A veterinary surgeons take on designing an operating room
You know the layout of these spaces is important. Heres what a boarded surgeon thinks is crucial to include.
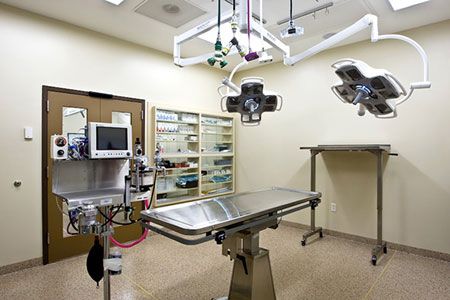
All photos courtesy of Dr. David Dycus.
Building or remodeling a veterinary hospital is a wonderful yet stressful time. There are many aspects that need attention, but one area that deserves a well-thought-out plan is the surgical suite, taking into account measures to promote asepsis while also being functional for personnel.
Surgical prep
Before we even get into the operating room (OR), there needs to be an area for surgical preparation of the patient. This is usually where the patient is anesthetized, the appropriate body part is clipped and a rough prep is completed. From here, the patient can be transferred into radiology or into the OR for surgery. The goal should be to minimize patient transport through areas that may increase chances of infection or require the patient to remain under anesthesia longer than what is necessary. Therefore, the flow needs to be designed for ease in transportation of patients between the preparation area to either the radiology suite or the OR.
“Dirty” versus “clean”
There should be defined areas for what is considered “dirty” and what is considered “clean.” Dirty areas are where nonsurgical treatments take place and street clothes can be worn. Clean areas are areas meant to minimize bacterial contamination. For an individual to be in a clean area, they should have on clean surgical scrubs, a cap, a mask and booties. Just outside of the OR, in the clean area, there should be a scrub sink where staff and doctors can appropriately scrub their hands and arms in anticipation for aseptically gowning and gloving. Once gowned and gloved, the individual must not leave the clean area but rather proceed into the OR.
The arrangement of these areas is vital, as traffic into and out of the OR should be minimized; this is the primary way that bacterial load in the environment is increased. To further minimize traffic, intercom systems, walkie-talkies and pass-through cabinets can be used. In my hospital, there are four surgery suites. Between each is a set of pass-through cabinets so that materials can be stored and team members don't have to go searching for suture or other miscellaneous items.

How many ORs and how big?
The number of operating rooms you'll need depends on your case load; however, in the event of building a new hospital, some anticipation should be given for continued growth as well as the addition of new equipment and instruments. It's also helpful to designate one OR to orthopedic procedures and another to soft tissue or “dirty” procedures where contamination may be increased such as with emergency or gastrointestinal surgeries. The square footage of the OR needs to be large enough that team members can move around with ease, and there should be space for the anesthesia team and their equipment at the head of the patient, as well as space for the operating team to perform surgery and for their surgical instruments. In human medicine, the guidelines for a primary OR are such that the room must be 400 square feet. Specialty ORs, such as for orthopedics, need to be at least 50% larger. For intermediate outpatient procedures, a guideline of 250 square feet is recommended.
I would suspect that most veterinary ORs are between 250 to 400 square feet. Hallways surrounding the OR where gurneys are used should be 8 feet wide. The floors and walls of the surgical area should be smooth and scrubbable and have no perforation. In addition, the material must be able to withstand disinfectants. Ceilings should also be cleanable, and lay-in tiles should be avoided. After each surgery, the OR should be cleaned and disinfected (mopped and surfaces wiped down). At the end of each surgical day, all ORs need a thorough cleaning.

A few more particulars
Inside the surgical suite, there should be electrical outlets placed at waist level as this will decrease the likelihood of electrical damage with fluids. All of the outlets should be of a ground-fault circuit interrupter type. In addition, at least one OR light and one outlet in each OR should be connected to an emergency electrical backup such as a generator.
Airflow is a very important consideration when designing an OR. Laminar airflow systems are costly in veterinary medicine, but they provide a significant advantage of decreasing environmental bacterial loads. When compared to conventional ventilation, laminar airflow systems revealed a 61% decrease in room bacteria and a 92% decrease in bacteria at the surgical wound. The laminar flow in a horizontal direction is preferred over vertical flow systems. The recommended HVAC guidelines are for 15 air exchanges per hour (20% should be outdoor air) with 30% to 60% humidity, and a temperature of 68 to 73 F. Doors should always remain closed to the OR, whether or not it is being used.1
After surgery, there should be an easy path to the recovery area where there should be space and cages sufficient for the number of cases seen. The recovery area should be staffed or in an area where staff are nearby in case of any postoperative complications. In addition, the recovery area should be stocked with anesthetic and emergency care equipment.
Reference
Renberg WC. Preparation of the patient, operating team, and the operating room for surgery. In: Tobias T, Johnston S, eds. Veterinary surgery: small animal. 1st ed. New York: Elsevier, 2012;164-169.
David Dycus is frequent speaker at the Fetch dvm360 conferences, an orthopedic staff surgeon at Veterinary Orthopedic & Sports Medicine Group in Annapolis Junction, Maryland, and co-founder and co-director of the Veterinary Sports Medicine & Rehabilitation Institute.