Primary hypoparathyroidism in dogs and cats: Physiology, clinical signs, and initial diagnostic tests
Primary hypoparathyroidism is most commonly caused by the destruction or removal of the parathyroid glands.
Primary hypoparathyroidism is rarely diagnosed in dogs and even less frequently in cats.1-4 It is most commonly caused by the destruction or removal of the parathyroid glands. In dogs, hypoparathyroidism most often results from immune-mediated destruction of the parathyroid glands, but in cats the condition occurs secondary to bilateral thyroidectomy, in which the parathyroid glands were inadvertently removed.1,3,5,6
Animals with primary hypoparathyroidism have decreased production of parathyroid hormone (PTH).3 PTH maintains normal serum calcium and, to some extent, phosphorus concentrations. A lack of PTH results in severe hypocalcemia and mild to moderate hyperphosphatemia through several mechanisms, including decreased bone resorption, decreased renal excretion of phosphate, decreased serum calcitriol (1,25-dihydroxycholecalciferol, or vitamin D3), decreased intestinal absorption of calcium, and increased renal excretion of calcium.1
The neurologic and neuromuscular clinical signs of hypocalcemia do not vary with its cause and are merely supportive in diagnosing hypoparathyroidism.1 While hypocalcemia is not an uncommon laboratory abnormality, hypoparathyroidism is an uncommon cause, so other causes of hypocalcemia must be considered.1,5
SERUM CALCIUM REGULATION
About 99% of the body's total calcium is within the skeleton, about 1% is intracellular, and 0.1% is in the extracellular fluid (i.e. in the plasma).7 In plasma, calcium exists in three forms: about 50% to 60% is ionized (the physiologically active form), about 35% is protein-bound (particularly albumin), and about 10% is complexed (i.e. bound to phosphate, bicarbonate, sulfate, citrate, or lactate).1,7,8 The control of the total serum calcium concentration is so precise that in a healthy animal, the setpoint ranges between 10.5 and 11.5 mg/dl, and the ionized calcium varies less than 0.1 mmol/L in either direction from its setpoint.1,2 The serum calcium concentration is controlled by the interaction among PTH, calcitriol, and calcitonin and their influence on calcium absorption from the intestine, calcium excretion by the kidneys, and uptake and release of calcium from the bone.7,8 PTH is the most important factor in serum calcium regulation.2,9
Because calcium plays an important role in stabilizing the permeability of cell membranes to sodium, hypocalcemia can cause progressive excitation of the nervous system.4,10 Calcium is also essential for normal contraction of skeletal, cardiac, and smooth muscle.7,11 Additionally, precise control of the serum ionized calcium concentration is critical because of calcium's role as an intracellular second messenger, in regulating mitochondrial metabolism, and as a cofactor in the coagulation cascade.4,11
Parathyroid hormone
The only biologically active product of the parathyroid glands is PTH, which is produced by specialized cells called chief cells.1,7 The other cell type in the gland, the oxyphil cell, is rare in carnivores and produces no known active substance.7,12 A pair of parathyroid glands are in close association with each thyroid gland.1,2 In cats, half of each parathyroid pair is embedded within the capsule of the thyroid gland or within the thyroid gland itself.12
PTH is first formed as a preprohormone on the ribosomes of the chief cells.7,9 Within the endoplasmic reticulum and Golgi apparatus, the molecule is cleaved sequentially to the prohormone and then to PTH.7,9 PTH is subsequently packaged into secretory granules within the cytoplasm.7 Within the chief cells of the parathyroid gland, a calcium-sensing receptor enables the chief cells to act as sensors of the extracellular calcium concentration.9 The serum ionized calcium provides proportional feedback, inhibiting or stimulating the release of PTH.1,2,7,9,12 Although less physiologically important, calcitriol also inhibits the production and release of PTH.9
PTH mobilizes both calcium and phosphorus from bone, causes the kidneys to retain calcium and excrete phosphate, and indirectly increases intestinal absorption of calcium and phosphate (Figure 1).1,2,9 PTH has both rapid and long-term effects on bone.7 In acute hypocalcemic situations, the rate of bone breakdown and subsequent calcium release into the blood is increased, and changes in serum calcium can be noted within minutes.7,9 Initially, calcium salts (about 1% of total body calcium), particularly CaHPO4, serve as a readily exchangeable reservoir of calcium.7,8 If hypocalcemia and elevation in PTH continue for several days to weeks, PTH causes proliferation of osteoclast-mediated breakdown of existing bone (osteolysis). Osteoclasts, unlike osteoblasts and osteocytes, lack receptors for PTH, so osteoclast activation is likely indirect through cytokines (e.g. insulin-like growth factor 1, interleukin 6, granulocyte-macrophage stimulating factor) released by activated osteoblasts and osteocytes.7,9 Osteolysis results in increased serum phosphorus and calcium concentrations.
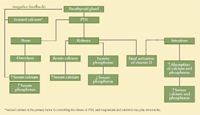
Figure 1. Regulation of parathyroid hormone (PTH). This illustration shows the direct (solid lines) and indirect (dashed line) effects of PTH on bone, kidneys, and intestines. PTH's net effect is to increase serum calcium and decrease serum phosphorus concentrations.
In normal animals, ionized and complexed calcium (but not protein-bound calcium) passes into the glomerular filtrate.7 Ninety-nine percent of this calcium is eventually reabsorbed.7,13 About 90% of the reabsorption of calcium occurs in the proximal tubules, loop of Henle, and early distal tubules.7 In the thick ascending limb of the loop of Henle, there is marked reabsorption of calcium because of the positive charge within the lumen of the tubules compared with the surrounding interstitial fluid.7 The reabsorption of the final 9% or 10% of calcium depends on the serum ionized calcium concentration and presence of PTH, which if present increase the degree of calcium reabsorption in the late distal tubules and early collecting ducts.1,7,9,13 In the proximal tubule, phosphate reabsorption is inhibited by PTH.7,9,13 PTH in the proximal tubule also stimulates the enzyme 1-alpha-hydroxylase, vital in the final conversion of the vitamin D precursor to its most active form, calcitriol (discussed later).9,11 The net effects of PTH on the kidneys are to decrease the serum phosphorus concentration and increase the serum calcium concentration.
Calcitonin
Calcitonin's activity further controls the effects of PTH on calcium. Calcitonin, the hormone produced by the parafollicular cells (also called C cells) of the thyroid gland, antagonizes the actions of PTH, particularly on bone.7 The effects of calcitonin are relatively weak compared with PTH.7
Vitamin D metabolism, including calcitriol
Long-term maintenance of the serum calcium concentration is controlled primarily by calcitriol and its ability to increase intestinal calcium absorption.9 Vitamin D's regulatory role is especially important in managing primary hypoparathyroidism. Multiple forms of vitamin D exist, including vitamin D1 (calciferol), vitamin D2 (ergocalciferol), and vitamin D3 (any of the analogues containing the word cholecalciferol).14 The major source of cholecalciferol in animals is the diet, primarily tissues from animals and fish liver oil; smaller amounts are produced in the skin.4 In the skin, 7-dehydrocholesterol is converted into cholecalciferol with exposure to ultraviolet light (UVB, wavelength 290 to 320 nm); this conversion is more important in people, since other mammals contain only small amounts of 7-dehydrocholesterol in their skin.7,11
Production of a biologically active vitamin D analogue requires multiple steps (Figure 2). Cholecalciferol undergoes several modifications, with the final product, calcitriol, being substantially more potent than its precursors.7 The first conversion occurs within the liver, where cholecalciferol is hydroxylated by a complex interaction of enzymes and cofactors into 25-hydroxycholecalciferol4,11,14 ; this conversion is regulated by negative feedback of 25-hydroxycholecalciferol.7 Unconverted cholecalciferol may be stored in the liver for months.7 In the proximal tubules of the kidneys, 25-hydroxycholecalciferol is converted into the most active form, calcitriol, by the enzyme 1-alpha-hydroxylase, under PTH regulation.4,7,11,13 The presence of sufficient amounts of calcium (directly and indirectly by PTH) or phosphorus (directly) in the plasma inhibits this conversion in the kidneys.5,7 In the absence of PTH, the 25-hydroxycholecalciferol is converted instead to 24,25-dihydroxycholecalciferol, which is biologically inactive.4,7
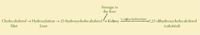
Figure 2. Steps in the conversion of vitamin D to its most active form, calcitriol.
Calcitriol's primary function is to increase intestinal absorption of calcium and phosphorus.7 In people, about one-third of the dietary calcium is absorbed and the remainder is passed in the feces.7 Calcitriol increases the production of a calcium-binding protein within intestinal epithelial cells.4,7 The rate of intestinal calcium absorption is directly related to the amount of calcium-binding protein present within the enterocytes.7 Calcium-binding protein acts to transport calcium across the brush border into the enterocyte.4,7 Through calcium-binding protein's effect, calcitriol can cause an increase in intestinal calcium absorption within two days, and this effect can last for several weeks.1,7 In addition to its intestinal effects, calcitriol also affects the kidneys and bone. Calcitriol weakly promotes calcium and phosphate retention by the kidneys7 ; supplementation with a vitamin D analogue may also increase serum phosphorus concentrations.15 In small amounts, calcitriol promotes calcification of bone, but in larger amounts, it promotes absorption of bone.7 The effects of PTH on bone are blunted in calcitriol's absence.4,7
Magnesium
Hypomagnesemia decreases both the secretion and activity of PTH, so it can contribute to hypocalcemia.8,16 A decreased PTH concentration also results in hypomagnesemia through decreased release from bone and decreased reabsorption from renal tubules.17 Additionally, vitamin D activation in the kidneys requires magnesium.
SIGNALMENT
Naturally occurring primary hypoparathyroidism tends to occur in middle-aged spayed female dogs.3 The average age at the time of presentation is 4.8 years, but it has been reported in dogs as young as 6 weeks and as old as 13 years.1,2 Sixty percent to 65% of the affected dogs are female.1-3 Toy poodles, Labrador retrievers, miniature schnauzers, German shepherds, and terrier breeds are predisposed to the condition.1-3
This condition was first reported in a cat in 1990,1 and few cases have been reported since.4,12,15,18 The average affected cat was just over 2 years old, and a sex predilection for male cats may exist, though a breed predilection has not been reported.1,4
PATHOPHYSIOLOGY AND CLINICAL SIGNS
The histopathologic changes in naturally occurring primary hypoparathyroidism depend on the stage in the course of the disease.1 Early in the process, there is a lymphocytic-plasmacytic parathyroiditis with degeneration of the chief cells, consistent with an immune-mediated pathogenesis.1,2,6 The remaining chief cells become hyperplastic and eventually become isolated in small areas at the periphery of the parathyroid gland.1,2,6 Later, fibrous connective tissue replaces the lymphocytic-plasmacytic infiltration of the parathyroid gland.1,2
Hypoparathyroidism is a lack of PTH resulting in decreased mobilization of minerals from bone, calciuresis, renal phosphate retention, and decreased absorption of both calcium and phosphorus from the intestines.1,2,5,7 The net effect of hypoparathyroidism is hypocalcemia and hyperphosphatemia.1
The severity of the signs and the timing of their onset reflect the duration, rate of change, and magnitude of the hypocalcemia.5,8 Calcium normally stabilizes nerve cell membranes by decreasing their permeability to sodium.1,2 Nerve fibers are sensitive to changes in the concentration of ionized calcium (the physiologically active form), which affects acetylcholine's release during neuromuscular transmission.1,2 The level of excitability increases as the ionized calcium concentration decreases.1 When the ionized calcium concentration reaches 50% below normal, there is spontaneous discharge of peripheral nerve fibers and skeletal muscle contraction.1,2,4-7
Mild hypocalcemia rarely causes overt clinical signs, and animals have some ability to adapt to hypocalcemia.1,4,5 An animal often does not show signs until its total serum calcium concentration drops below 6 to 6.5 mg/dl, but if the concentration drops even slightly lower, clinical signs may develop rapidly.1,4,5 In individual dogs, it is difficult to predict the exact onset of clinical tetany; in people, tetany generally occurs when the calcium concentration drops 35% to 40% below normal. This percentage of decrease would correspond to a total calcium concentration below 6 mg/dl or an ionized calcium below 0.7 mmol/L in dogs.1,7 Although rare, a total serum calcium concentration less than 4 mg/dl can be lethal because of hypotension, decreased myocardial contractility, and paralysis of the respiratory muscles leading to respiratory arrest.1,5,7 Even with a stable level of hypocalcemia, clinical signs are often intermittent. Exercise or excitement may cause a respiratory alkalosis (i.e. increased ventilation from tachypnea leads to decreased arterial carbon dioxide), reducing the ionized fraction of serum calcium by increasing the binding of calcium to albumin.1,4,5,8,10,11
Clinical signs
The clinical signs of hypocalcemia are identical, regardless of the cause.5 Clinical signs of hypocalcemia may be nonspecific, such as anorexia, nervousness, stilted gait, panting, ataxia, episodic weakness, vomiting, diarrhea, and weight loss.1,18 In a case series of 37 dogs with naturally occurring primary hypoparathyroidism, the most commonly noted abnormalities at presentation (in descending order of incidence) included fever, tense or splinted abdomen, stiff gait, thinness, generalized muscle fasciculations, growling, tachyarrhythmias, muffled heart sounds, weak pulses, and cataracts.1 Although these dogs were persistently hypocalcemic, signs of tetany were intermittent.1 In cats, anorexia and lethargy are more common signs, but vomiting has also been reported.2,4,5 Raised nictitating membranes and ear twitching may be observed in cats.2,4
Clinical signs may be present from one day to two years before presentation.1,2 Animals presenting for seizures may be misdiagnosed if a pretreatment biochemical profile is not performed.1,2 The owners may perceive that the clinical signs appeared acutely, but the disease probably had been present for a long time.1
Neuromuscular and neurologic signs
Neuromuscular and neurologic signs usually predominate in dogs and cats with primary hypoparathyroidism. Patients usually present for an acute onset of tetany or seizures. In retrospect, owners often identify more subtle signs of muscle stiffness.1-3,10,18 On occasion, the tetany may be latent, and excitement or activity increases neuromuscular activity, inducing tetany.1,2,10 Neuromuscular signs are intermittent and include mild muscle tremors and fasciculations, muscle cramping, and stilted gait and may progress to neurologic signs, such as generalized seizures.1,2,4,6,8,10 Seizures are often preceded by muscle tremors in one limb that gradually spread throughout the body and culminate in a seizure.1,10 Seizure activity is atypical in that dogs remain conscious and seizure activity usually ceases without intervention.2 Secondary to prolonged seizure activity, it is not unusual for the body temperature to exceed 105 F (40.6 C).2 In the same case series of 37 dogs, tetany was noted on presentation in nearly 50% of dogs, and seizure activity was directly observed in 86% of the dogs with hypoparathyroidism during their initial hospitalization.1 In cats, induction of seizure activity with excitement has not been observed.5
Other neuromuscular effects include disorientation, chewing and licking at the paws, and behavioral changes.1,4-6,10 Facial rubbing, which can be dramatic and lead to self-mutilation, is a common observation.1 In the case series of the 37 dogs, 23 of the dogs exhibited facial rubbing. People with hypoparathyroidism report a paresthesia or tingling in the lips and distal extremities, possibly from hyperexcitability of sensory neurons.6 The facial rubbing seen in dogs may be due to a similar phenomenon.6 Another possible explanation for facial rubbing is pain caused by cramping of the masseter or temporal muscles.1,2,18 Behavioral changes associated with hypocalcemia include nervousness, reluctance to be touched, decreased activity level, and aggressive behavior. Gastrointestinal signs may be secondary to smooth muscle spasms due to autonomic nerve hyperexcitability.6 The neuromuscular signs should resolve with treatment of the hypocalcemia.1,2
Cardiac manifestations
In addition to the neuromuscular effects of hypocalcemia, there may be cardiac manifestations. Calcium normally acts as a positive inotrope and as a mild positive chronotrope.1 With decreased calcium concentrations, the duration of the action potential in cardiac cells is prolonged and may result in decreased myocardial function and bradycardia.1,2,4 In people, hypocalcemia may result in 2:1 heart block.1
Ophthalmologic manifestations
In people, cats, and dogs, hypoparathyroidism can be associated with the development of bilateral, small, punctate-to-linear cataracts in the anterior and posterior cortical subcapsular region.1,3,4,15 The mechanism of cataract formation is unknown, and vision is not typically impaired if treatment is initiated early.1,15 The cataracts are slowly progressive if the hypoparathyroidism is left untreated.1
DETECTION AND CONFIRMATION OF HYPOCALCEMIA
In patients with clinical signs consistent with hypocalcemia, perform a serum chemistry profile. Measure the total serum calcium, phosphorus, blood urea nitrogen, creatinine, and albumin concentrations. Ideally, a complete blood count and urinalysis should also be performed. In most laboratories, the lower end of the reference range of total calcium is 9.5 mg/dl in dogs and 9 mg/dl in cats.1 Dogs with untreated hypoparathyroidism often have serum total calcium concentrations consistently below 6.5 mg/dl.1,2
When the total calcium concentration is below the reference range, two factors must be considered. First, a common cause of hypocalcemia is sampling or laboratory error. So confirm hypocalcemia by obtaining a second blood sample to repeat the total calcium concentration or measure an ionized calcium concentration.1 Second, consider the albumin concentration. Hypoalbuminemia will lower the total calcium concentration in the blood, but the ionized fraction will likely be normal.1,8 Formulas for corrected calcium concentrations exist, but their accuracy remains controversial.1 The most common formula for corrected calcium is corrected calcium is equal to the measured total calcium concentration (mg/dl) – albumin concentration (g/dl) + 3.5.1 With the availability of equipment to measure ionized calcium concentrations, the use of corrected formulas is falling out of favor.
In dogs with hypoparathyroidism, the albumin, blood urea nitrogen, and creatinine concentrations are typically normal.1,2,5 Evaluation of total serum magnesium may be warranted. In the case series of 37 dogs, 23 had total serum magnesium concentration evaluated.1 Nineteen of the 23 were normal and four were decreased. However, total serum magnesium concentration may not accurately reflect the biologically active component (ionized magnesium).
In any patient with hypocalcemia, evaluate the ionized fraction.8 Ionized calcium concentrations below 1.1 mmol/L in dogs and below 1 mmol/L in cats are diagnostic for hypocalcemia.1 Whole blood, plasma, or serum samples are appropriate as long as they are collected under anaerobic conditions.4,11 If a plasma sample is processed within three days, refrigeration of the sample is sufficient. If there is a delay in processing, the sample should be frozen.1 Before collecting the samples, contact your laboratory for guidelines on handling samples. It may be prudent to simultaneously request a PTH concentration.
CONCLUSION
To recognize primary hypoparathyroidism, you must have a thorough understanding of the interaction of PTH and calcitriol and the effect that both have on serum ionized calcium concentration. Neurologic and neuromuscular clinical signs predominate. Once these signs are noted, you should perform diagnostic testing. Once you have definitively diagnosed primary hypoparathyroidism, begin appropriate therapy. The next article discusses the differential diagnoses in dogs and cats with hypocalcemia, additional diagnostic testing, and treatment of primary hypoparathyroidism.
Beth L. McElravy, DVM
Jill D. Brunker, DVM, DACVIM
Department of Small Animal Internal Medicine
College of Veterinary Medicine
Oklahoma State University
Stillwater, OK 74078
REFERENCES
1. Feldman EC, Nelson RW. Hypocalcemia and primary hypoparathyroidism. In: Canine and feline endocrinology and reproduction. 3rd ed. Philadelphia, Pa: Elsevier Science, 2004;716-742.
2. Feldman EC. Disorders of the parathyroid glands. In: Ettinger SJ, Feldman EC, eds. Textbook of veterinary internal medicine: diseases of the dog and cat. 6th ed. St. Louis, Mo: Elsevier Saunders, 2005;1508-1535.
3. Bruyette DS, Feldman EC. Primary hypoparathyroidism in the dog. J Vet Intern Med 1988;2:7-14.
4. Waters CB, Scott-Moncrieff JCR. Hypocalcemia in cats. Compend Cont Educ Vet Pract 1992;14:497-507.
5. Chew DJ, Nagode LA. Treatment of hypoparathyroidism. In: Bonagura JD, ed. Kirk's current veterinary therapy XIII small animal practice. Philadelphia, Pa: WB Saunders Co, 2000;340-345.
6. Sherding RG, Meuten DJ, Chew DJ, et al. Primary hypoparathyroidism in the dog. J Am Vet Med Assoc 1980;176:439-444.
7. Guyton AC, Hall JE. Urine formation by the kidneys; parathyroid hormone, calcitonin, calcium and phosphate metabolism, vitamin D, bone, and teeth. In: Textbook of medical physiology. 10th ed. Philadelphia, Pa: WB Saunders Co, 2000;302-309,899-915.
8. Church D. Electrolyte disorders. In: Ettinger SJ, Feldman EC, eds. Textbook of veterinary internal medicine: diseases of the dog and cat. 6th ed. St. Louis, Mo: Elsevier Saunders, 2005;236-238.
9. Potts JT. Diseases of the parathyroid gland and other hyper-and hypocalcemic disorders. In: Braunwald E, Fauci AS, Kasper DL, et al., eds. Harrison's principles of internal medicine. 15th ed. New York, NY: McGraw-Hill, 2004;2205-2226.
10. Towell TL, Shell LG. Endocrinopathies that affect the central nervous system of cats and dogs. Compend Cont Educ Vet Pract 1994;16:1461-1465.
11. Dhupa N, Proulx J. Hypocalcemia and hypomagnesemia. Vet Clin North Am Small Anim Pract 1998;28:587-608.
12. Barber PJ. Disorders of the parathyroid glands. J Feline Med Surg 2004;6:259-269.
13. Mikiciuk MG, Thornhill JA. Control of parathyroid hormone in chronic renal failure. Compend Cont Educ Vet Pract 1989;11:831-836.
14. Allen TA, Weingand K. The vitamin D (calciferol) endocrine system. Compend Cont Educ Vet Pract 1985;7:482-488.
15. Bassett JR. Hypocalcemia and hyperphosphatemia due to primary hypoparathyroidism in a six-month-old kitten. J Am Anim Hosp Assoc 1998;34:503-507.
16. Kimmel SE, Waddell LS, Michel KE. Hypomagnesemia and hypocalcemia associated with protein-losing enteropathy in Yorkshire terriers: five cases (1992-1998). J Am Vet Med Assoc 2000;217:703-706.
17. Bush WW, Kimmel SE, Wosar MA, et al. Secondary hypoparathyroidism attributed to hypomagnesemia in a dog with protein-losing enteropathy. J Am Vet Med Assoc 2001;219:1732-1734.
18. Greco DS. Endocrine emergencies. Part II. Adrenal, thyroid, and parathyroid disorders. Compend Cont Educ Vet Pract 1997;19:27-39.