Multiple myeloma in a 9-year-old Labrador: Clinical pathology perspective
Dr. Lisa Viesselmann provides the clinical pathology perspective on this multiple myeloma case.

Lisa Viesselmann, DVMSerum protein electrophoresis (SPE) is an important tool in the work-up of multiple myeloma, as it is necessary for the identification of a monoclonal gammopathy-one of the four main diagnostic criteria for the cancer. SPE separates serum proteins on the basis of their size, shape and electrical charge, and in dogs is often used to investigate the cause of an increased total globulin concentration.1 The height and width of the peaks on a densitometer tracing of the SPE gel (agarose gels are most commonly used) are directly related to the number of proteins in each region and to the quantity of these proteins. Six distinct regions are typically visible on SPE tracings in dogs: α1, α2, β1, β2 and γ globulins, and albumin.1 A serum protein electrophoretogram from a normal dog is shown in Figure 1. Because albumin is the only protein that migrates in this region, the albumin peak has a narrow base. It is also taller than the other regions because in health, it is the most abundant protein in serum.
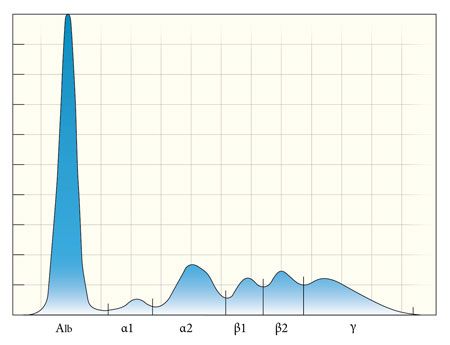
Figure 1. A serum protein electrophoretogram from a normal dog highlights the distinct protein regions typically present in canine serum. The albumin peak is the tallest, with a narrow base. The globulin peaks are shorter with wider bases, reflecting the multiple protein types migrating in these regions. A dog with a monoclonal gammopathy will have a narrow-based peak in either the β2 or γ region that is at least as tall as the albumin peak (Figure 2). The monoclonal peak is so named because it is composed of a large quantity of immunoglobulin proteins being produced by a single clone of neoplastic plasma cells.1 Multiple myeloma is the most common cause of a monoclonal gammopathy, and the source of the increased immunoglobulin (known as a paraprotein-typically IgA or IgG) is a single clone of neoplastic plasma cells. B-cell lymphoma, leukemia and extramedullary plasmacytomas can also produce a monoclonal gammopathy.2 The addition of anti-immunoglobulin antibodies to the analysis (immunoelectrophoresis) can aid in identifying the immunoglobulin class and heavy chain isotype (IgA, IgG, IgM) as well as the light chain class (kappa or lambda).
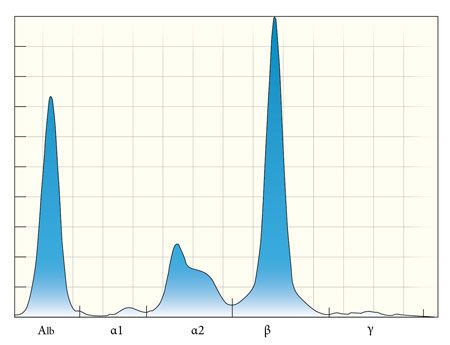
Figure 2. A serum protein electrophoretogram from a dog (not the patient in this case) shows the key diagnostic features of a monoclonal gammopathy: a narrow-based peak that is at least as tall as the albumin peak. A monoclonal gammopathy is the result of a single clone of neoplastic lymphoid cells producing a single type of immunoglobulin.Chronic infectious and inflammatory diseases can also cause increases in immunoglobulin concentrations, although we expect these conditions to produce a polyclonal gammopathy, which is differentiated from monoclonal gammopathy by a wide-based peak in the β2 to γ region (Figure 3). The shorter, wider base indicates that the peak is composed of multiple immunoglobulin types being produced by different populations of inflammatory lymphoid cells.
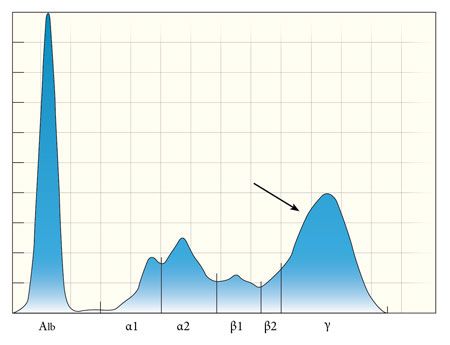
Figure 3. In contrast to a monoclonal gammopathy, a polyclonal gammopathy is the result of multiple lymphoid populations producing different isotypes of immunoglobulins, typically as part of a chronic inflammatory process. The globulin peaks (arrow) are taller than normal, but are shorter and wider than the albumin peak. Depending on the degree of ongoing active inflammation, a polyclonal gammopathy may be accompanied by smaller peaks in the alpha and beta regions (consistent with an acute phase response).1 In the patient in this case, the electrophoretogram revealed a polyclonal gammopathy with a small monoclonal component-a pattern sometimes referred to as a restricted oligoclonal gammopathy (Figure 4). This pattern suggests the possibility of a lymphoid neoplasm with concurrent antigenic stimulation of another source, although it is nonspecific and is not diagnostic for multiple myeloma in itself.3
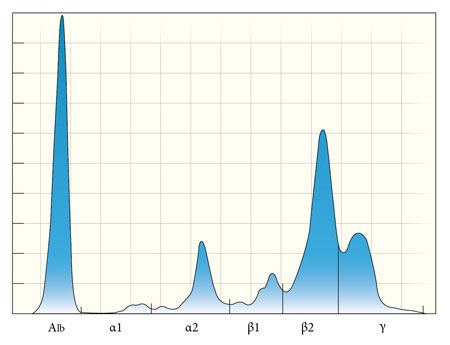
Figure 4. The serum electrophoretogram from the patient in this case demonstrates a unique pattern sometimes referred to as a restricted oligoclonal gammopathy, with a monoclonal peak superimposed on a polyclonal peak. This pattern is nonspecific and may be seen with chronic inflammatory diseases as well as with lymphoid neoplasia. Additional diagnostics are required to definitively diagnose or rule out multiple myeloma. Another, less common, SPE pattern that can be observed in cases of multiple myeloma is a biclonal gammopathy, in which two separate clones of neoplastic cells, a single clone producing two separate immunoglobulin isotypes, or the dimeric or multimeric forms of a single immunoglobulin (i.e. IgA, IgM) migrate separately through the gel (Figure 5).4
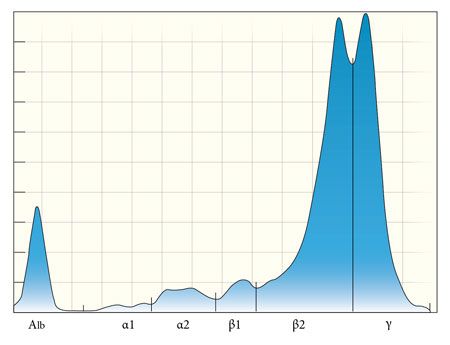
Figure 5. Biclonal gammopathy is another unique SPE pattern that may be seen in patients with multiple myeloma, and immunoelectrophoresis may aid in identifying two separate immunoglobulin populations or a single dimeric or multimeric immunoglobulin.While a polyclonal gammopathy is the expected SPE pattern for cases of chronic infection and inflammation, certain conditions can produce an apparent monoclonal gammopathy on agarose gel electrophoresis. In dogs, Ehrlichia canis and visceral leishmaniasis infections, chronic pyoderma and several immune-mediated disorders have been reported in association with a monoclonal gammopathy.5 In many of these cases, immunoelectrophoresis can be used to reveal the presence of more than one immunoglobulin subclass or more than one type of light chain. However, true monoclonal gammopathies have been reported with these non-neoplastic disorders, and they are important differentials in the absence of other diagnostic criteria for multiple myeloma.5
Protein electrophoresis can also be used to detect Bence Jones proteinuria, which is present in 25% to 40% of dogs with multiple myeloma.2 Bence Jones proteins are the free immunoglobulin light chain components of the paraproteins. Since these light chains are relatively small, they can pass freely through the glomerular filtration barrier. In health, any light chains that pass through the glomerular basement membrane are resorbed in the proximal tubules. However, with the magnitude of paraproteinemia that can be present in multiple myeloma, the resorptive capacity of the proximal tubules is exceeded and the proteins enter the urine.6
Urine protein electrophoresis is the recommended method for detecting Bence Jones proteins, and a pattern similar to that of the serum is expected in positive cases (monoclonal peak in the β or γ regions).2 Immunoelectrophoresis of the urine is the most sensitive and specific test, but the availability of veterinary-specific anti-light chain antibodies is often a limiting factor. Standard urine dipstick analysis, sulfosalicylic acid testing and heat precipitation methods for detecting Bence Jones proteins have all been described, but these tests are prone to false positive results due to nonspecific detection of polyclonal immunoglobulin proteins that may be present for a variety of reasons, including inflammation and chronic renal disease.2
Bone marrow plasmacytosis is a third diagnostic criterion for multiple myeloma. Plasmacytosis is defined as a condition in which plasma cells compose at least 5% of the total nucleated cell population in canine bone marrow aspirates (normal is defined as less than 2%).2 However, the proportions vary in individual cases.
Neoplastic plasma cells may appear well-differentiated, with pale to moderately basophilic cytoplasm, a small, eccentric nucleus, and a clear perinuclear region representing the Golgi apparatus (Figure 6). More immature and atypical plasma cells may also be seen, along with more deeply basophilic cytoplasm and a higher nuclear to cytoplasmic ratio.7
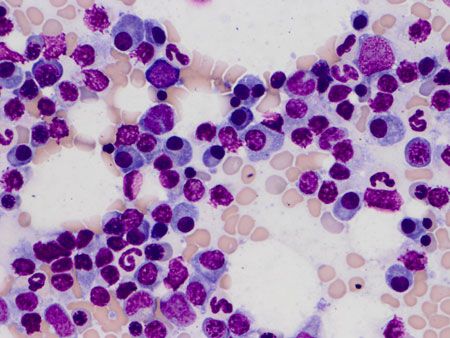
Figure 6. The bone marrow aspirate from the patient in this case contains many individual, well-differentiated plasma cells. In this field, mildly increased numbers of plasma cells are present, scattered among various stages of normal erythroid and myeloid precursor cells. An occasional binucleate plasma cell is seen (500x magnification, methanolic Wright's stain). Binucleation and occasional trinucleation may be seen in well-differentiated plasma cells, and features of plasmacytoid differentiation (Mott cells, flame cells) may also be present.8 The distribution of plasma cells in the bone marrow is often uneven, with some fields of an aspirate appearing to contain normal proportions of plasma cells scattered among other hematopoietic precursors, while other fields contain homogenous sheets and aggregates of plasma cells to the exclusion of other cell lineages (Figure 7). For this reason, many cytologists will perform a 500-cell differential across multiple areas of the slide to ensure an accurate representation of the sample. Overall marrow cellularity may be normal, increased or decreased, and the main hematopoietic lineages (erythroid, myeloid and megakaryocyte) may or may not be affected.
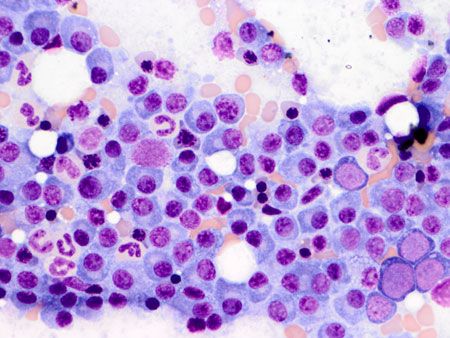
Figure 7. Other fields in this patient's bone marrow aspirate contain large sheets of plasma cells with relatively few normal hematopoietic cells present. This highlights the fact that the neoplastic cells often have an uneven distribution in the bone marrow, and emphasizes the importance of examining several fields (500x magnification, methanolic Wright's stain).It is important to note that chronic inflammatory conditions (such as those that might cause an apparent monoclonal gammopathy) may also cause bone marrow plasmacytosis. Interpretation of bone marrow plasmacytosis should therefore be done in conjunction with the other diagnostic criteria for multiple myeloma. Diagnostic aspirates from lytic bone lesions of affected dogs appear similar to bone marrow aspirates, often predominantly consisting of sheets of normal to atypical immature plasma cells.
References
Thrall MA, Weiser G, Allison R, et al. Laboratory evaluation of plasma and serum proteins. In: Veterinary hematology and clinical chemistry. 2nd ed. Oxford, UK: Wiley-Blackwell, 2012.
Weiss DJ, Wardrop KJ. Plasma cell tumors. In: Schalm's veterinary hematology. 6th ed. Hoboken, New Jersey: Wiley-Blackwell, 2010.
Geigy C, Riond B, Bley CR, et al. Multiple myeloma in a dog with multiple concurrent infectious diseases and persistent polyclonal gammopathy. Vet Clin Pathol 2013;42(1):47-54.
Facchini RV, Bertazzolo W, Zuliani D, et al. Detection of biclonal gammopathy by capillary zone electrophoresis in a cat and a dog with plasma cell neoplasia. Vet Clin Pathol 2010;39(4):440-446.
Antognoni MT, Birettoni F, Miglio A, et al. Monoclonal gammopathy associated with multiple myeloma and visceral leishmaniasis in the dog: a comparison of two cases. Vet Res Commun 2010;34 Suppl 1:S97-S101.
Burtis CA, Ashwood ER, Bruns DE. Kidney disease. In: Tietz textbook of clinical chemistry and molecular diagnostics. 4th ed. St. Louis: Elsevier, 2006.
Valenciano AC, Cowell RL. The bone marrow. In: Cowell and Tyler's diagnostic cytology and hematology of the dog and cat. 4th ed. St. Louis: Elsevier, 2013.
Harvey JW. Disorders of bone marrow. In: Veterinary hematology: a diagnostic guide and color atlas. St. Louis: Elsevier, 2012.