The physiologic effects of fear
An overview of the signs and effects of fear, anxiety, stress and phobias in pets.
For far too long, veterinarians and many pet owners have accepted the fact that a certain amount of fear displayed by pets in the veterinary clinic is "normal." While veterinarians have always sought to minimize injury to staff and clients, we have often just accepted the occasional bite or scratch as part of the job. We simply buy muzzles and make sure we have a wide variety of sedative options on hand. By doing this, we have neglected the potentially serious mental damage that we may have been inflicting upon our patients.
On the other hand, over the past 10 years or so, zoo veterinarians have progressively moved to less physical or chemical restraint and more training, helping their patients to participate in their own medical care. If a 400-lb lion can be taught to present its tail for venipuncture or a 500-lb bottle nose dolphin to present its abdomen for an ultrasonographic examination, why are we so slow to imagine that dogs and cats might also be taught to-at the very least-tolerate physical examination and venipuncture with minimal restraint and distress?

Panting is one sign that a dog is fearful. This dog is also displaying the avoidance of eye contact, lowered ears and head, and the whites of its eyes that are classic signs of a worried dog.
Patients that are frightened from the moment they enter the veterinary clinic are not only unlikely to clearly display the same behavioral signs of illness that they have been displaying at home, but also any samples collected are likely to be altered by their stress response. Again, these are things we have come to accept, but maybe it is time we changed our thinking.
In addition-and what should be of most concern-the animal is having a traumatic experience with strangers that has the potential to profoundly affect its long-term mental health and, ultimately, even its physical health. Lastly, if we accept that all fearful pets entering our doors are "normal," how will we possibly be able to recognize the pathologically fearful or anxious animal?

This dog is exhibiting frequent lip licking-a sign of anxiety or discomfort with the situation the dog is in-in the examination room.
A FEW DEFINITIONS
Fear and anxiety are often spoken in the same breath, but it is helpful to keep in mind that they are not the same thing. They share many similar physiologic responses, but fear should be adaptive when it helps an animal escape from a situation that is truly dangerous. However, both fear and anxiety can lead to great stress when they are chronic or unrelenting or when an animal is unable to change its behavior in such a way as to be better able to cope with the situation or the environment that it finds threatening.
Fear
Fear, by definition, is an emotion that induces an animal to avoid situations and activities that may be dangerous. The emotional response occurs when an animal perceives that something or someone is dangerous. The key word here is perceives. It is critical that veterinarians and pet owners understand that just because they do not think the person, event, or thing is to be feared does not mean that the fear is not real to the pet. A pet's perception is its reality, and that is what the pet will act on.
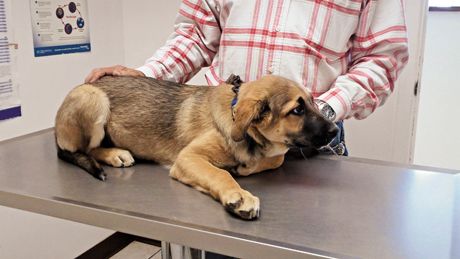
This puppy shows several signs of fear, including lowered ears and head, avoidance of eye contact, a furrowed brow, and visible whites of his eyes. Part of his discomfort is associated with the fact that he can't gain purchase on the slippery exam table-his front legs and toes are splayed in an attempt to grasp the surface and stand.
When pets cannot escape a fearful stimuli, they may freeze or they may fight. This, in many cases, is a perfectly normal adaptive response. Sadly, when pets in the veterinary clinic choose to freeze and tolerate our handling, we continue to restrain and handle them in a way that they find threatening without attending to the fact that they are frightened. Thus, they learn that freezing is not the best strategy, and this increases the chance that they will struggle or fight harder during the next visit.
Veterinarians and veterinary staff should be cognizant of a fearful, compliant animal and attempt to make the visit as pleasant as possible by moving slowly, handling the animal extremely gently with a minimum of restraint, talking quietly, and plying the patient with special food treats before, during, and after the appointment. This type of collaborative effort, where handlers stay attuned to an animal's behavior and change their own behavior appropriately, results in less stressful appointments for everyone. Animals whose appointment ends with a pleasant, positive experience are more likely to leave with that pleasant memory rather than a powerful memory of a fearful experience.
Many pets, for reasons that we are just now beginning to understand, perceive threats where none exist and may truly be suffering from a pathologic degree of fear or anxiety. Without a better understanding of normal animal behavior and an awareness of how our patients are learning from their experiences with us, these patients may be overlooked or their behavior may be misinterpreted, especially in cases in which an animal's history is unknown.
Animals that have been through the shelter system are a good example. When these dogs or cats demonstrate fearful or anxious behavior, it is common for pet owners to simply shrug and say that the pet must have been abused. While this is certainly possible, what must be equally considered is that many fearful and anxious animals are born with these behavioral pathologies. These behaviors, often referred to as shyness or fearfulness by different researchers, have been found to be highly heritable, and the more quickly the problems are recognized and dealt with, the more likely the animal can be helped. Ignoring the problem only extends the animal's suffering-and that should be unacceptable.
Anxiety
Anxiety is the anticipation of future danger that may be unknown, imagined, or real. It can result in physiologic responses similar to those associated with fear. The animal may begin to pace, pant, tremble, and salivate. Pupils dilate and heart rate, blood pressure, and respiratory rate may increase. Anxious or fearful animals may exhibit avoidance behaviors such as hiding and may be hypervigilant-constantly on alert-and possibly even startle at the slightest sudden stimuli. In the case of intense fear, an animal may lose bladder and bowel control and may express its anal sacs.
Animals that live in a constant state of anxiety are not normal nor healthy. Just because their behavior is not a concern for their owners does not mean it should not be a concern to us. As the pet's advocate, we must ask questions about the pet's behavioral responses in a variety of environments so that we can determine if the behaviors we are seeing in the clinic are typical for the pet. If the pet is commonly anxious or fearful about many novel situations, it may need behavioral help.
This is not unlike the many years that we have spent lifting the gums of animals and showing the owners tartar, trying to teach them that just because this did not bother them did not mean it was not a health concern for the pet. Anxiety is no more an esthetic or cosmetic issue than periodontal disease is; anxiety has an effect on virtually every system in the body, not unlike periodontal disease.
Stress
Stress is a concept that comes into play as well. For our purposes, it might be best defined as any chemical, physical, or emotional force that threatens an organism's homeostasis.
While a certain amount of anxiety or fear may be adaptive in some situations, an animal that experiences fear or anxiety frequently, especially if unable to safely escape from fear-inducing stimuli, will begin to suffer from stress and its effects. Since the initial result of fear and anxiety is a physiologic one involving autonomic arousal and stimulation of the hypothalamic-pituitary-adrenal axis (and accompanying release of stress hormones), eventually the animal can suffer physical harm such as an increased susceptibility to disease secondary to suppression of the immune system.
Phobia
Phobia is the final term to consider. Phobias are persistent and excessive fears of certain things or situations that are usually out of proportion to the actual threat that they present. Animals anticipating exposure to these stimuli will often display anxiety. An animal's response to actual exposure to the stimuli can result in a range of responses from relatively mild signs of anxiety to extreme panic and even catatonia. Serious injury may occur when animals exhibit such a severe panic response that they chew or tear through doors or windows in an apparent attempt to escape from the frightening stimuli. It is not uncommon for these phobic responses to become increasingly severe with every repeated exposure to the frightening stimulus.
Sadly, phobias are quite common in dogs, and many dogs exhibit phobic responses to loud noises such as fireworks, thunderstorms, and fire alarms. Some animals are so frightened by their experiences at the veterinary clinic that their responses on subsequent visits could be defined as phobic. It should not be acceptable to have to drag a leashed animal into your reception area and onto a scale.
SIGNS OF FEAR OR ANXIETY
The greatest challenge to recognizing stress-related problems in pets probably arises from the fact that most pet owners are not adept at reading their pets' body language. More overt signs such as avoidance behaviors, flattened ears, a crouched body posture, trembling, or panting may be recognizable to them as signs of distress. But the more subtle signs, such as frequent lip licking, yawning with a very tense face, displacement grooming, or avoidance of eye contact are often overlooked. Clients should be educated about reading their pets' body language and taught that ignoring these signs can result in their pets experiencing unnecessary stress and, thus, a reduced quality of life. (Download a client handout on the signs of anxiety and fear in pets at dvm360.com/FearSigns.)
Veterinarians and veterinary staff should also be aware that a pet showing these subtle signs of fear or anxiety is being stressed by the visit, if they continue to proceed without attempting to ameliorate the stress, they may not change the pet's behavior at that time, but the animal will learn from the experience and will likely behave in a more fractious manner at the next visit. (Download a handout to help your staff understand how dogs communicate their discomfort at dvm360.com/AggressionLadder.) Anything that can be done to relieve the stress of the visit will pay off in future visits being less difficult on both the pet and the staff. In addition, veterinarians need to be aware of how frequent, distressing experiences can negatively impact an animal's overall health and well-being.
Also, by continuing with a procedure when an animal is showing signs of anxiety, we are teaching the animal that its normal means of communication is meaningless. If we do that, what recourse might that animal have but to develop other less tolerable means of communicating its discomfort? Essentially, we can take perfectly normal behavioral signaling and cause it to become exaggerated and ultimately abnormal, again to the detriment of ourselves and especially to our patients.
PHYSIOLOGIC EFFECTS
Any time an animal feels threatened, whether that threat is real or imagined, physiologic changes occur immediately within its body to prepare for fight or flight. These changes occur because the sympathetic nervous system and the hypothalamic-pituitary-adrenal axis release a variety of stress hormones that have profound effects across multiple body systems.
The overall effect of this physiologic response is to increase the immediate availability of energy, increase oxygen intake, decrease blood flow to areas not critical for movement, and inhibit digestion, growth, immune function, reproduction, and pain perception. In addition, memory and sensory function are enhanced. Animal caretakers need to be aware that when an animal is under stress, the memories of any events occurring during that time will be very powerful, and our behavior when handling them may have long-standing consequences for our future ability to handle the animal.
When stressors are unremitting and the stress response continues, virtually every system within the body can be pathologically affected to varying degrees-cardiovascular, metabolic, reproductive, gastrointestinal, immune, and integumentary. The results can include myopathy, fatigue, hypertension, decreased growth rates, gastrointestinal distress, and suppressed immune function, with subsequent impaired disease resistance. Chronic stress can even lead to structural and functional changes in the brain, and, when extreme conditions persist, permanent damage can result.
For example, shelter cats exhibiting higher stress scores have been shown to be at a higher risk of upper respiratory tract infections.1 Feline interstitial cystitis (FIC), a common and difficult-to-treat condition in cats that often leads to house soiling, appears to be associated with an increased sensitivity to environmental stress.2,3 One study found that cats with FIC are more likely to live in multicat households and be in conflict with other cats in the household, further supporting the important role that chronic stress may play in this condition.4
Stress has also been shown to impact normal gastrointestinal tract functioning. Chronic stress has been demonstrated to decrease gastric emptying, increase intestinal contractility, increase gut permeability, reduce water absorption in the gut, disrupt normal electrolyte absorption, and increase the colonic inflammatory response.5
In people, stress has been shown to play an important role in the development and exacerbation of several chronic dermatologic conditions. The skin and the central nervous system share many of the same hormones, neuropeptides, and receptors. Many of these substances are involved in neurogenic inflammation, pruritus, and pain sensation, and stress can alter their release. While more research is needed for us to have a better understanding of these relationships in animals, it is logical to assume that stress has the potential to cause pathophysiologic responses that perpetuate the itch-scratch cycle in animals just as it does in people.
Summary
The effects of fear and anxiety are profound and distressing for the animals that must experience them. We need to recognize fearful animals in our clinics, do more to decrease their fear when possible, and prevent fear in new patients by moving more toward a collaborative form of handling and away from the "manhandling" methods of the past. Pets that demonstrate pathologic levels of fear or anxiety need to be recognized and treated. They do not deserve to suffer simply because their owners (or we) do not recognize their suffering.
Valarie V. Tynes, DVM, DACVB, Premier Veterinary Behavior Consulting, Sweetwater, Texas.
REFERENCES
1. Tanaka A, Wagner DC, Kass PH, et al. Associations among weight loss, stress, and upper respiratory tract infection in shelter cats. J Am Vet Med Assoc 2012;240(5):570-576.
2. Buffington CAT, Pacak K. Increased plasma norepinephrine concentration in cats with interstitial cystitis. J Urol 2001;165(6 Pt 1):2051-2054.
3. Buffington CAT, Teng B, Somogyi GT. Norepinephrine content and adrenoceptor function in the bladder of cats with feline interstitial cystitis. J Urol 2002;167(4):1876-1880.
4. Cameron ME, Casey RA, Bradshaw JWS, et al. A study of environmental and behavioural factors that may be associated with feline idiopathic cystitis. J Small Anim Pract 2004;45(3):144-147.
5. Bhatia V, Tandon RK Stress and the gastrointestinal tract. J Gastroenterol Hepatol 2005;20(3):332-339.