The proper use of topical and oral corticosteroids
Corticosteroids are among the most used and misused medications in veterinary medicine. They exert a powerful, reliable, and rapid effect, and there is no viable, more effective therapeutic alternative in animals with certain skin conditions. Topical and oral corticosteroid therapies are considered the first choice for treatment of acute and chronic inflammatory skin diseases, particularly allergic dermatitis. In addition, they aid in the inflammation associated with some types of infections, primarily Malassezia dermatitis and otitis.
Corticosteroids are among the most used and misused medications in veterinary medicine. They exert a powerful, reliable, and rapid effect, and there is no viable, more effective therapeutic alternative in animals with certain skin conditions. Topical and oral corticosteroid therapies are considered the first choice for treatment of acute and chronic inflammatory skin diseases, particularly allergic dermatitis. In addition, they aid in the inflammation associated with some types of infections, primarily Malassezia dermatitis and otitis.
Using oral corticosteroids
As a review, the oral corticosteroids available for dogs are listed in Table 1 along with their relative potencies, half-life, and relative mineralocorticoid effects. As you can see from the table, these drugs' half-life becomes much longer as the potency increases. This is important from a clinical standpoint because many patients that are treated for more than two to three weeks with oral corticosteroids experience side effects.1 To minimize these effects, clinicians should use an alternate-day protocol when administering oral corticosteroids longer than two weeks.

Table 1. Oral Corticosteroids Used in Dogs
The incidence of side effects—either annoying or more serious—increases as the potency of the corticosteroid increases. Some controversy surrounds the use of oral triamcinolone in regard to its potency and half-life. To be conservative, it is best to assume that oral triamcinolone has a greater potency than prednisone or prednisolone and has a longer biologic half-life—closer to 36 hours. Therefore, practitioners should reserve the use of oral triamcinolone in dogs for treatment of serious refractory skin diseases. Oral dexamethasone should be used in canine cases only if no other treatment has been successful and the owners have been warned about the potential serious side effects, or the owners are debating the pet's quality of life (i.e., they are considering euthanasia).
The mineralocorticoid effects of corticosteroids are responsible for increased water consumption, subsequent increased urine output, and potential urinary incontinence. Prednisone and prednisolone exert a slightly stronger mineralocorticoid effect than methylprednisolone. Therefore, methylprednisolone may be used instead of prednisone or prednisolone in cases of undesirable increases in water consumption and urine output.
The most commonly administered oral corticosteroids are prednisone and prednisolone, the latter being more effective in cats. In dogs, a short regimen of prednisone or prednisolone usually results in mild to no side effects.
Most clinicians in private practice are regularly faced with challenging dermatologic cases, and a common question arises: How much prednisone is too much? No one can definitively answer this question, as different dogs respond in different ways. Some patients are unaffected by long-term prednisone administration, while others immediately demonstrate polyphagia, polydipsia and polyuria, or incontinence. Still others show signs of iatrogenic Cushing's disease—muscle wasting, a pot-bellied appearance, and muscle weakness—early on in therapy. The best approach is to try the safest treatment first, monitor the patient's response carefully, and adjust the therapeutic protocol if side effects become problematic or the condition does not respond.
Many dogs receiving corticosteroids will experience alterations in blood work, including variable increases in alkaline phosphatase activity; stress leukograms characterized by neutrophilia, lymphopenia, and eosinopenia; hyperglycemia; hypercholesterolemia; and occasionally a blunted cortisol response to adrenocorticotropic hormone (ACTH) administration.2 These changes are generally acceptable as they are rarely of clinical importance.
Other side effects commonly seen with long-term therapy include weight gain, a pot-bellied appearance associated with fat redistribution, alopecia (some hairs fracture, but most are arrested in the telogen phase), thin and poorly elastic skin, comedones, pustules, and secondary bacterial infections primarily involving the skin and the urinary tract. In one study, more than one-third of dogs experienced a urinary tract infection when treated with corticosteroids for longer than six months.3
More serious side effects associated with long-term corticosteroid administration include muscle weakness, severe muscle wasting primarily affecting the muscles of mastication, gastroduodenal ulceration, severe and often hemorrhagic colitis (particularly with oral dexamethasone), induction of sometimes irreversible diabetes mellitus, severe liver disease, and renal disease as evidenced by proteinuria.
Using topical corticosteroids
In light of these many possible side effects, I suggest that in some cases topical corticosteroids be used in place of systemically administered corticosteroids. Most of the side effects discussed above can be avoided or reduced when topical corticosteroids are prescribed in a responsible way. However, with uncontrolled use, some side effects at the site of application are common with topical corticosteroids, including cutaneous changes such as thin skin, loss of elasticity, and comedones. Side effects can also include ecchymoses resulting from vascular fragility and ulceration with pyoderma. This pyoderma is termed bullous (blister-like) impetigo and results in large, irregularly shaped pustules. It can also be accompanied by the small pustules typically associated with allergy and can be somewhat refractory to antibiotic therapies.
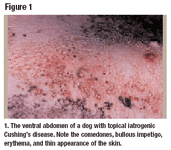
Figure 1. The ventral abdomen of a dog with topical iatrogenic Cushing's disease. Note the comedones, bullous impetigo, erythema, and thin appearance of the skin.
The disease involving bullous impetigo and other cutaneous changes seen from the repeated use of potent topical corticosteroids is termed topical iatrogenic Cushing's disease (Figure 1). This response is localized to the site of corticosteroid application, can result in a blunted cortisol response to ACTH, and is reversible. Patients are less likely to experience these adverse cutaneous changes with low- or intermediate-potency topical corticosteroids such as hydrocortisone and triamcinolone.
Although topical corticosteroids are generally less likely to cause side effects than oral formulations, there are some contraindications to their use in dogs. Topical corticosteroids are contraindicated any time pyoderma is present. It is recommended that pyoderma be treated and resolved with appropriate antibiotic therapy before the application of topical corticosteroids. In some cases (particularly in small dogs), more corticosteroid will be systemically absorbed into the bloodstream per unit of body weight and thus can affect the ACTH stimulation test and elevate alkaline phosphatase activities. This is a well-recognized phenomenon with otic and ophthalmic preparations of triamcinolone, prednisone, prednisolone, and dexamethasone.
Overall, however, topical corticosteroids are far less likely to produce systemic side effects.
Indications for corticosteroid therapy
Flea allergy dermatitis. Before the advent of imidacloprid, fipronil, and selamectin, fleas and flea allergy dermatitis were the most common dermatologic cases seen in both general and referral practice. With more pet owners using the new adulticides, the number of flea allergy patients I see in my busy San Francisco referral practice has declined somewhat. However, the cases I do see are much more challenging—in many instances adult fleas are not observed on the dog upon presentation. This can be a result of the partial success of the new adulticides or inconsistent application of these products in the presence of environmental infestations.
When fleas aren't seen on presentation, practitioners must rely on other clinical signs to diagnose flea allergy dermatitis. Canine flea allergy dermatitis is one of few skin diseases that presents with acute pruritus. The pruritus is generally distributed over the caudal half of the body, particularly the dorsal lumbosacral area, tail base, and inguina. On occasion, some dogs develop more generalized skin disease (Figure 2). Scabies is another skin disease that presents with acute pruritus. In the absence of adult fleas or positive skin scrapings for sarcoptic mites, the clinical distribution of the dermatitis is the key to differentiating these two diseases—canine Sarcoptes infestation commonly presents with pinnal, elbow, and ventral pruritus.

Figure 2. A dog with flea allergy and secondary generalized pyogranulomatous dermatitis.
Flea allergy dermatitis patients experience a systemic response to antigen in the flea's saliva through increased production of IgE. This promotes an influx of inflammatory cells into the skin, resulting in local and sometimes diffuse pruritus. My preferred method of treating these intensely pruritic dogs is to prescribe a short duration (two to three weeks maximum) of orally administered prednisone or methylprednisolone and institute strict flea control on the patient and in the environment. The antipruritic and anti-inflammatory dosage of prednisone and prednisolone in dogs is generally 0.5 to 1 mg/kg orally once daily and tapered over two to three weeks. Since methylprednisolone is 20% more potent than prednisone and prednisolone, 4 mg methylprednisolone is equivalent to 5 mg prednisone.
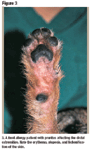
Figure 3. A food allergy patient with pruritus affecting the distal extremities. Note the erythema, alopecia, and lichenification of the skin.
In some cases of flea allergy dermatitis, I prefer to use intermediate-potency triamcinolone acetonide topical spray (Genesis—Virbac) per the labeled instructions. This approach provides many advantages over oral corticosteroids. First, some dogs are difficult for owners to medicate orally, so a topical treatment can be a welcome alternative. Secondly, the owner can apply the treatment to the specific problem areas. Thirdly, flea allergy dermatitis cases have a therapeutic endpoint. Flea control will eliminate the need for corticosteroids at some point, so it seems reasonable to consider topical treatment in order to avoid systemic side effects. In addition, systemic corticosteroids are contraindicated in animals with preexisting underlying disease such as diabetes mellitus.
Food allergy. Another common allergic dermatologic disease is food allergy. The only consistent clinical sign is pruritus that is typically nonseasonal. The pruritus associated with food allergy can be managed similarly to flea allergy pruritus, as the proper diet should eventually eliminate the need for corticosteroids. In my opinion, it is not sound medicine to allow a patient to remain in discomfort during the initial phase of a dietary trial. Some food allergy patients may take up to 12 weeks to respond to the diet change. During this time they may continue to exhibit pruritus and develop secondary pyoderma. Therefore, it seems prudent to consider using corticosteroids during the first two to four weeks of the diet trial. Again, oral prednisone, prednisolone, or methylprednisolone, or topical triamcinolone is preferred. Some cases of food allergy have a limited clinical distribution, involving only the feet, perianal area, axillae, trunk, or inguina (Figure 3). These cases are excellent candidates for treatment with topical triamcinolone alone.

Figure 4. A patient with severe atopy and secondary Malassezia dermatitis affecting the face. Note the hyperpigmentation, alopecia, and lichenification of the skin.
Atopy. Canine atopic dermatitis is my most commonly referred case and the most frustrating. This disease is genetically based (although the exact mode of inheritance is unknown) and is thus not curable. Clinical signs can be seasonal or nonseasonal and include many potential pruritic patterns. Since atopic disease is chronic, I usually prescribe oral corticosteroids because they constitute the most reliable and relatively safe therapy.

Figure 5A. A patient with atopy before treatment with topical triamcinolone and allergen-specific immunotherapy. Note the numerous wheals on the ventral abdomen, flank, and inguina. An area on the left thorax has been shaved for intradermal allergen testing.
In some situations (cases that are refractory to oral corticosteroids or involving severe side effects to oral corticosteroids, lifelong disease, or owners who object to corticosteroid use), I prescribe cyclosporine. Because cyclosporine can have a delayed onset of action, I recommend use of topical triamcinolone for the first two to three weeks. Topical corticosteroids can also be sprayed onto a cotton ball or medical gauze and applied to difficult-to-spray areas, such as the pinnae and areas around the face (Figure 4). Topical triamcinolone can also be successfully used for immediate and short-term relief of pruritus pending the desired response to allergen-specific immunotherapy (Figures 5A and 5B).
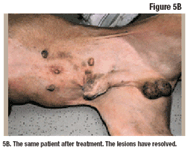
Figure 5B. The same patient after treatment. The lesions have resolved.
References
1. Scott DW. Dermatology therapy. In: Scott DW, Miller WH, Griffin CE, eds. Muller and Kirks' Small Animal Dermatology. 6th ed. Philadelphia, Pa: WB Saunders Co, 2001;244-273.
2. McDonald RK, Langston VC. Use of corticosteroids and non-steroidal anti-inflammatory agents. In: Ettinger SJ, Feldman EC, eds. Textbook of Veterinary Internal Medicine: Diseases of the Dog and Cat. 4th ed. Philadelphia, Pa: WB Saunders Co, 1995;284-293.
3. Ihrke PJ, Norton AL, Ling GV, et al. Urinary tract infection associated with long-term corticosteroid administration in dogs with chronic skin diseases. J Am Vet Med Assoc 1985;186:43-46.