The role of fatty acids in the management of osteoarthritis
Osteoarthritis is a chronic and potentially debilitating disease involving the disruption of metabolic homeostasis within the articular chondrocyte. Specifically, osteoarthritis involves an increased ratio of cartilage-degrading enzymes (matrix metalloproteinases, or MMPs) to their normal inhibitors, tissue inhibitors of metalloproteinases (TIMPs). It is the imbalance of TIMPs and MMPs that contributes to the pathologic breakdown of cartilage. Dietary fatty acids can help to correct this imbalance by modulating the production of inflammatory mediators.
Osteoarthritis is a chronic and potentially debilitating disease involving the disruption of metabolic homeostasis within the articular chondrocyte. Specifically, osteoarthritis involves an increased ratio of cartilage-degrading enzymes (matrix metalloproteinases, or MMPs) to their normal inhibitors, tissue inhibitors of metalloproteinases (TIMPs). It is the imbalance of TIMPs and MMPs that contributes to the pathologic breakdown of cartilage. Dietary fatty acids can help to correct this imbalance by modulating the production of inflammatory mediators.
N-3 fatty-acid types
Dietary fats are an important component of canine diets. They supply a concentrated source of energy as well as essential fatty acids, such as linoleic acid and α-linolenic acid. Due to dogs' inability to produce these fatty acids and their metabolic need for them, linoleic acid and α-linolenic acid must be supplied in the diet. Furthermore, these fatty acids serve as substrates for further desaturation and chain elongation to longer 20- and 22-carbon fatty acids.
Vegetable oils-such as flaxseed, soybean, and canola oils-contain amounts of α-linolenic acid ranging from 7% to more than 50% of the oil's total fatty-acid content. Alpha-linolenic acid can be metabolized into the long-chain n-3 fatty acids, eicosapentaenoic acid and docosahexaenoic acid. However, the conversion rate of α-linolenic acid to eicosapentaenoic acid and docosahexaenoic acid is low. In dogs fed diets containing α-linolenic acid or fish oil at the same n-6:n-3 fatty-acid ratio, fish oil supplementation resulted in significantly greater eicosapentaenoic acid and docosahexaenoic acid enrichment in both the plasma and neutrophils than the group consuming the α-linolenic acid supplemented diet.1 Furthermore, even when α-linolenic acid was fed at levels of more than 20% of total energy, there was no docosahexaenoic acid enrichment in the plasma or neutrophils.1 The findings are similar in primates and people-studies reveal inefficient conversion of dietary α-linolenic acid to eicosapentaenoic acid.2-4 Even though α-linolenic acid and eicosapentaenoic acid are both n-3 fatty acids, they need to be considered separately because they're metabolized differently. The dietary n-6:n-3 fatty-acid ratio or the total n-3 fatty-acid content does not include the possible anti-inflammatory potential of a diet.5
Fatty acids and eicosanoid synthesis
The 20-carbon fatty acids-eicosapentaenoic acid and arachidonic acid-serve as precursors for biologic mediators, including the prostaglandins and leukotrienes (Figure 1). Most cells in the body produce prostaglandins, including chondrocytes and synoviocytes. Inflammatory cells, polymorphonuclear leukocytes, macrophages, and mast cells produce leukotrienes primarily. The arachidonic-acid-derived prostaglandin E2 (PGE2), which is normally present in small amounts, serves important physiologic roles. However, its production increases in inflammatory conditions such as osteoarthritis. PGE2 stimulates pain receptors and promotes additional inflammation. Leukotriene B4 (LTB4), also derived from arachidonic acid, promotes inflammation as well. On the other hand, prostaglandin E3 (PGE3) and leukotriene B5 (LTB5), the eicosanoid products of eicosapentaenoic acid, have markedly less biologic activity than those derived from arachidonic acid and are considered anti-inflammatory.
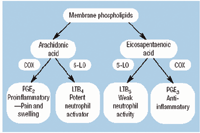
Figure 1. Eicosanoid formation from 20-carbon chain n-6 (arachidonic acid) and n-3 (eicosapentaenoic acid) fatty acids. (Abbreviations: COX = cyclooxygenase, 5-LO = 5-lipoxygenase, PGE = prostaglandin E, and LTB = leukotriene B.)
Cytokines and matrix metalloproteinases
The proinflammatory cytokines, interleukin-1β (IL-1β) and tumor necrosis factor-α (TNF-α), are known to have long-term deleterious effects on bone and cartilage.6 IL-1β stimulates PGE2 production, and both IL-1β and TNF-α activate MMPs, the enzymes responsible for cartilage degradation. Furthermore, both IL-1β and TNF-α concentrations are elevated in canine osteoarthritis.7,8 A number of in vitro and ex vivo studies demonstrate long-chain n-3 supplementation's ability to reduce the production of these proinflammatory cytokines. In vitro studies have shown that n-3 fatty-acid supplementation reduces MMP production.9,10 Further- more, ex vivo studies demonstrate that dietary fish oil supplementation reduces TNF-α and IL-1β production in stimulated whole blood or polymorphonuclear leukocytes.11-13 Long-chain n-3 fatty-acid supplementation's ability to suppress IL-1β and TNF-α synthesis is important because of these cytokines' roles in the inflammatory process.
Fish oil supplementation and arthritis
In people, rats, and cell culture models, fish oil supplementation improves the symptoms and biochemical parameters associated with arthritis. Fish oil supplementation can significantly improve the symptoms associated with rheumatoid arthritis in people.14-20 Patients' assessments of morning stiffness, swelling, joint tenderness, and grip strength were among the outcomes measured and shown to improve in these studies. The dosages used were relatively low, ranging from 1.3 g to 3.8 g of eicosapentaenoic acid per day. Thus, patient-assessed clinical measures significantly improved even with relatively low doses of eicosapentaenoic acid.
In addition, fish oil supplementation has been shown to improve the biochemical parameters associated with osteoarthritis.21,22 These studies demonstrated that long-chain n-3 fatty acids reduced the inflammation associated with osteoarthritis and decreased the production of MMP, IL-1, 5-lipoxygenase, and cyclooxygenase-2, with no reduction in TIMP production. Similar findings have been observed in rodent studies in which osteoarthritis was induced.23,24
Fish oil supplementation in canine osteoarthritis
A study recently conducted at the Colorado State University Veterinary Teaching Hospital evaluated the effects of fish oil on key biochemical markers in dogs with osteoarthritis.25 Twenty-four dogs with confirmed osteoarthritis were referred for cruciate ligament repair. They were randomly assigned to one of two groups-a group receiving fish oil supplements or a control group. Beginning on day â7, the dogs were fed the specified diets until day 56 (63 days total). Plasma and synovial fluid samples were collected on days â7, 0, 14, 28, and 56. Samples were assayed for fatty-acid composition, MMP-2 and MMP-9, TIMP-2, and bicyclo-PGE2 (the stable metabolite of PGE2).
Numerous significant differences were observed. As expected, fish oil supplementation had significant effects on eicosapentaenoic acid and docosahexaenoic acid enrichment in plasma and synovial fluid as well as a corresponding reduction in arachidonic acid. A significant increase in TIMP-2 and significant reductions in MMP-2 and MMP-9 were also observed. Furthermore, plasma bicylco-PGE2 was significantly reduced from point of entry due to diet (P = 0.0195). The study demonstrated that fish oil supplementation improves the biochemical parameters associated with canine osteoarthritis.
Studies have also shown that fatty-acid supplementation decreases lameness in dogs with osteoarthritis. In one study, 13 of 22 dogs with osteoarthritis of the hip showed improvement with a mixed fatty-acid supplement as reported by the owners.26 More recently, forceplate technology was used to evaluate the benefit of long-chain n-3 fatty acids in dogs with osteoarthritis of the elbow. Ten adult dogs with clinical lameness were fed a diet containing fish oil. Concurrent medications for osteoarthritis were not allowed. Each dog's gait was evaluated using forceplate analysis on Day 1 and again after seven to 10 days. Gait analysis was conducted using two biomechanical force platforms positioned sequentially to allow data collection from both rear limbs during each trial. During the period the dogs were fed the eicosapentaenoic-acid-supplemented diet, lameness scores improved (Figure 2).
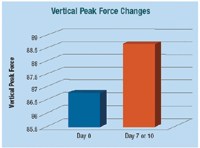
Figure 2. Gait analysis was conducted using two biomechanical force platforms positioned sequentially to allow data collection from both rear limbs during each trial. Each trial consisted of the dog moving across the 2-meter measurement area, with no distracting head movements or gait abnormality, at a speed of 1.7 to 2.1 m/sec. For each limb, data from five valid trials were used. Improvements in vertical peak force were observed following seven to 10 days on the test diet (p = 0.08).
Conclusion
These studies in dogs and other species confirm that long-chain n-3 fatty acids-specifically eicosapentaenoic acid and docosahexaenoic acid-can have a significant effect on osteoarthritis. It's clear that nutritional intervention plays a prominent role in the management of canine osteoarthritis. Nutritional management of canine osteoarthritis should also include an appropriate dietary caloric density and feeding regimen to promote ideal body condition score, and high levels of antioxidants to help reduce the free radical damage associated with osteoarthritis. Dietary glucosamine for cartilage and joint health may also be beneficial. It's important to note that a diet that leverages fatty acids to promote a reduction in proinflammatory cytokines and eicosanoids must contain the correct type and amount of n-3 fatty acids and eicosapentaenoic acid and docosahexaenoic acid.
References
1. Waldron, M.K.: Dietary fat effects on canine neutrophil membrane fatty acid composition and cell functions (PhD dissertation). Texas A&M University, College Station, 1999, pp. 57-98.
2. Su, H.M. et al.: Fetal baboons convert 18:3n-3 to 22:6n-3 in vivo. A stable isotope tracer study. J. Lipid Res. 42 (4):581-586; 2001.
3. James, M.J. et al.: Metabolism of stearidonic acid in human subjects: comparison with the metabolism of other n-3 fatty acids. Am. J. Clin. Nutr. 77 (5):1140-1145; 2003.
4. Brenna, J.T.: Efficiency of conversion of alpha-linolenic acid to long-chain n-3 fatty acids in man. Curr. Opin. Clin. Nutr. Metab. Care 5 (2):127-132; 2002.
5. de Deckre, E.A. et al.: Health aspects of fish and n-3 polyunsaturated fatty acids from plant and marine origin. Eur. J. Clin. Nutr. 52 (10):749-753; 1998.
6. Arend, W.P.: The mode of action of cytokine inhibitors. J. Rheumatol. (suppl. 65):16-21; 2002.
7. Kammermann, J.R. et al.: Tumor necrosis factor-alpha (TNF-alpha) in canine osteoarthritis: Immunolocalization of TNF-alpha, stromelysin and TNF receptors in canine osteoarthritic cartilage. Osteoarthritis Cartilage 4 (1):23-34; 1996.
8. Fernandes, J.C. et al.: The effects of tenidap on canine experimental osteoarthritis: II. Study of the expression of collagenase-1 and interleukin 1 beta by in situ hybridization. J. Rheumatol. 25 (5):951-958; 1998.
9. Curtis, C.L. et al.: Effects of n-3 fatty acids on cartilage metabolism. Proc. Nutr. Soc. 61 (3):381-389; 2002.
10. Curtis, C.L. et al.: Pathologic indicators of degradation and inflammation in human osteoarthritic cartilage are abrogated by exposure to n-3 fatty acids. Arthritis Rheum. 46 (6):1544-1553; 2002.
11. Endres, S. et al.: The effect of dietary supplementation with n-3 polyunsaturated fatty acids on the synthesis of interleukin-1 and tumor necrosis factor by mononuclear cells. N. Eng. J. Med. 320 (5):265-271; 1989.
12. Meydani, S. et al.: Oral (n-3) fatty acid supplementation suppresses cytokine production and lymphocyte proliferation: comparison between younger and older women. J. Nutr. 121 (4):547-555; 1991.
13. Caughey, G.E. et al.: The effect on human tumor necrosis factor-alpha and interleukin-1-beta production of diets enriched in n-3 fatty acids from vegetable oil or fish oils. Am. J. Clin. Nutr. 63 (1):116-122; 1996.
14. Kremer, J.M. et al.: Effects of manipulation of dietary fatty acids on clinical manifestations of rheumatoid arthritis. Lancet 1 (8422):184-187; 1985.
15. Kremer, J.M. et al.: Effects of manipulation of dietary fatty acids in active rheumatoid arthritis. Ann. Intern. Med. 106 (4):497-503; 1987.
16. Cleland, L.G. et al.: Clinical and biochemical effects of dietary fish oil supplements in rheumatoid arthritis. J. Rheumatol. 15 (10):1471-1475; 1988.
17. van der Tempel, H. et al.: Effects of fish oil supplementation in rheumatoid arthritis. Ann. Rheum. Dis. 49 (2):76-80; 1990.
18. Skoldstam, L. et al.: Effect of six months of fish oil supplementation in stable rheumatoid arthritis: A double-blind, controlled study. Scand. J. Rheumatol. 21 (4):178-185; 1992.
19. Kjeldsen-Kragh, J. et al.: Dietary omega-3 fatty acid supplementation and naproxen treatment in patients with rheumatoid arthritis. J. Rheumatol. 19 (10):1531-1536; 1992.
20. Nielsen, G.L. et al.: The effects of dietary supplementation with n-3 polyunsaturated fatty acids in patients with rheumatoid arthritis: a randomized double blind trial. Eur. J. Clin. Invest. 22 (10):687-691; 1992.
21. Curtis, C.L. et al.: Effects of n-3 fatty acids on cartilage metabolism. Proc. Nutr. Soc. 61 (3):381-389; 2002.
22. Curtis, C.L. et al.: Pathologic indicators of degradation and inflammation in human osteoarthritic cartilage are abrogated by exposure to n-3 fatty acids. Arthritis Rheum. 46 (6):1544-1553; 2002.
23. Leslie, C.A. et al.: A fish oil diet reduces the severity of collagen induced arthritis after onset of the disease. Clin. Exp. Immunol. 73 (2):328-332;1988.
24. Cathcart, E.S.; Gonnerman, W.A.: Fish oil fatty acids and experimental arthritis. Rheum. Dis. Clin. North Am. 17 (2):235-242; 1991.
25. Hansen, R.A. et al.: Long chain n-3 PUFA improve biochemical parameters associated with canine osteoarthritis. Proc. AOCS, AOCS, Cincinnati, Ohio, 2004.
26. Miller, W.H. et al.: Treatment of dogs with hip arthritis with a fatty acid supplement. Canine Pract. 17:6-8; 1992.