What can therapeutic drug monitoring do for you?
For starters, it can make you a veterinary detective/fortune teller/superhero who practices better medicine while making more money.

Shutterstock.comYou've of course heard the famous saying: Ask not what you can do for therapeutic drug monitoring, but what therapeutic drug monitoring can do for you. But do you really understand the widespread perks to you, your clients and your patients?
Drug monitoring is especially vital in older pets-the most likely of your patients to be receiving long-term medications, and also the most likely to have one or more conditions that warrant close monitoring. Here's a rundown of the potential benefits of drug monitoring, as outlined by Melissa Clark, DVM, PhD, DACVCP, at a recent Fetch dvm360 conference:
Make mo' money
Therapeutic drug monitoring presents an opportunity for you to practice better medicine while increasing revenue, says Fetch dvm360 speaker Karen Felsted, CPA, MS, DVM, CVPM. Here are her top tips for making the most of it:
Communicate the value. Studies show that when you take an additional moment to simply explain to your clients why you're asking them to bring their pets back to the clinic and pay you to poke them with needles again, you gain greater compliance. If you do a better job communicating to pet owners why you think something is important, they will be more likely to understand the value, says Dr. Felsted. On the contrary, if you simply say you need to see pets back for a “recheck,” pet owners won't see the purpose or value in the visit and are less likely to comply.
According to Dr. Felsted, you should try saying the following: “It's critical that we see Spot back in three weeks for a blood test so I can check the level of medication in his body. The right dose is different in every dog. If we give too little, he won't get the benefit, and if we give too much, it can have potential side effects.”
Make sure the price is right. If the cost of monitoring is a barrier to your clients, Dr. Felsted suggests examining your records to see whether or not you're getting good compliance with therapeutic drug monitoring. If you are getting pushback on your pricing or if compliance is low, one solution is to lower the price of monitoring and simply do more of it to make up the revenue. Volume is often a dirty word in veterinary medicine, but Dr. Felsted says that if you're able to get more pets monitored and make the same money (or more), why does it matter? If you monitor two phenobarbital concentrations at $55 a piece or five at $40 a piece, which approach makes you more money?
Check the AAHA Veterinary Fee Reference or Benchmarks 2015: A Study of Well-Managed Practices to see if your pricing is comparable with other practices. You should also settle on what to charge these patients coming in for blood draws. Do these visits require a doctor (and thus a full exam fee), or can you have a technician draw the blood and charge a sample collection fee?
1. It can make you a pet detective
Have you ever wondered if a patient's failure to respond to a drug is because the client isn't adhering to the medication instructions you so carefully constructed and painstakingly explained?
Therapeutic drug monitoring can help you track client compliance. If drug concentrations aren't within the expected range at steady state (after three to five half-lives), poor client compliance is one possible culprit. Unexpected subtherapeutic concentrations provide a natural opportunity for you to review with the client how and when the drug is being given, to reemphasize the importance of giving the drug consistently (e.g. “Daisy isn't getting the benefit of the drug”), and to impress the client with your uncanny detective skills!
Therapeutic drug monitoring can also help you determine the reason for poor clinical efficacy or toxicity of drugs such as phenobarbital in epileptic patients. Timing can be important, so Dr. Clark offers some case-specific pointers:
A patient with refractory seizures. Measure the trough concentration (right before the next dose is given) to see if phenobarbital concentrations are falling to subtherapeutic concentrations.
An ataxic and excessively sedated patient. Measure the peak (four to six hours after giving the medication) to see if the drug is at unacceptably high concentrations.
A patient with refractory seizures that is also ataxic and excessively sedated. Measure both the peak and the trough concentrations. If the peak is too high and the trough is too low, a veterinary clinical pharmacologist can help calculate the half-life and design a new dosing regimen. This service is available at laboratories with a clinical pharmacologist on staff (such as Auburn University), often at no additional cost!
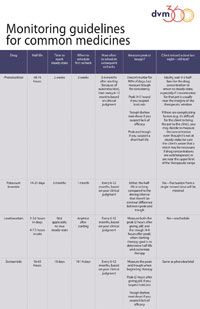
Click on the image to access a downloadable PDF of monitoring guidelines for common medicines.2. It can allow you to add “fortune teller” to your resume
Therapeutic drug monitoring lets you tell the future-really! It allows you to adjust the dose of the medication, if needed, before the animal develops clinical side effects from loss of drug efficacy or toxicosis.
In some cases, therapeutic drug monitoring lets you adjust the dose even before the drug reaches steady-state concentrations. For owners of dogs with refractory seizures that are receiving drugs such as bromide (which takes three months to reach steady-state), being able to adjust dosages sooner is a big win. Instead of having to wait three months (and risking declining drug concentrations and seizures in the meantime), you can measure the bromide concentration at the one-month mark, or after one half-life has elapsed.
If you give a loading dose of bromide and want to ensure your maintenance dose is adequate to maintain what you achieved with the load, take a blood sample within a week after finishing the load and measure the concentration. Then recheck in one month. If there is more than a 15% decrease between the load and the concentration at one month, the maintenance dose is too low.
If you didn't give a loading dose but still want to know earlier rather than later if your maintenance dose is appropriate, you can check the concentration after one half-life and use that to predict the concentration at steady state. After one half-life, bromide will be at 50% of its steady-state concentration, so you can simply take your one-month measurement and double it to estimate the steady-state concentration. If the number is below the therapeutic window, increase the maintenance dose. If the number is above, reduce it. If the number is in the window, great! Stay the course.
Therapeutic drug monitoring can also help you detect drug interactions. If your patient develops clinical signs associated with subtherapeutic drug concentrations when the dose being given hasn't changed, investigate for dietary factors, other drugs, or other illnesses that may be affecting the drug. In the case of bromide, increased sodium intake displaces bromide in body fluids, which can result in dramatically enhanced bromide excretion. Consequently, a switch to a saltier diet (or even feeding salty treats) can result in acute declines in bromide concentration and recurrence of seizures.
For other drugs such as phenobarbital that are primarily eliminated by the liver, concurrent administration of drugs that increase or reduce cytochrome P450 activity (such as chloramphenicol, a P450 inhibitor) can affect plasma drug concentrations.
What about levetiracetam? Do we really have to make clients pill their cats three times a day? The relationship between the frequency of dosing and the half-life of the drug has a big effect on how consistent the plasma concentrations will be. For example, if the half-life is longer than the dosing interval (as with phenobarbital), the drug will accumulate in the body and the peak and the trough concentrations at steady-state will be relatively close to each other. If the half-life of the drug is much shorter than the dosing interval (e.g. levetiracetam), the drug will be completely eliminated within the dosing interval. Expect big variations in the peak and the trough concentrations because the drug won't accumulate within the body.
In the case of levetiracetam, some pets eliminate the drug more slowly than others, and the longer the half-life, the more likely the drug can be given twice a day without compromising efficacy. If your goal is to determine the half-life in your patient, measure the peak two hours after giving the medication and then four to six hours later. As discussed above, a clinical pharmacologist can help to determine the half-life and adjust the dosing regimen. In many cats, the half-life of levetiracetam is seven and a half hours or longer, which allows for twice-daily administration. Additionally, an extended-release form of levetiracetam (with a longer half-life due to delayed absorption) is now available and may make life easier for working pet parents.
Last, although it doesn't fit the classical definition of therapeutic drug monitoring (which is measuring the concentration of the drug), drug monitoring can also refer to screens of organ function to monitor for potential adverse effects. For example, idiosyncratic hepatotoxicosis has been associated with carprofen in dogs, and in most cases, it occurs within five to 30 days of starting the drug.1 Consequently, a frequent recommendation is to perform a serum chemistry profile before starting carprofen and to repeat the test two to three weeks later to detect toxicosis before the pet is clinically ill.
3. It can make you a superhero in the eyes of your clients
According to the 2012 Veterinary Information Gap study, 60% of clients have concerns about the cost of drugs. But generics still get a bum rap because veterinarians have doubts about efficacy and safety.
Therapeutic drug monitoring can help you sleep at night when prescribing generics. Face it-many of our clients are already shopping online for better drug prices instead of buying what's stocked on your practice's shelves, so offering generics is a way to build goodwill. This simple gesture shows your client that you care about what they care about and builds trust and customer loyalty. And, in all likelihood, it will increase compliance for follow-up monitoring.
If you are switching from a brand name to a generic, Dr. Clark recommends measuring the peak or trough concentration (depending on whether lack of efficacy, toxicity or both is the major concern) when the drug concentrations are expected to be at steady-state (usually after about three to five half-lives). This helps to determine whether absorption of the generic is appropriate and can be used to predict safety and efficacy. Earlier measurements can also be made, as discussed above for bromide.
4. It can give you a reason to use your ninth grade math skills
If you are like me, you (happily) thought you would never use algebra again. However, Dr. Clark says a simple algebraic equation can help you calculate the expected drug concentration in your patient every time you start a drug or change the dose.
Most drugs used in veterinary medicine have linear pharmacokinetics, so drug dosage and plasma drug concentration should vary in a proportional manner. Therefore:
I
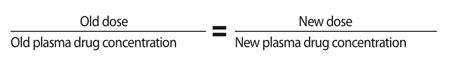
f you want a higher plasma drug concentration, you can calculate the new dose using the equation above. For example, let's say you're giving 2 mg/kg of phenobarbital twice a day (old dose), and you measure a drug concentration of 15 µg/ml (old concentration). If you want the new concentration to be 25 µg/ml, plugging in the numbers to the above equation gives us a new dose of 3.3 mg/kg.
Alternatively, when the plasma drug concentration is measured after a dose change, the new expected concentration can be calculated and compared with the actual results. For example, say you decide to increase the dose to 4.5 mg/kg twice a day. Using the equation, you can determine that the new concentration is 34 µg/ml. A large discrepancy may hint at owner compliance difficulties or changes in drug absorption or elimination-all issues you can investigate and remedy using your newfound knowledge.
If you suspect a lack of efficacy and measure subtherapeutic plasma drug concentrations, you can either increase the dose by 25% or adjust the dose based on what you calculate the target plasma concentration to be.
Reference
1. MacPhail CM, Lappin MR, Meyer DJ, et al. Hepatocellular toxicosis associated with administration of carprofen in 21 dogs. J Am Vet Med Assoc 1998;212:1895–1901.