Three-minute peripheral blood film evaluation: Preparing the film
A peripheral blood film evaluation should be part of all complete blood counts, regardless of whether hematology is performed in-house or at a reference laboratory.
A peripheral blood film evaluation should be part of all complete blood counts (CBCs), regardless of whether hematology is performed in-house or at a reference laboratory. Proper sample collection, slide preparation, and staining are essential to accurately evaluate a blood film, as is the correct use of a high-quality microscope. This article describes the steps in preparing a blood film and the equipment you'll need.
COMPONENTS OF AND INDICATIONS FOR A CBC
Important components of a CBC include evaluating the erythron (hematocrit, total red blood cell [RBC] count, hemoglobin concentration, absolute reticulocyte count, and RBC indices), the leukon (total white blood cell [WBC] count, five-part differential count including immature neutrophils), the thrombon (platelet count and platelet indices), and the total protein concentration. As mentioned earlier, always include a peripheral blood film evaluation in the CBC.
A CBC should be included in evaluations of every sick patient, every patient with vague signs of disease, and every patient receiving long-term medications. In addition, a CBC should be performed as part of every preanesthetic workup, for adult wellness and geriatric profiles, and as a recheck test for patients in which RBC, WBC, or platelet abnormalities were previously diagnosed.
COLLECTING A SAMPLE FOR THE BLOOD FILM
Artifacts must be avoided for proper hematologic interpretation. Causes of artifacts include poor blood collection techniques, inadequate sample volumes, prolonged sample storage, and delayed sample analysis.
Proper blood collection is vital to prevent erroneous results from sample clotting and cellular lysis. Obtain hematology samples from the largest blood vessel possible to minimize cellular trauma and to prevent the activation of clotting mechanisms. For accurate results, discard clotted samples and collect fresh samples. Common venipuncture sites in dogs and cats include the jugular, cephalic, and lateral and medial saphenous veins. Anticoagulants include EDTA, heparin, and citrate. EDTA is the preferred anticoagulant for blood film preparation because it preserves cellular detail better than other anticoagulants do and does not interfere with Romanowsky staining of WBCs.
Inadequate sample volume is a common cause of inaccurate hematologic results. Properly fill anticoagulated blood collection tubes to avoid falsely decreased hematocrits and cell counts and to prevent RBC shrinkage.
Hematologic samples must be analyzed as soon as possible to prevent artifacts created by exposure to anticoagulants and cell deterioration due to storage and shipment. Analyze samples within three hours or refrigerate them at 39.2 F (4 C) to avoid an artificially increased hematocrit, increased mean corpuscular volume, and decreased mean corpuscular hemoglobin concentration.1 Prepare blood films within one hour of collection to avoid morphologic artifacts. RBC crenation, neutrophil hypersegmentation, lymphocytic nuclear distortion, and general WBC degeneration including vacuolization in neutrophils may occur in aged samples. In addition, monocyte vacuolization, monocyte cytoplasmic pseudopod formation, and platelet agglutination can be encountered in stored samples.2 If you use a reference laboratory for primary hematologic analyses, we recommend submitting freshly prepared blood films along with the anticoagulated blood.
PREPARING THE BLOOD FILM
Producing high-quality blood films begins by using clean, new slides. Used slides frequently have imperfections such as scratches and other physical defects. Slides must be free of fingerprints, dust, alcohol, detergents, and debris. Using a microhematocrit tube, place a small drop (2 to 3 mm in diameter) of well-mixed EDTA blood about 1 to 1.5 cm from the end of the slide. Next, draw a spreader slide back into the blood drop at about a 30-degree angle until the spreader slide edge contacts the sample drop and capillary action disperses the sample along the edge. Then, using a smooth steady motion, push the spreader slide away from the blood drop, creating a uniform film that covers nearly the entire length of the slide (Figure 1). Changing the angle of the spreader slide will change the length and thickness of the blood film. For blood samples with low hematocrits (severe anemia), you may need to decrease the angle of the spreader slide to make a good-quality slide. In contrast, for samples with high hematocrits (severe dehydration and polycythemia due to a variety of conditions), you may need to increase the angle of the spreader slide.

1. The steps in preparing a blood film. A small drop of blood is placed near the end of a slide (top). A spreader slide is drawn back into the blood drop at a 30-degree angle (middle). Then the spreader slide is pushed away from the blood drop, creating a uniform film across the slide (bottom).
Drying is an important step in the production of good-quality blood films. Allow the blood film to thoroughly air-dry before applying stain, or use a heat block (at the low setting) or a hair dryer to hasten the drying time, thus minimizing refractile markings that can distort erythrocyte morphology. In addition, keep formalin and formalin-containing containers away from all blood and cytology smears to prevent staining artifacts such as increased cytoplasmic granularity and basophilia.
STAINING THE BLOOD FILM
Most veterinary practices use a modified Wright's stain (Romanowsky stain) for both hematology and cytology. Modified Wright's stains are available as either three- or two-solution kits. We prefer kits with three separate solutions: an alcohol fixative, an eosinophilic staining solution, and a dark-blue staining solution. Veterinary practices should have two separate Coplin stain jar sets—one for hematology and cytology samples and one for contaminated samples such as those collected for ear and fecal cytology. For optimal results, replace staining solutions regularly.
Recommended blood staining protocol includes dipping the air-dried slide five to 10 times in each solution while blotting one edge briefly in between each solution. Rinse the slide with distilled water after the final staining step, and allow the blood film to air-dry before examination. Good staining technique is critical to identifying polychromatophils on a peripheral blood film. If the staining is done improperly, many of the quick Romanowsky-type stains will not give the needed tinctorial differences between mature RBCs (orange-red) and polychromatophils (bluish-pink). Typically, poor staining with the various quick stains results in all RBCs having a bluish or muddy tint.
EVALUATING THE BLOOD FILM
The microscope
A high-quality microscope is essential for hematology. We recommend a binocular microscope with a minimum of 10×, 20×, and 100× (oil-immersion) objectives and wide-field 10× oculars. When evaluating the slide, make sure maximum light reaches the blood film. This means positioning the substage condenser as close as possible to the stage with the iris wide open. The light source should be equipped with a variable rheostat to allow maximal control of light intensity. To ensure optimal focused light for the microscopic evaluation, the microscope should be in Köhler illumination. Contact your microscope vendor, or review the microscope manual to ensure proper illumination.
The three zones
A good-quality blood film has three zones: the body (near the point of blood application), the monolayer (the zone between the body and feathered edge), and the feathered edge (the area most distant from the point of application) (Figure 2). The definition of the monolayer varies from institution to institution, but the definition used to ensure consistent semiquantification of various morphologic abnormalities is the area where about half of the RBCs are touching one another without overlapping. The monolayer is the area of the blood film where WBCs and platelet numbers are estimated and cell morphology is examined. Although the monolayer is the only zone where morphologic evaluation of individual cells is performed at oil-immersion magnification, systematic blood film evaluation includes assessing of all three zones.

Figure 2. The components of the peripheral blood film slide.
First, examine the blood film at low magnification (10× or 20×), and scan the entire slide to evaluate overall film thickness, cell distribution, and differentiation of the three different zones. Evaluate the feathered edge (Figure 3) for microfilariae, phagocytized organisms, atypical cells, and platelet clumping. Next, examine the body of the blood film (Figure 4) for rouleau formation or RBC agglutination. Then, still using low magnification, evaluate the monolayer (Figure 5), estimate the total WBC count (see the third article in this symposium), and predict the expected WBC differential count. Finally, use the oil-immersion objective (100×) to examine RBC, WBC, and platelet morphology in the monolayer.

Figure 3. Look for platelet clumps, microfilariae, and large cells in the feathered edge of the film (purple section).
Evaluate RBCs for evidence of anisocytosis, poikilocytosis, polychromasia, hemoglobin concentration, and RBC parasites. Important RBC morphologic abnormalities include spherocytes, schistocytes, acanthocytes, and leptocytes (see the second article in this symposium).
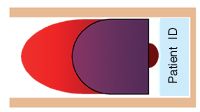
Figure 4. Look for rouleau formation and RBC agglutination in the body of the film (purple section).
Evaluate neutrophils for toxicity and the presence or absence of a left shift (increased numbers of band neutrophils). Evaluate lymphocytes for reactivity and monocytes for phagocytized organisms (see the third article in this symposium).
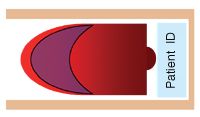
Figure 5. Estimate platelet and WBC counts and examine cell morphology in the monolayer zone (purple section).
With relatively little practice, you can identify most important morphologic abnormalities in the RBCs, WBCs, and platelets with the 20× objective field of view; these can be quickly validated with the 100× oil-immersion view.
SUMMARY
Examining a properly prepared peripheral blood film offers invaluable information about cellular morphologic changes not provided by automated instruments and provides a quality assurance confirmation of CBC data generated by in-clinic or reference laboratory hematology analyzers. We recommend taking about three minutes to view the blood film and, using the questions discussed in the next two articles of this symposium, to systematically evaluate the RBC, platelet, and WBC components of the peripheral blood film.
Fred L. Metzger Jr., DVM, DABVP (canine and feline practice)
Metzger Animal Hospital
1044 Benner Pike
State College, PA 16801
Alan Rebar, DVM, PhD, DACVP
Department of Veterinary Pathobiology
School of Veterinary Medicine
Purdue University
West Lafayette, IN 47907
ACKNOWLEDGMENT
The authors gratefully acknowledge the technical assistance and images provided by Dennis DeNicola, DVM, PhD, DACVP.
REFERENCES
1. Willard, M. et al.: The complete blood count and bone marrow examination. Textbook of Small Animal Clinical Diagnosis by Laboratory Methods, 3rd Ed. W.B. Saunders, Philadelphia, Pa., 1999; pp 11-30.
2. Rebar, A.; Metzger, F.: The Veterinary CE Advisor: Interpreting Hemograms in Cats and Dogs. Vet. Med. (suppl.) 96 (12):1-12; 2001.