Initially treating fading puppies and kittens
Timely treatment of ill neonates will provide the best chances of survival. Although time-consuming, intensive care of these puppies and kittens, which requires serial monitoring, can be extremely rewarding.
Timely treatment of ill neonates will provide the best chances of survival. Although time-consuming, intensive care of these puppies and kittens, which requires serial monitoring, can be extremely rewarding. Because the exact causes of fading puppy and kitten syndrome are often not apparent at the time of presentation, therapy should focus on supportive care and treating the treatable causes while awaiting further diagnostic information. Initial therapy includes providing supplemental warmth, hydration, supplemental glucose, and nutrition, and sometimes blood transfusion and oxygen supplementation.
SUPPLEMENTAL WARMTH
Neonates whose temperatures fall to 94 F (34.4 C) or below suffer ileus and marked bradycardia.1 Without correction, hypothermia results in a fatal spiral of events. Warming should take place gradually, over one to four hours.2 Rapid warming may result in peripheral vasodilation and core collapse.3,4
Good methods for heating include incubators, warmed circulating air or water pads, and covered warm-water bottles. Electric heating pads are not recommended because of uneven heating and a high risk of thermal burns. Only use heat lamps with appropriate technique and supervision. Neonates must be able to move away from the heat. Neonates easily suffer thermal burns because of their thin skin, and the dehydration often present in ill neonates results in poor circulation that increases the risk of burns. In neonates that have or are suspected of having canine herpesvirus infection, body temperatures should be maintained just above 100 F (37.8 C) regardless of age to interfere with viral replication.5
Once the patient is warmed, the ambient temperature should be 85 to 95 F (29.4 to 35 C), with humidity at 55% to 65%.2 Serial monitoring of body temperature is needed to ensure that the hypothermia does not relapse and that the rectal temperature does not rise above what is normal for the neonate's age.
DEXTROSE, FLUID, AND VITAMIN K THERAPY
Hypoglycemia often accompanies hypothermia. Warmed isotonic dextrose solution can be given through a stomach tube, and then 1 to 2 ml 5% to 10% glucose solution can be administered orally or through a tube once the neonate is warmed.2,4 Once venous or intraosseous access is acquired, 20% dextrose solution can be given at a dose of 0.25 ml/25 g in patients that are severely dehydrated, are in shock, or have neurologic signs.4
Venous access is problematic in neonates because of vein size. Jugular catheterization can be performed, but the intraosseous route is most commonly used. Clip and prepare the area over the trochanteric fossa of the femur, and place a 20- to 22-ga spinal needle in a sterile manner. Keep the area covered, and handle it only with sterile gloved hands. Up to 11 ml/min of fluid can be administered by gravity flow with this technique, but unattended gravity flow is contraindicated in neonates.2 Fluid therapy should be provided by pump or slow bolus. If the neonate is in shock, 1 ml/30 g can be given over five to 10 minutes. Maintenance is 60 to 200 ml/kg/day.6,7
Subcutaneous fluid absorption is slow and should be used only for maintenance in stable neonates.6 Fluid injected intraperitoneally can take 24 to 48 hours to absorb, so it is not useful in neonates.8 When choosing a crystalloid fluid, take into account the neonate's immature metabolic processes and avoid lactate-containing fluids. If colloid therapy is needed, hetastarch or dextran 70 can be given at a dose not to exceed 20 ml/kg/day.4 Warm all fluids given to neonates.
In neonates 48 hours of age or younger, vitamin K should be given at a dose of 0.5 to 2.5 mg/kg subcutaneously because thrombin activity is decreased at birth.4
NUTRITION
Once the neonate is warmed and has been given dextrose, if needed, feeding is the next requirement. Hypothermic neonates should not be fed because they cannot digest or absorb their food, and formula sitting in the stomach increases the risk of aspiration pneumonia.
Tube feeding is the ideal route for ill or orphaned neonates. Weak neonates are unable to suckle effectively from an appropriately sized nipple hole. Enlarging the hole to allow easy passage of the formula risks aspiration pneumonia. Tube feeding results in quick, safe administration of appropriate nutrition. Use the largest French red-rubber feeding tube that can be easily passed into the affected neonate's esophagus. Measure from the tip of the neonate's nose to its last rib with the head in an extended position, and mark this length on the tube. This is where the tube must reach to be securely in the stomach.

Table 1. Feeding Protocol for Neonatal Puppies*
The appropriate amount of warmed formula for a neonate's age and species is noted in Table 1 and Table 2.1 These guidelines should be adjusted to attain appropriate daily weight gains. In general, feed 22 to 26 kcal/100 g/day.9 While some advocate feeding intervals greater than every two hours, I have found greatly improved survival rates when feedings are maintained at two-hour intervals.

Table 2. Feeding Protocol for Neonatal Kittens*
If a conspecific foster dam is not available, use formula appropriate for the species. While homemade formula may be useful in an emergency, commercial formula is recommended because it is similar to dam's milk (Table 3).10 If returning to the dam is not possible, cross fostering to an appropriate dam is ideal. Many puppies and kittens fed commercial formula exclusively may develop diarrhea or constipation. Administering a probiotic supplement, containing normal beneficial bacteria, is common in neonates. The goal of probiotic administration is to support and provide normal intestinal flora, but no data exist on efficacy in neonatal puppies and kittens. The manufacturer should provide a product evaluation for content of live organisms. If probiotics are given, daily administration is most likely required.
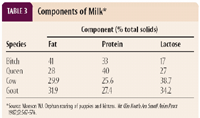
Table 3. Components of Milk*
Tube feed neonates until it is no longer possible to do so. Once neonates are too vigorous for tube feeding, bottle-feeding can commence. Using bottles and nipples for premature infants is often more successful than pet nursing bottles, except for very tiny neonates.
Kittens at risk for neonatal alloimmune hemolytic anemia can be removed from their dam before nursing and allowed to suckle a lactating type A queen. Queens produce antibodies in their milk throughout lactation, so passive antibody transfer will occur. Kittens can continue to be fostered on the type A queen or returned to their dam after 24 to 48 hours.11 For kittens and puppies that do not receive colostrum, passive antibodies can be provided by using serum from healthy, well-vaccinated donors.11,12 In pups, 16 ml pooled serum can be given subcutaneously, either slowly or in multiple doses over 24 hours.12 To collect serum, obtain blood in a sterile manner from healthy, well-vaccinated donors free of communicable diseases. Once the blood has clotted and been centrifuged, remove the serum and administer it in a sterile manner. In kittens, appropriately typed serum given subcutaneously at a dosage of 150 ml/kg divided into three doses and given over a 24-hour period provides passive antibody concentrations until at least 6 weeks of age that are similar to antibody concentrations of kittens that receive colostrum.11
Lay sources often advocate administering bovine or caprine colostrum to neonatal kittens and puppies. While this colostrum will not provide any passive antibody protection, it may supply important nutritional components to the enterocytes.13 Further evaluation of such therapy is needed, but it likely does no harm.
At 3 weeks of age in puppies and 4 weeks of age in kittens, offer puppy or kitten food mush four times a day. Most healthy neonates will start to eat within a few days of this age. Mush is made by combining growth formula canned or dry with warm water to make gruel. Some kittens will refuse gruel yet readily eat dry food from an early age.
TRANSFUSION
Type A kittens that nurse from a type B dam are at great risk of death. They may be saved by a transfusion of washed type B red blood cells or by a transfusion from the dam or a cat successfully cross-matched with the dam.2,4 Three days after birth, additional transfusions can be given that consist of washed type A blood, as the kitten will be forming its own antibodies by that time.2 Wash red blood cells three times in 0.9% saline solution to remove all traces of plasma. Avoiding the problem is the best solution by selecting a compatible sire and dam or by removing kittens at birth and before any nursing for the first 24 hours.
Puppies and kittens with hookworm infestation may also require transfusion. Donors should be cross-matched, and a 10 to 20 ml/kg transfusion can be administered intraosseously over a four-hour period.4
OXYGEN SUPPLEMENTATION
Kittens and puppies with pneumonia, either infectious or aspiration, may require oxygen therapy. Indications include cyanosis, tachypnea, dyspnea, and abnormal lung sounds on auscultation.6 The fraction of inspired oxygen should not exceed 40% to 60% to avoid oxygen toxicity, which can cause retinal damage or acute respiratory distress syndrome.14 While oxygen cages, either commercial or home-built, are readily available, the frequency with which ill neonates need to be assessed makes it difficult to sustain useful oxygen concentrations.
Intranasal oxygen is an excellent way to oxygenate ill neonates, and the technique is well-described.15,16 I use a small French feeding tube with multiple holes placed.15 The largest tube size possible should be premeasured to the medial canthus.15 Topical proparacaine may be used on the nasal mucosa.15 Tilt the neonate's head with its muzzle upward, and then insert the tube, directing it ventromedially to the premeasured distance. Attach the tube with suture or tissue adhesive close to the nostril, on the muzzle, and on the forehead. Then attach the tube through an adapter to a humidified oxygen source.15 An Elizabethan collar is recommended in all but the most lethargic of patients. For patients less than 22 lb (10 kg), administering humidified oxygen at a flow rate of 40 ml/min/kg will result in a tracheal oxygen concentration of 40%.16
GENERAL OBSERVATIONS ABOUT DRUG ADMINISTRATION
Particular physiologic differences affect drug use in neonatal patients. Drug absorption can be reduced when drugs are given intramuscularly because of decreased vascular supply and small muscle mass.17 Absorption from subcutaneous injections can also be quite variable in neonates—drugs can either be more rapidly absorbed or less so.18,19 A neonate's temperature can also affect the subcutaneous absorption rate.6,19 Oral absorption can be more rapid because of increased intestinal permeability for the first few weeks of life; however, decreased oral absorption of some drugs is also seen.20 Hypothermic puppies often have delayed intestinal absorption. Intraosseous drug administration is often used, and absorption is rapid by this route.19
The volume of distribution of drugs is also altered in neonates because of a higher percentage of body water compared with adults. Plasma protein is lower in neonates, and this affects drug distribution. In addition, neonatal albumin has a lower affinity to bind many drugs, often resulting in a higher free drug concentration in serum.19 Also, the blood-brain barrier is more permeable for the first several weeks of life.19
Finally, drug metabolism is altered in neonates because of reduced glomerular filtration rate and tubular secretion in the kidneys.19 Hepatic metabolism is also immature.19
These alterations in drug absorption, distribution, and metabolism in neonates provide us with challenges in administering drugs. Few studies give us absolute answers, so we must make our best choices based on understanding the pharmacology of the particular drug.
Antimicrobial and antiviral treatment
Since most ill neonates will not have a definitive diagnosis at the onset of treatment, antibiotics are often administered in case bacterial infection is present. Common antibiotics used in neonates are shown in Table 4. In general, beta-lactam antibiotics are considered safe and are typically used as initial empirical therapy. While concern exists about the use of fluoroquinolones in immature patients because of the risk of cartilage damage, they have been used successfully in neonates under the age of 4 weeks with no apparent ill effects.4,19 In resistant infections, the benefits of use may outweigh the risk. One study showed that in kittens 2 to 8 weeks of age, subcutaneous and intravenous administration of enrofloxacin achieved therapeutic ranges when given at 5 mg/kg, but oral dosing did not.20

Table 4. Antibiotic Use in Neonates*
In puppies with canine herpesvirus infection, treatment with acyclovir (10 mg/kg orally every six hours for five days) can be successful.5
Antiparasitic treatment
Empirically treat all neonates with pyrantel pamoate for prepatent roundworm and hookworm infestations. While treatment is routinely started at 2 weeks of age and continued every two weeks until post-weaning, it can be safely given to ill neonates at any age at a dosage of 5 to 10 mg/kg orally.7 Preventing larval migration from the dam to offspring can be achieved with fenbendazole at a dosage of 50 mg/kg given orally daily from Day 40 of gestation to 14 days postpartum.7
Giardiasis in the neonate can be treated with fenbendazole as well at the same dosage for seven days. Coccidiosis can be treated with sulfadimethoxine at 30 mg/kg/day for 20 days in puppies and kittens weighing at least 2.2 lb (1 kg).7 Tritrichomonas foetus infection causes chronic large bowel diarrhea in kittens. It has been successfully treated in 10-week-old kittens with ronidazole (30 to 50 mg/kg b.i.d. for two weeks).21
THERAPY FOR CONGENITAL DEFECTS AND THYMIC DYSFUNCTION
Certain defects, such as cleft palates and patent ductus arteriosis, are amenable to surgical correction. With cleft palates, the neonate must be carefully tube fed until surgery can be successfully completed, typically 6 to 12 weeks of age depending on breed and size. Patent ductus arteriosis is best corrected as soon as the pup is large enough for the surgeon to operate—this may be 6 to 9 weeks of age. Atresia ani, while technically correctable with surgery, carries a high risk of permanent fecal incontinence, so most neonates with this problem are euthanized.
In swimmer neonates, the typical dorsoventral flattening and inability to walk are responsive to physical therapy. Rule out pectus excavatum because of its poor prognosis. Once you identify dorsoventral flattening in a puppy or kitten, change the neonate's bedding to egg-crate foam or heavy artificial sheepskin to provide good footing. Loose tape hobbling of the affected limbs will reduce the permanent dorsoventral flattening.22 Be sure not to compromise blood flow to the limbs when applying hobbles, and check them frequently as the neonate grows. In addition, make a channel from towel-covered concrete blocks just wide enough for the neonate to walk through. Three times a day, pass the neonate through this channel five to 10 times. This protocol is almost always successful in achieving normal locomotion, although the thorax may always be somewhat flattened.
One form of wasting syndrome in pups due to thymic atrophy was responsive, in limited clinical trials, to subcutaneous injections of 0.1 mg/kg of pituitary-derived bovine growth hormone daily for five doses, then on alternate days for five doses, then every three days for four additional doses.23
CONCLUSION
Treating fading puppy and kitten syndrome focuses on correcting hypothermia, hypoglycemia, dehydration, and inadequate nutrition, as well as treating any treatable disease that may be present. Frequent serial monitoring and subsequent adjustment of therapy will provide successful outcomes in a high percentage of cases.
Joni L. Freshman, DVM, MS, DACVIM
Canine Consultations
3060 Woodview Court
Colorado Springs, CO 80918
REFERENCES
1. Johnston SD, Root Kustritz MV, Olson PNS. The neonate—from birth to weaning. In: Canine and feline theriogenology. Philadelphia, Pa: WB Saunders Co, 2001;146-167.
2. Bucheler J. Fading kitten syndrome and neonatal isoerythrolysis. Vet Clin North Am Small Anim Pract 1999;29:853-870.
3. Hoskins JD. Clinical evaluation of the kitten from birth to eight weeks of age. Compend Contin Educ Pract Vet 1990;12:1215-1225.
4. Macintire DK. Pediatric intensive care. Vet Clin North Am Small Anim Pract 1999;29:971-988.
5. Davidson AP, Grundy SA, Foley JE. Successful medical management of neonatal canine herpesvirus: a case report. Commun Therio 2003;3:1-5.
6. Lee JL. Critical care of the neonate, in Proceedings. Soc Therio Annu Meet 2004;326-333.
7. Root Kustritz MV. Common disorders of the small animal neonate, in Proceedings. Soc Therio Annu Meet 2004;316-325.
8. Moon PF, Massat BJ, Pascoe PJ. Neonatal critical care. Vet Clin North Am Small Anim Pract 2001;31:343-365.
9. Lawler DF, Chandler ML. Indications and techniques for tube feeding puppies. Canine Pract 1992;17:20-23.
10. Monson WJ. Orphan rearing of puppies and kittens. Vet Clin North Am Small Anim Pract 1987;17:567-576.
11. Levy JK, Crawford PC, Collante WR, et al. Use of adult cat serum to correct failure of passive transfer in kittens. J Am Vet Med Assoc 2001;219:1401-1405.
12. Bouchard G, Plata-Madrid H, Youngquist RS, et al. Absorption of an alternate source of immunoglobulin in pups. Am J Vet Res 1992;53:230-233.
13. Wolinski J, Biernat M, Guilloteau P, et al. Exogenous leptin controls the development of the small intestine in neonatal piglets. J Endocrinol 2003;177:215-222.
14. Jenkins JS. Oxygen toxicity. J Crit Care Med 1988;3:137-152.
15. Marks SL. Cardiopulmonary resuscitation and oxygen therapy. Vet Clin North Am Small Anim Pract 1999;29:959-969.
16. Fitzpatrick RK, Crowe DT. Nasal oxygen administration in dogs and cats: experimental and clinical investigations. J Am Anim Hosp Assoc 1986;22:293-300.
17. Jones RL. Special considerations for appropriate antimicrobial therapy in neonates. Vet Clin North Am Small Anim Pract 1987;17:577-602.
18. Hoskins JD. Pediatric health care and management. Vet Clin North Am Small Anim Pract 1999;29:837-852.
19. Plumb DC. Drugs in neonates: principles and guesses, in Proceedings. Soc Therio Annu Meet 2004;307-315.
20. Seguin MA, Papich MG, Sigle KJ, et al. Pharmacokinetics of enrofloxacin in neonatal kittens. Am J Vet Res 2004;65:350-356.
21. Gookin J, Copple C, Papich M. Efficacy of ronidazole in vitro and in vivo for treatment of feline Tritrichomonas foetus infection (abst). J Vet Intern Med 2005;19:436.
22. Shires PK, Schulz KS. The skeletal system. In: Hoskins JD, ed. Veterinary pediatrics: dogs and cats from birth to six months. Philadelphia, Pa: WB Saunders Co, 2001;402-423.
23. Roth JA. Possible association of thymus dysfunction with fading syndromes in puppies and kittens. Vet Clin North Am Small Anim Pract 1987;17:603-616.
Episode 67: Choosing trusted supplements
October 20th 2021In this episode of The Vet Blast Podcast, Dr Adam Christman chats with Dr Janice Huntingford about the latest insights into selecting the best supplements for your patients, including the importance of recommending and utilizing products that have a substantial amount of science and research behind them. (Sponsored by Vetoquinol)
Listen