Surgical and medical treatment of pyometra
Drs. Brian Lucas Hamm and Jeff Dennis discuss your treatment options for this uterine infection.
Both surgical and medical management options are available to treat patients with pyometra, and both carry associated risks. The decision to pursue medical vs. surgical management should be based on the clinical stability of the bitch as well as on discussions with the patient's owner concerning the associated risks of treatment and the patient's reproductive value and potential. Bitches with closed-cervix pyometra are at higher risk for uterine rupture and systemic illness.
INITIAL TREATMENT
Dogs presenting with clinical signs of illness or shock should be appropriately stabilized before direct treatment of the uterine disease is attempted. The goals of patient stabilization are to restore normal perfusion of the tissues, correct electrolyte and glucose imbalances, and initiate treatment of infection. Clinically ill patients will benefit from intravenous (IV) fluid therapy and the administration of parenteral antibiotics. In patients not responding to IV support and medical treatment, surgical excision of the infected uterus may be required to remove the source of infection and achieve a successful recovery. The mortality rate associated with pyometra is about 5%, and most of these deaths are due to secondary endotoxemia and shock.1
Bacterial culture and antibiotic susceptibility testing of the uterine contents and urine are recommended in all patients with pyometra to confirm the effectiveness of empiric antibiotic therapy. Samples for bacterial culture are most commonly taken from the surgically excised uterus. In those patients undergoing medical management, representative bacterial cultures may be retrieved from the cranial vagina by using double-guarded swabs. It should be noted that bacteria grown from cranial vaginal cultures may not be the same as those present in the uterus. The retrieval of samples for bacterial culture and cytologic evaluation through transcervical endoscopy has also been reported.2
All patients being treated for pyometra should immediately begin empiric bactericidal antibiotic therapy. Amoxicillin-clavulanate, or a combination of a penicillin and a fluoroquinolone, is a good antibiotic choice based on historical bacterial causes of uterine infection. The suitability of the empiric antibiotic therapy would then be confirmed by the antibiotic susceptibility results reported from the patient's original bacterial cultures. Antibiotic therapy should be continued for seven to 14 days beyond resolution of the patient's pyometra based on physical examination, laboratory, and ultrasonographic findings.3,4
SURGICAL MANAGEMENT
Regardless of cervical patency, ovariohysterectomy is the treatment of choice for dogs with pyometra that are not deemed reproductively important by their owners.4 The main advantage of ovariohysterectomy over medical management is that it is both curative and preventive for recurrence of pyometra. A discussion of the ovariohysterectomy procedure is outside the scope of this article and can be reviewed in any veterinary surgical textbook.
Ovariohysterectomy carries significant risk, especially in clinically compromised and septic patients. Potential complications such as low blood pressure, aspiration pneumonia, and cardiac arrhythmia should be discussed with the patient's owner before anesthetizing the dog. In addition, the uterine walls are often friable and easily torn during manipulation, leading to spillage of infected contents into the abdomen (Figure 1). A generous abdominal incision allows for easier exposure and exteriorization of the uterus, therefore minimizing the risk of intra-abdominal rupture. In cases of inadvertent intra-abdominal leakage, abdominal culture followed by copious lavage with warm saline solution should be performed.
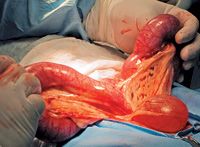
Figure 1. An exteriorized uterus during an ovariohysterectomy for pyometra.
After surgery, patients with pyometra may develop wound infections, fistulous tracts, or local swelling of the surgical incision site or may hemorrhage.5 Referral to an institution with personnel capable of providing advanced anesthetic monitoring and postoperative care may be warranted, especially in systemically ill patients that require intensive monitoring.
MEDICAL MANAGEMENT
Both dogs with open-cervix or closed-cervix pyometra can be successfully treated with medical management. Medical management of pyometra is best performed in patients of appropriate breeding age that are reproductively valuable and free of immediate life-threatening illness, including septicemia, endotoxemia, or organ dysfunction. Closed-cervix pyometra carries an increased risk for complications, primarily uterine rupture.4
The initial goal of medical management is to reduce the progesterone stimulation of the uterus, which contributes to making the uterus a favorable environment for bacterial infection. This goal can be achieved by administering medications that promote regression of the progesterone-producing corpora lutea or that block progesterone receptors in the uterus.
Numerous medical protocols for the treatment of pyometra have been described and are beyond the scope of this article. Please refer to Table 1 for a list of references detailing treatment protocols used for this purpose. Dosing and monitoring requirements vary among the protocols.
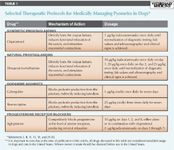

Table 1 Selected Therapeutic Protocols for Medically Managing Pyometra in Dogs*
Prostaglandins
Prostaglandin F2-alpha is the most commonly used medication to medically manage pyometra in dogs. Prostaglandins induce regression of the corpora lutea (luteolysis) through numerous mechanisms, including constriction of blood vessels responsible for oxygen delivery.6,7 As the corpora lutea regress, progesterone production drops. The reduction in progesterone concentrations promotes relaxation (opening) of the cervix, allowing the uterine contents to escape. Prostaglandins also directly stimulate myometrium contraction, thereby promoting expulsion of the infected uterine contents.3 Although not documented, uterine rupture could occur theoretically if intense myometrial contractions were to precede cervical relaxation.
Dogs treated with injectable prostaglandins frequently demonstrate adverse effects such as abdominal discomfort, vomiting, defecation, urination, tachycardia, restlessness, anxiety, fever, hypersalivation, dyspnea, or panting.4 Adverse effects are dosage-dependent and cholinergic-like and result from the systemic stimulatory effects of prostaglandins on smooth muscle elsewhere in the body.8 These adverse effects will usually occur within minutes of administration and can persist for up to an hour or more afterward.4 The prevalence and severity of adverse effects usually decrease with repeated prostaglandin treatments. An earlier study suggested that intravaginal administration of prostaglandin may be associated with a reduction of adverse effects.9 Walking the patient immediately after prostaglandin administration for 20 to 60 minutes can be beneficial in minimizing the severity of these adverse effects.4 If the adverse effects are persistent or severe, pretreatment with anticholinergics and antiemetics has been suggested.10 Rarely, more serious adverse effects, including cardiac arrhythmias, and anaphylactic shock, have been reported.4
Both natural and synthetic prostaglandin formulations have been used to successfully treat pyometra. Their dosages and administration frequencies vary according to the selected protocol. It is important you adhere closely to the recommended prostaglandin product dosing regimen as prostaglandins have narrow safety margins and severe adverse effects can be expected when excessive doses are given. Synthetic prostaglandin formulations, such as cloprostenol, appear to induce fewer adverse effects because of increased specificity for the uterine smooth muscle.3 In a report of 163 dogs with open-cervix pyometra treated medically with prostaglandins alone, 153 dogs responded favorably.4
Dopamine agonists
Dopamine agonists have been used in combination with prostaglandins to treat pyometra.11 Dopamine agonists act by inhibiting prolactin production by the pituitary gland. Prolactin is luteotrophic. Repeated administration of prolactin inhibitors will induce a rapid drop in plasma progesterone concentrations.12 Thus, a reduction in prolactin concentrations in the blood would be expected to have a synergistic effect with prostaglandins for promoting regression of the corpora lutea. Dopamine agonists cabergoline and bromocriptine have been administered for this purpose.3 Cabergoline is often preferred over bromocriptine because it usually has fewer adverse effects.3 In one study, the combination of cloprostenol and cabergoline was successful in treating 21 of 22 patients with open cervix pyometra.11 In another study involving both open and closed cervical cases, 24 of 29 patients were successfully treated with this combination.13
Progesterone receptor antagonists
Progesterone receptor antagonists, such as aglepristone, have also been evaluated for the treatment of pyometra.14-17 These products competitively bind to progesterone receptors in the uterus, preventing endogenous progesterone from exerting its effect. However, because progesterone-receptor antagonists do not directly stimulate the myometrium to contract and expel the uterine contents, their use as a sole therapeutic agent for treating pyometra may be limited.3 When combined with cloprostenol, aglepristone was found to be more effective for treating pyometra than aglepristone alone was.17,18 Adverse effects are uncommon in patients treated with aglepristone. Aglepristone is not available in the United States at this time.
Prognosis
The patient's stage of diestrus may impact the initial success of medical management. The corpus luteum becomes more sensitive to prostaglandins as it ages.19 During the first five weeks of diestrus, higher doses of prostaglandins or the concurrent administration of dopamine agonists may be required to achieve luteolysis. Bitches treated during the first five weeks of diestrus are more likely to require retreatment than are those that are treated after the fifth week.4
Regardless of the protocol selected, patients undergoing medical management for pyometra should be examined frequently on the days of treatment and again one and two weeks after treatment. The patient's vital signs, mental status, and hydration should be evaluated. The character of the vaginal discharge as well as the ultrasonographic status of the distended uterus should be assessed every few days along with progesterone concentrations. A successful treatment would be characterized by the resolution of vaginal discharge, normalization of physical examination findings and laboratory abnormalities, and the complete evacuation and reduction in the diameter of the uterine horns.
Abnormal laboratory findings have been reported to normalize within 14 days of successful medical and surgical management of pyometra.11,14,20 Any significant deterioration in the patient's clinical condition would warrant diagnostic reevaluation of the patient, initiation of the appropriate supportive care, and, in most cases, the recommendation that medical management be abandoned in favor of an ovariohysterectomy.
For most medical protocols, clinical improvement in the patient's signs is apparent within two to four days of initiating treatment. A treatment failure can be identified by the persistence or recurrence of clinical illness, a purulent vaginal discharge, and persistent or progressive uterine distention beyond the period of expected protocol response. Progesterone concentrations > 0.5 ng/ml are an indicator of ineffective luteolysis.21 Fluid identified within the abdomen would suggest peritonitis. Patients failing to respond to medical treatment may undergo further medical therapy using the same or a different treatment protocol or may receive an ovariohysterectomy.
Medical treatments may be repeated until they prove successful. Typically, no more than two treatment cycles are required to medically resolve pyometra in most patients.4 In 163 bitches with open-cervix pyometra receiving medical management with prostaglandins, 153 completely recovered from the infection. Of those 153 dogs, 98 recovered with one course of treatment and 55 required two courses.4 Medical treatment was discontinued in 10 dogs in this series for various reasons. An early study suggested a poor response of closed pyometra to prostaglandin therapy alone.4 However, a more recent study combining cabergoline and cloprostenol reported that three out of three dogs with closed-cervix pyometra responded favorably to this combination of drugs.11
Bitches successfully treated with medical therapy should be bred during the estrous cycle immediately after treatment.3,4 Subsequent pregnancy has been suggested to be protective against the recurrence of pyometra.4 For reproductively valuable bitches, it is also important to obtain a litter whenever possible. The subsequent reproductive success of intact bitches that have recovered from pyometra varies from 50% to 65%.22 It has been suggested that those dogs that responded most quickly to treatment were more likely to breed successfully in the future.3 It is not uncommon for patients successfully treated for pyometra to demonstrate estrus much sooner because of a shortened diestrus period.4 Bitches with shorter interestrus intervals have an increased potential for recurrence of pyometra because of inadequate time for uterine recovery (remodeling and healing of the endometrium). For this reason, estrus suppression could be considered to delay cycling and promote uterine recovery until breeding is planned.4
The prevalence of pyometra recurrence in bitches that have been successfully treated remains undetermined. Recurrence rates have been reported to vary from as high as 77% within the first 27 months after treatment to no additional risk above that of dogs that have never acquired pyometra.3,23 Because an increased risk for recurrence may be present, once the owner's reproductive goals for the dog have been achieved, the patient should undergo an ovariohysterectomy.
CONCLUSION
Pyometra is a serious and potentially life-threatening disease of the canine uterus. Patients presenting with pyometra should be stabilized, and the decision whether to pursue medical management or surgical management of the uterine disease should discussed with the dog's owner. Medical management of pyometra is best performed in patients of appropriate breeding age that are reproductively valuable and free of life-threatening illnesses, including septicemia, endotoxemia, and organ dysfunction.
Brain Lucas Hamm, DVM
Jeff Dennis, DVM, DACVIM
BluePoint Specialty & Emergency Medicine for Pets
11950 W. 110th St., Suite B
Overland Park, KS 66210
REFERENCES
1. Wheaton LG, Johnson AL, Parker AJ, et al. Results and complications of surgical treatment of pyometra; a review of 80 cases. J Am Anim Hosp Assoc 1989;25:563-568.
2. Watts JR, Wright PJ, Whithear KG. Uterine, cervical and vaginal microflora of the normal bitch throughout the reproductive cycle. J Small Anim Pract 1996;37:54-60.
3. Verstegen J, Dhaliwal G, Verstegen-Onclin K. Mucometra, cystic endometrial hyperplasia, and pyometra in the bitch: advances in treatment and assessment of future reproductive success. Theriogenology 2008;70:364-374.
4. Feldman EC, Nelson RW. Cystic endometrial hyperplasia/pyometra complex. In: Canine and feline endocrinology and reproduction. 3rd ed. St. Louis, Mo: Saunders, 2004; 852-867.
5. Fransson BA. Canine pyometra: an updated on pathogenesis and treatment. Compend Contin Educ Vet 2003;25:602-612.
6. Nett TM, McClellan MC, Niswender GD. Effects of prostaglandins on the ovine corpus luteum: blood flow, secretion of progesterone and morphology. Biol Reprod 1976;15:66-78.
7. Repasi A. Effect of prostaglandin treatment on the corpus luteum, plasma progesterone concentration and the largest follicle in the dairy cow. PhD thesis. Szent Istvan University, Budapest, 2005.
8. Rudd R, Kopcha M. Therapeutic use of prostaglandin F2 alpha. J Am Vet Med Assoc 1982;181:932-934.
9. Gabor G, Siver L, Szenci O. Intravaginal prostaglandin F2 alpha for the treatment of metritis and pyometra in the bitch. Acta Vet Hung 1999;47:103-108.
10. Lein DH. Termination of pregnancy in bitches by administration of prostaglandin F-2 alpha. J Reprod Fertil Suppl 1989; 39:231-240.
11. England GC, Freeman SL, Russo M. Treatment of spontaneous pyometra in 22 bitches with a combination of cabergoline and cloprostenol. Vet Rec 2007;160:293-296.
12. Onclin K, Silva LD, Donnay I, et al. Luteotrophic action of prolactin in dogs and the effects of a dopamine agonist, cabergoline. J Reprod Fertil Suppl 1993;47:403-409.
13. Corrada Y, Arias D, Rodriguez R, et al. Combination dopamine agonist and prostaglandin agonist treatment of cystic endometrial hyperplasia-pyometra complex in the bitch. Theriogenology 2006;66:1557-1559.
14. Jurka P, Max A, Hawrynska K, et al. Age-related pregnancy results and further examination of bitches after aglepristone treatment of pyometra. Reprod Domest Anim 2010;45:525-529.
15. Gurbulak K, Pancarci M, Ekici H, et al. Use of aglepristone and aglepristone+ intrauterine antibiotic for the treatment of pyometra in bitches. Acta Vet Hung 2005;53:249-255.
16. Trasch K, Wehrend A, Bostedt H. Follow-up examinations of bitches after conservative treatment of pyometra with the antigestagen aglepristone. J Vet Med A Physiol Pathol Clin Med 2003;50:375-379.
17. Breitkopf M, Hoffman B, Bostedt H. Treatment of pyometra (cystic endometrial hyperplasia) in bitches with an antiprogestin. J Reprod Fertil Suppl 1997;51:327-331.
18. Gobello C, Castex G, Klima L, et al. A study of two protocols combining aglepristone and cloprostenol to treat open cervix pyometra in the bitch. Theriogenology 2003;60:901-908.
19. Concannon PW. Endocrinologic control of normal canine ovarian function. Reprod Domest Anim 2009;44(Suppl 2):3-15.
20. Bartoskova A, Vitasek R, Leva L, et al. Hysterectomy leads to fast improvement of haematological and immunological parameters in bitches with pyometra. J Small Anim Pract 2007;48:564-568.
21. Nelson RW, Feldman EC, Stabenfeldt GH. Treatment of canine pyometra and endometritis with prostaglandin F2 alpha. J Am Vet Med Assoc 1982;181:899-903.
22. Smith FO. Canine pyometra. Theriogenology 2006;66:610-612.
23. Meyers-Wallen VN, Goldschmidt MH, Flickinger GL. Prostaglandin F2 alpha treatment of canine pyometra. J Am Vet Med Assoc 1986;189:1557-1561.
24. Lein DH. Prostaglandins in therapy in small animal reproduction. In: Kirk RW, ed. Current veterinary therapy IX: small animal practice. Philadelphia, Pa : W.B. Saunders Co, 1986;1233-1236.
25. Shille VM. Management of reproductive disorders in the bitch and queen. In: Kirk RW, ed. Current veterinary therapy IX: small animal practice. Philadelphia, Pa: W.B. Saunders Co, 1986;1225-1229.
26. Feldman E. The cystic endometrial hyperplasia/pyometra complex and infertility in female dogs. In: Ettinger S, Feldman E. Textbook of veterinary internal medicine: diseases of the dog and cat. 5th ed. Philadelphia, Pa: W.B. Saunders Co, 2000;1549-1565.
27. Romagnoli S. Canine pyometra: pathogenesis, therapy and clinical cases, in Proceedings. World Small Anim Vet Assoc World Cong, 2002.
28. Threfall W. Hormonal usage in canine theriogenology. in Proceedings. CVC in San Diego, 2009;485-487.
29. Metcalfe S, Vischer C. Medical treatment of pyometra and the use of aglepristone. Aus Vet Pract 2006;36:171-174.
30. Fieni, F. Clinical evaluation of the use of aglepristone, with or without cloprostenol, to treat cystic endometrial hyperplasia-pyometra complex in bitches. Theriogenology 2006;66:1550-1556.