas depending on the climate. Patients that have been infected with E. canis may be admitted for clinical signs throughout the year because of the various clinical phases (acute, subclinical, chronic) of E. canis.
Diagnostic tests
Complete blood count. The most consistent laboratory abnormality found in patients with ehrlichiosis, anaplasmosis or RMSF is thrombocytopenia, although its absence does not rule out these tick-borne diseases. Thrombocytopenia generally ranges from mild to moderate, with more severe deficits sometimes occurring in dogs with ehrlichiosis or RMSF.
Patients with ehrlichiosis or RMSF may have a variety of other complete blood count abnormalities, including mild to moderate anemia, which is most often nonregenerative. However, antibody formation against platelets or red blood cells can occasionally occur, resulting in more severe thrombocytopenia or regenerative anemia, which may be Coombs positive.
Although normal white blood cell counts can occur in patients with ehrlichiosis and RMSF, leukocytosis occurs commonly in patients with RMSF. Leukocytosis can occur with ehrlichiosis, but leukopenia can occur in patients infected with Ehrlichia species as well. Lymphopenia and monocytosis are abnormalities sometimes seen with both ehrlichiosis and RMSF, although patients with ehrlichiosis will occasionally have lymphocytosis. Chronic ehrlichiosis can result in pancytopenia.
Coagulation profile. Other than thrombocytopenia, the results of coagulation profiles may be normal or show additional changes consistent with disseminated intravascular coagulation, such as increased fibrinogen degradation products or D-dimers and prolonged activated partial thromboplastin time and, less commonly, prolonged prothrombin time.
Serum chemistry profile. Serum chemistry profile abnormalities are uncommon in patients with anaplasmosis but can be frequent and varied in patients with ehrlichiosis or RMSF. Protein abnormalities are commonly associated with both ehrlichiosis and RMSF, with hypoalbuminemia common in patients with either disease. Ehrlichiosis, particularly chronic ehrlichiosis, may produce hyperglobulinemia that is usually a polyclonal gammopathy but can, on rare occasion, be a monoclonal gammopathy. Liver (alkaline phosphatase, alanine transaminase, bilirubin) and renal (blood urea nitrogen, creatinine) serum chemistry values are often elevated in dogs with RMSF or ehrlichiosis.
Urinalysis. Urinalysis may reveal proteinuria in patients with ehrlichiosis, especially in chronic cases in which glomerulopathy may be a consequence of the disease process. Proteinuria may also be found in patients with RMSF, but in these patients, the protein is often accompanied by hematuria and pyuria produced by the underlying inflammatory disease without the associated bacterial infection. Bilirubinuria may be observed in patients with RMSF and should raise the index of suspicion for this disease when other compatible clinical findings are present.
Cerebrospinal fluid analysis. In patients with neurologic signs, cerebrospinal fluid analysis may show inflammatory pleocytosis and increased protein.
Bone marrow aspiration. Bone marrow aspiration may be indicated in patients with suspected ehrlichiosis exhibiting nonregenerative anemia, pancytopenia or monoclonal gammopathy determined through serum protein electrophoresis. Megakaryocytic hyperplasia is a characteristic of bone marrow aspirates from patients with acute ehrlichiosis. Bone marrow aspirates from patients with chronic ehrlichiosis are often characterized by generalized hypoplasia of cell lines together with plasmacytosis.
Radiography. In patients with ehrlichiosis or RMSF, abdominal radiography typically reveals hepatomegaly and splenomegaly. Thoracic radiography commonly reveals diffuse pulmonary interstitial infiltrates.
Cytology and serology. A more specific diagnosis of infection with R. rickettsii or an Anaplasmataceae organism is most commonly made through cytologic identification and antibody and polymerase chain reaction (PCR) assays.
For anaplasmosis and ehrlichiosis, an in-house ELISA serologic screening test (SNAP 4Dx Plus-IDEXX) is available for A. phagocytophilum, A. platys, E. canis and E. ewingii. An antibody against the Anaplasma and Ehrlichia genera can be detected with the screening test and is designated as positive (detectable) or negative (not detectable). A positive result would ideally be followed up with PCR testing of blood or tissue for specific species DNA or by serologic antibody titers, both of which are available at multiple diagnostic laboratories. The presence of an antibody only indicates that exposure to the associated organism has occurred and not that active infection is present.
A four-fold rise in antibody titer determined by assessment three or four weeks after an initial low to negative titer or a single high antibody titer, especially after more than four weeks of illness, is a strong indication of active infection (the level compatible with infection varies by laboratory and test methodology). The detection of organism-associated DNA is also a strong indication of infection, realizing that the lack of detection of DNA may be associated with an inadequate specimen, recent antibiotic therapy or a low circulating level of infecting organisms.
Cytologic evaluation of blood smears, fine-needle aspirates or tissue samples may reveal the presence of morulae (aggregations of infecting organisms) in patients with ehrlichiosis or anaplasmosis (See Table 1 for classic cell type infected). Although the presence of morulae is indicative of infection, low levels of circulating organisms or, in some cases, the cell types carrying the organisms, make the probability of identifying morulae relatively low.
For RMSF, identification of R. rickettsii infection is most commonly accomplished by antibody and PCR assay through diagnostic laboratories. Although both IgM and IgG antibody concentrations can be determined by some of the assay methods, IgG titers are the type most laboratories measure. As with the Anaplasmataceae organisms, it is difficult to distinguish exposure from active infection based on titer results alone. The same guidelines previously mentioned for the use of titers in determining active infection apply to diagnosing RMSF as well.
Direct fluorescent antibody tissue staining can be used to diagnose RMSF from skin lesions or other affected tissue. Such testing is best done early in the disease course since the infecting organisms disappear quickly from the tissues, especially once therapy has been initiated. A PCR assay performed on a patient's blood or tissue is commonly used to identify R. rickettsii and obtain a diagnosis.
Definitive diagnosis
When reaching a diagnosis of one of these tick-borne diseases, consider the patient's history, physical examination findings and diagnostic test results together. Co-infection with other tick-borne organisms is common, increasing the difficulty of making a clear-cut diagnosis and potentially increasing the degree of patient morbidity.
Response to appropriate treatment is also an important aspect of establishing a presumptive diagnosis of tick-borne disease. A therapeutic trial may be indicated in an at-risk patient prior to receiving results of serology or PCR testing and can also be helpful in identifying potentially infected patients with equivocal or false negative test results due to an early disease phase, previous treatment, or a low circulating level of organisms.
Treatment
Treating ehrlichiosis, anaplasmosis and RMSF centers around appropriate antimicrobial administration and adjunctive or supportive care. Doxycycline is the mainstay of antimicrobial treatment. Table 2 lists suggested dosages for doxycycline and alternative antimicrobial drugs recommended for therapy.
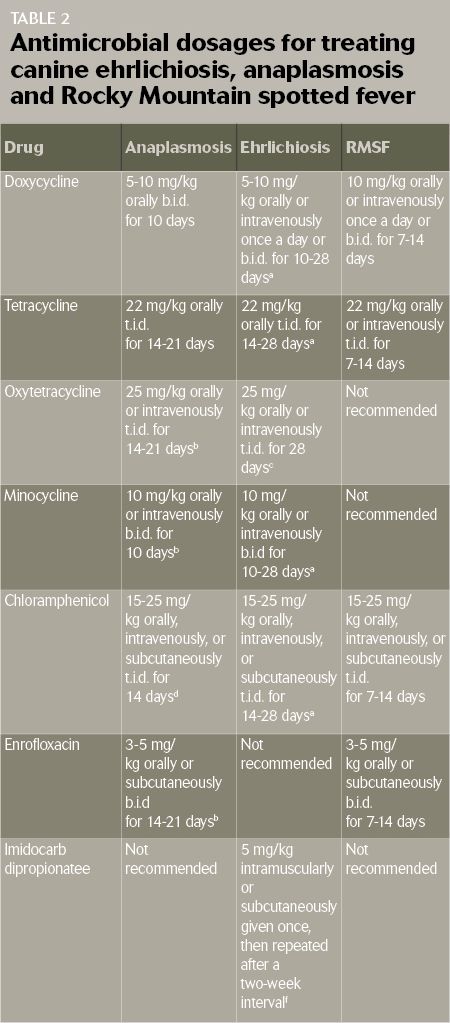
aRecommended minimum duration of treatment for Ehrlichia canis infection is 28 days. bRecommended for the treatment of Anaplasma platys only. cRecommended for the treatment of Ehrlichia canis and Ehrlichia chaffeensis only. dRecommended for the treatment of Anaplasma phagocytophilum only. ePretreat with atropine or glycopyrrolate intramuscularly or subcutaneously 20 minutes before giving imidocarb to prevent cholinergic signs. fRecommended for the treatment of Ehrlichia canis only; variable efficacy.
Adjunctive or supportive therapy can vary widely, depending on the organ systems affected and associated clinical signs. Patients that exhibit neurologic signs, hemolytic anemia, severe thrombocytopenia, edema, joint swelling or muscle pain frequently require high anti-inflammatory or immunosuppressive doses of corticosteroids initially (prednisone/prednisolone at 1 to 2.2 mg/kg/day orally; dexamethasone sodium phosphate at 0.15 to 0.35 mg/kg every 48 hours intravenously until oral prednisone can be given) in combination with an appropriate antimicrobial drug to achieve timely resolution of these more critical or uncomfortable aspects of infection. After the patient receiving corticosteroids starts to show clinical signs of improvement, the corticosteroid dose can be rapidly tapered while monitoring for any signs of relapse. In severely affected patients, nutritional and fluid support may be needed. Patients with severe anemia may require a blood transfusion.
Treatment response
The prognosis for most affected dogs is good if treatment is initiated early in the disease course. Clinical improvement for the tick-borne diseases discussed here often occurs within a few days to weeks of initiating appropriate therapy. Hyperglobulinemia may take several months to normalize. Severe glomerulopathy and bone marrow suppression may improve slowly but may never improve in some cases. Patients with suspected RMSF that have clinical signs persisting for longer than two weeks after initiating therapy should be reassessed for a different disease.
Resolution of clinical signs does not always mean that the infection has been eradicated. Decreasing antibody titers would reinforce the likelihood that treatment could be discontinued. However, antibody titers for most of the Anaplasmataceae and RMSF organisms, especially E. canis, often remain high for several months in spite of successful treatment of the associated disease. A negative PCR assay result on a specimen obtained at least two weeks after discontinuing antibiotic therapy would be a good indication that the organism had been successfully eradicated.
Reinfection
Rechecking patients periodically after apparent successful treatment, including performing pertinent diagnostic tests such as a platelet count, is an important method of not only detecting a relapse but also monitoring for reinfection. Resolving an episode of tick-borne infection does not confer immunity to reinfection (with the possible exception of dogs that have recovered from RMSF). Owners should be instructed to watch for recurrence of clinical signs and to practice diligent tick prevention.
Periodic antimicrobial treatment of dogs in areas highly endemic for organisms causing ehrlichiosis or anaplasmosis may be considered, especially for hunting dogs that are at greater risk for ongoing tick exposure. You can also consider low-dose daily therapy with doxycycline (3 mg/kg orally once a day) during tick season.
Reference
1. Sykes JE: Ehrlichia, anaplasmosis, Rocky mountain spotted fever, and Neorickettsia infection. In: Ettinger SJ, Feldman EC, eds. Textbook of veterinary internal medicine. 7th ed. Philadelphia: Saunders Elsevier, 2010;901-909.
Mary Bowles, DVM, DACVIM, emeritus associate professor, recently retired after a 40-year career as a clinician in the Department of Veterinary Clinical Sciences, Center for Veterinary Health Sciences, Oklahoma State University in Stillwater, Oklahoma.