Lecture Link: New trends in handling histoplasmosis
An antigen assay is one of the newer tools at your disposal for diagnosing this fungal disease.
An antigen assay is one of the newer tools at our disposal for diagnosing histoplasmosis. In her presentation "Histoplasmosis: Current diagnostic and treatment strategies," Audrey Cook, BVM&S, MRCVS, DACVIM, DECVIM–CA, discussed the methodology behind the test and how it may be used to diagnose and manage histoplasmosis cases.1
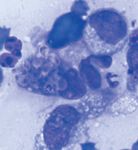
ZEROING IN ON A DIAGNOSIS
Histoplasma species organisms release antigens into affected tissues, and those antigens can then enter the plasma, urine, and cerebrospinal fluid. New assays can detect these antigens with good sensitivity and specificity, making cytologic or histopathologic identification of the organism less necessary.
While there is little in the veterinary literature regarding the use of this test, Dr. Cook discussed a study currently in press that found a sensitivity of 94% when compared with the gold standard of cytologic or histopathologic identification of the organism. Dr. Cook noted, however, the clinician "cannot exclude histoplasmosis infection on the basis of one negative result." She also said the test is less sensitive for patients with intestinal involvement.
Because the antigen passes through the glomerulus, it is concentrated in the urine, so urine may be the most sensitive sample to submit for testing. Dr. Cook also said serologic testing for histoplasmosis is of little use since false negative and false positive results are common.
WHICH TREATMENT TO TRY
- Itraconazole: The mainstays of histoplasmosis treatment are the azole drugs, of which itraconazole has shown the best efficacy. A dosage of 5 mg/kg given twice a day or 10 mg/kg given once a day is the standard therapy, with steady state being achieved within two weeks. The capsule form of this drug is best absorbed if given with a fatty meal, while the liquid formulation is best absorbed if administered before eating. The capsules should not be administered concurrently with antacids. The most significant side effect of itraconazole is dose-dependent hepatotoxicosis, which generally occurs within the first two months of therapy.
Dr. Cook noted no real difference between the brand name itraconazole and the generic. Reported problems of efficacy have primarily been with compounded formulations in which there have been issues with accuracy and consistency among products. If using these products, it is best to perform therapeutic drug monitoring.
- Fluconazole: This azole drug can also be used to treat histoplasmosis and is best for patients with central nervous system or ocular involvement because of its ability to cross the blood-brain barrier. Direct comparison studies between itraconazole and fluconazole for efficacy against histoplasmosis have not been performed.
- Voriconazole: A relatively new azole in veterinary medicine, voriconazole has been shown to have good bioavailability. Dr. Cook cautioned that neurologic side effects are noted with this drug but that these signs abate once treatment is discontinued. She also said the use of voriconazole in veterinary patients with histoplasmosis is not recommended at this time unless standard treatment is unsuccessful and resistance is suspected.
- Posaconazole: This broad-spectrum azole has also shown to be an effective treatment for aspergillosis and candidiasis. As with voriconazole, posaconazole is not recommended unless standard treatment is unsuccessful and resistance is suspected.
- Amphotericin B: Unlike the azoles, amphotericin B also affects mammalian cells and has potential adverse effects, such as nephrotoxicity. The liposomal formulation is targeted to only fungal cells; however, the cost of this drug is a concern.
- Terbinafine: Terbinafine is a squalene epoxidase inhibitor and may work synergistically with the azoles. But no dosages have been established for histoplasmosis treatment.
TREATMENT MONITORING
To assess response to therapy, Dr. Cook recommended monitoring for return of clinical signs, serial radiographic changes, and serial antigen concentrations. Treatment for these patients generally lasts for more than six months, with azoles being continued for at least one month past resolution of clinical signs. Antigen concentrations would be expected to decline within four to eight weeks of initiating therapy.
REFERENCE
1. Cook A. Histoplasmosis: current diagnostic and treatment strategies. Presented at the Annual Meeting of the American College of Veterinary Internal Medicine; June 2012.
This "Lecture Link" summary from the 2012 American College of Veterinary Internal Medicine Forum was contributed by Jennifer L. Garcia, DVM, DACVIM, a veterinary internal medicine specialist at Sugarland Veterinary Specialists in Houston, Texas.

Dr. Jennifer L. Garcia