Canine pulmonary hypertension, Part 1: An in-depth review of its pathophysiology and classifications
Understanding this syndrome's pathophysiology and classification schemes will help you better manage affected patients.
Although previously thought to be uncommon, canine pulmonary hypertension is now diagnosed with relative frequency.1 Understanding the pathophysiology of pulmonary hypertension is paramount to successful treatment. Canine pulmonary hypertension should also be recognized as a complex syndrome that is often associated with severe underlying systemic disease.
In this article, we review the anatomy of the pulmonary vascular system and discuss the regulation of pulmonary arterial pressure. We also describe the clinical and functional classifications of pulmonary hypertension.
DEFINITION
Any elevation of pulmonary arterial pressure above normal constitutes pulmonary hypertension.2 More specifically, pulmonary hypertension can be defined as pulmonary arterial systolic pressure > 30 mm Hg, pulmonary arterial diastolic pressure > 15 mm Hg, or pulmonary arterial mean pressure > 20 mm Hg.3 Although it is possible to obtain these measurements directly through right-sided cardiac catheterization, this procedure typically requires heavy sedation or anesthesia, is considered high risk in unstable patients, and can be costly.4 Alternatively, pulmonary arterial pressures can be assessed by transthoracic echocardiography, which includes subjective assessment of cardiac changes and Doppler analysis of tricuspid valve regurgitation and pulmonary valve insufficiency.
Pulmonary arterial pressure depends on several factors, including right ventricular cardiac output (or pulmonary blood flow), pulmonary vascular resistance, and pulmonary venous pressure.3 An increase in blood flow to the pulmonary arteries, such as in congenital shunts, leads to increased pulmonary arterial pressure. Augmented activity of vascular smooth muscle, increased blood viscosity, and the presence of vascular obstruction all result in increased pulmonary vascular resistance and, thus, increased pulmonary arterial pressure. Pulmonary venous pressure, which becomes elevated in advanced left-sided heart disease, also contributes to increased pulmonary arterial pressure. Based on the variety of factors that contribute to and control pulmonary arterial pressure, it is clear that pulmonary hypertension may develop as the result of many underlying diseases.
PULMONARY VASCULAR ANATOMY
The pulmonary vascular system is characterized as low pressure, low resistance, and high capacitance.5 Normal pulmonary arteries are elastic with distensible walls. They are composed of an inner tunica intima, middle tunica media, and outer tunica adventitia (Figure 1). The tunica intima consists of a single layer of endothelial cells, collagen, and occasional fibroblasts. The tunica media is thicker and is a combined layer consisting of elastin, collagen, and smooth muscle fibers. The tunica adventitia consists of collagen.6
Several characteristic histopathologic lesions are associated with pulmonary hypertension. These most often include concentric thickening and muscularization of the tunica intima and hypertrophy with fibrosis and proliferation of smooth muscle of the tunica media (Figure 2). In severe cases, plexiform lesions (irregularly shaped outgrowths that project from the intimal layer into the lumen of the blood vessel) may develop, and vessel wall necrosis can occur.7
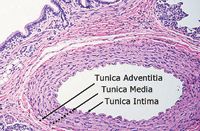
1. A photograph of a cross section of a normal canine pulmonary artery. The tunica adventitia, media, and intima layers are all normal in thickness and cell structure (hematoxylin-eosin stain; 10X magnification). (Image courtesy of Pam Mouser, DVM, MS, DACVP, Angell Animal Medical Centerâs Department of Pathology.)
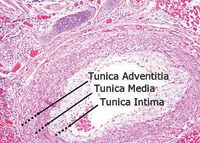
2. A photograph of a cross section of a canine pulmonary artery in a patient with documented pulmonary hypertension. The tunica adventitia and intima layers are both thickened, supporting the clinical diagnosis of pulmonary hypertension (hematoxylin-eosin stain; 10X magnification). (Image courtesy of Pam Mouser, DVM, MS, DACVP, Angell Animal Medical Centerâs Department of Pathology.)
PATHOPHYSIOLOGY OF PULMONARY HYPERTENSION
Pulmonary hypertension develops when there is an imbalance among the factors that control pulmonary arterial vasoconstriction, vasodilation, platelet activation, and smooth muscle cell proliferation (Table 1).3 By understanding these factors, practitioners are better able to choose the therapy or combination of medications that is most likely to help reduce pulmonary arterial pressure. For instance, by understanding the roles that prostaglandins, endothelin, and nitric oxide play in pulmonary vessel constriction and dilation, you can choose the best therapy for your patient.
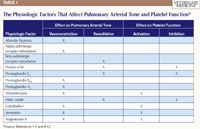

Table 1: The Physiologic Factors That Affect Pulmonary Arterial Tone and Platelet Function*
Alveolar hypoxia
Alveolar hypoxia elicits pulmonary vessel vasoconstriction, a response unique to the pulmonary system. Vasoconstriction allows deoxygenated blood to be shunted to areas of the lung that are better ventilated and improves ventilation-perfusion matching, which is thought to be a beneficial physiologic response in acute instances but, in chronic conditions, may lead to pulmonary hypertension.
Pulmonary vasculature tone is controlled by potassium, calcium, and chloride channels. The activity of these channels is affected by local oxygen tension. Poor oxygen tension, or hypoxia, leads to vasoconstriction mainly in small pulmonary arteries and arterioles, leading to increased pulmonary vascular resistance.2 If oxygen tension remains poor over a long period, pulmonary vasoconstriction results in increased pulmonary arterial pressure and pulmonary hypertension.
Alveolar hypoxia also induces growth factors, such as platelet-derived growth factors A and B, vascular endothelial growth factor, endothelin, and serotonin. These factors are associated with endothelial cell proliferation and vascular remodeling, as seen in Figure 2.2
Adrenergic control
Pulmonary arterial vasoconstriction occurs in response to the stimulation of alpha-adrenergic receptors. Alpha-adrenergic receptors found in the pulmonary arteries have a high affinity for their agonists, such as norepinephrine, and, when excessively stimulated, may also cause pulmonary arterial remodeling.2 Pulmonary arterial vasodilation occurs in response to the stimulation of beta-adrenergic receptors.
Eicosanoids: prostaglandins and thromboxane
Prostaglandins are hormone-like substances that are actively synthesized, metabolized, and released by the lungs. Prostacyclin and prostaglandin E1 cause vasodilation and vascular hypertrophy and remodeling and inhibit platelet aggregation. On the other hand, prostaglandin F2α and prostaglandin A2 cause vasoconstriction.2,8
Thromboxane, a substance derived from prostaglandins, is synthesized by and stored in platelets. Thromboxane is associated with vasoconstriction and platelet activation. In people with pulmonary hypertension, there is a documented prostacyclin-thromboxane imbalance with associated pulmonary artery vasoconstriction, thrombosis, and proliferation.9
Nitric oxide
Nitric oxide is synthesized in endothelial cells from L-arginine and oxygen by the enzyme nitric oxide synthase. Once produced, nitric oxide is released by the vascular endothelium and travels to smooth muscle cells. There, nitric oxide stimulates the enzyme guanylate cyclase, which catalyzes guanosine triphosphate conversion to cyclic guanosine monophosphate (cGMP), leading to an increase in cGMP concentrations. cGMP inhibits calcium release from the endoplasmic reticulum and causes pulmonary vasodilation (Figure 3). Vasodilation is limited by phosphodiesterase 5 inactivation of cGMP.1 Nitric oxide also inhibits platelet activation and smooth muscle cell hypertrophy.10
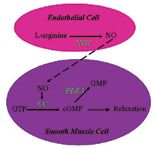
3. A schematic demonstrating the actions of nitric oxide in pulmonary vascular endothelial and smooth muscle cells (NO = nitric oxide; NOS = nitric oxide synthase; GTP = guanosine triphosphate; GC = guanylate cyclase; cGMP = cyclic guanosine monophosphate; PDE5 = phosphodiesterase 5; GMP = guanosine monophosphate).
Endothelin-1
Endothelin-1 is a peptide released by the vascular endothelium in response to changes in blood flow, vascular stretch, oxygenation, and thrombin concentrations. Once released, endothelin-1 causes vasoconstriction, stimulates growth factors and smooth muscle cell proliferation, and promotes vascular remodeling.8 Production of endothelin-1 is inhibited by prostacyclin and nitric oxide.2
Endothelin-1 is considered a potent vasoconstrictor and has been well-studied in human medicine. Circulating endothelin-1 concentrations are elevated in people with pulmonary hypertension, and there is a correlation between endothelin-1 concentrations and the severity of pulmonary hypertension and the prognosis for people with pulmonary hypertension.11 Veterinary studies have also confirmed that endothelin-1 concentrations are elevated in dogs with pulmonary hypertension.12
Serotonin
Serotonin is produced by the gastrointestinal tract from tryptophan.5 Once produced, serotonin is released into circulation and taken up by platelets. Platelets then release serotonin in response to blood vessel wall damage so that serotonin causes local vasoconstriction. As mentioned above, serotonin can act as a growth factor and also causes smooth muscle cell hypertrophy and vascular remodeling.8
Angiotensin II
Angiotensin II is a peptide produced by the actions of the angiotensin-converting enzyme (ACE) on angiotensin I. In animal models of pulmonary hypertension, pulmonary hypertension is associated with an increase in ACE expression and activity.2 Angiotensin II causes vasoconstriction and vascular remodeling.2
CLINICAL CLASSIFICATION
The Evian Classification Scheme, proposed by the World Health Organization (WHO), categorizes pulmonary hypertension based on similarities in pathophysiologic mechanism, clinical presentation, and treatment options.13,14 This scheme has been adopted by the veterinary community.
Clinical class I: pulmonary arterial hypertension
Class I pulmonary hypertension includes patients with pulmonary hypertension due to pulmonary arteriolar vascular disease. In people, the most common form of class I pulmonary hypertension is idiopathic. Although idiopathic pulmonary hypertension has been recognized in dogs, it is rarely reported.15 In dogs, the most common causes of class I pulmonary hypertension include congenital shunts and heartworm disease.15
Congenital shunts. Congenital shunts include patent ductus arteriosus, atrial septal defects, and ventricular septal defects. These defects all lead to increased pulmonary blood flow and structural changes in the vascular walls. Specifically, histopathology demonstrates hypertrophy of the small muscular pulmonary arteries and arterioles. Advanced disease is associated with fibrosis, vessel obliteration, and arteritis.16
Eisenmenger syndrome describes severe pulmonary arterial hypertension secondary to a congenital cardiac defect. In this condition, a left-to-right cardiac shunt causes severe endothelial dysfunction, which leads to increased pulmonary vascular resistance. This resistance ultimately increases right-sided heart pressures to the point of shunt reversal, and blood flows right to left through the congenital defect. Patients with Eisenmenger syndrome develop severe cyanosis, polycythemia, and congestive heart failure. In human medicine, the development of Eisenmenger syndrome secondary to an unrepaired congenital shunt is associated with a 10- to 12-fold increase in mortality; almost all patients with unrepaired patent ductus arteriosus develop Eisenmenger syndrome.17
Heartworm disease. Heartworm disease, caused by the nematode Dirofilaria immitis, is another common cause of canine class I pulmonary hypertension. Heartworm disease is diagnosed worldwide and occurs when a mosquito bite transmits D. immitis larvae to a canine host. Over a period of months, the larvae develop into adult nematodes and relocate to the right side of the heart and the pulmonary artery. Acute signs of pulmonary hypertension can be caused by an embolism of dead adult heartworms and are associated with class IV pulmonary hypertension (see below). But long-term, occlusion of large pulmonary arteries leads to pulmonary vascular proliferation, irreversible structural damage, inflammation, and vascular dysfunction that is typical of class I pulmonary hypertension.18 French heartworm, caused by Angiostrongylus vasorum, has also been associated with canine pulmonary hypertension.19
Clinical class II: pulmonary venous hypertension
Patients in the class II category develop pulmonary hypertension secondary to left-sided heart disease. Chronic left-sided heart disease leads to increased left atrial pressure, which in turn leads to increased pulmonary venous pressure. In these scenarios, pulmonary edema and hypoxia develop, and reactive pulmonary arterial hypertension occurs.3 When pulmonary venous pressure exceeds 25 mm Hg, pulmonary arterial pressure increases in an attempt to maintain pulmonary blood flow. Ultimately, pulmonary arteriole hypertrophy and pulmonary artery noncompliance develop.
Left-sided heart disease is the most common cause of pulmonary hypertension overall in both people and dogs.13,15 While causes of left-sided heart disease may include dilated cardiomyopathy, degenerative mitral valve disease is a more common cause of canine pulmonary hypertension. In a study of 60 dogs with pulmonary hypertension, 38 dogs (63%) had pulmonary hypertension due to degenerative mitral valve disease, while only two dogs (3%) had pulmonary hypertension due to dilated cardiomyopathy.20 Other studies indicate that anywhere from 14% to 31% of dogs with degenerative mitral valve disease develop pulmonary hypertension.21,22 Although less common, class II pulmonary hypertension has been reported in people and dogs with myocarditis and atrial distention secondary to atrial fibrillation.8,23
Clinical class III: pulmonary disease or hypoxia
Pulmonary hypertension may also occur secondary to primary pulmonary disease or chronic hypoxia. These patients are considered class III. The respiratory diseases most frequently associated with class III pulmonary hypertension in people are chronic obstructive airway disease, interstitial lung disease, and sleep-disorder breathing.8 In dogs, class III pulmonary hypertension has been associated with pulmonary fibrosis, pneumonia, tracheobronchial disease, and neoplasia.22 Given the breed predilection, it is not surprising to find that up to 40% of West Highland white terriers with chronic interstitial lung disease have some degree of pulmonary hypertension.24
Clinical class IV: thromboembolic disease
Class IV pulmonary hypertension is caused by a thrombotic or embolic event. In people with class IV pulmonary hypertension, pulmonary artery obstruction has been associated with thromboembolism, tumors, and foreign bodies. In dogs, pulmonary thromboembolism has been associated with immune-mediated hemolytic anemia, neoplasia, protein-losing nephropathies and enteropathies, hyperadrenocorticism, sepsis, and trauma.15,23 Given the possibility of worm emboli, heartworm disease can be included in this category as well.15
Clinical class V: miscellaneous
Class V pulmonary hypertension encompasses the miscellaneous causes of pulmonary hypertension. In people, class V includes conditions that indirectly alter cardiac blood flow (e.g. primary polycythemia vera), granulomatous diseases, and diseases that lead to the destruction of pulmonary parenchyma.13 In veterinary medicine, class V pulmonary hypertension is rarely reported; however, the most common conditions are likely those that cause pulmonary vasculature compression, such as neoplasia.
FUNCTIONAL CLASSIFICATION
While the clinical classification scheme groups pulmonary hypertension patients into classes based on the underlying cause of pulmonary hypertension, the functional classification scheme groups these patients into classes based on the severity of pulmonary hypertension-induced clinical signs (Table 2). This schematic was also developed at the 1998 WHO Evian meeting and is used in human medicine to help determine when to institute therapy, to decide which treatments may be most beneficial, and to provide an objective treatment goal.25 Although not explicitly evaluated in dogs, the information can be easily extrapolated from people to dogs.
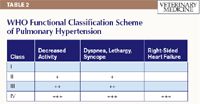
Table 2: WHO Functional Classification Scheme of Pulmonary Hypertension
Functional class I
This class includes patients with pulmonary hypertension that do not suffer any decrease in physical activity and can exercise without signs of dyspnea, fatigue, chest pain, or syncope.
Functional class II
Class II patients are comfortable at rest but suffer a mild decrease in activity associated with dyspnea, fatigue, chest pain, or syncope.
Functional class III
These patients have pulmonary hypertension that results in marked limitations in physical activity and have severe dyspnea, fatigue, chest pain, or syncope even with minimal activity. These patients are comfortable at rest.
Functional class IV
The final class includes patients with pulmonary hypertension that are unable to participate in physical activity, and any activity leads to severe signs. These patients are symptomatic at rest and have right-sided heart failure secondary to pulmonary hypertension.
CONCLUSION
Canine pulmonary hypertension is a complex condition caused by an imbalance in pulmonary arterial vasoconstriction and vasodilation and is associated with enhanced platelet actions and vascular remodeling. Patients with pulmonary hypertension may be classified into clinical groups based on the underlying cause of disease and into functional groups based on the severity of signs. Ultimately, the classification schemes should help practitioners diagnose pulmonary hypertension, formulate an effective treatment plan, and evaluate a patient's prognosis.
Rebecca L. Quinn, DVM, DACVIM (internal medicine)
Department of Cardiology
Angell Animal Medical Center
350 S. Huntington Ave.,
Boston, MA 02130
Justin G. Williams, DVM, DACVIM (cardiology)
VCA Animal Care Center of Sonoma County
6470 Redwood Drive
Rohnert Park, CA 94928
REFERENCES
1. Henick R. Pulmonary hypertension: more than Viagra, in Proceedings. Int Vet Emer Crit Care Symp, 2007.
2. Bonow RO, Mann DL, Zipes DP, et al. Braunwald's heart disease: a textbook of cardiovascular medicine. Philadelphia, Pa: W.B. Saunders. Retrieved January 18, 2011 from http://expertconsultbook.com.
3. Stepien RL. Pulmonary arterial hypertension secondary to chronic left-sided cardiac dysfunction in dogs. J Small Anim Pract 2009;50(Suppl 1):34-43.
4. Mercier E, Mathieu M, Sandersen CF, et al. Evaluation of the influence of age on pulmonary arterial pressure by use of right ventricular catheterization, pulsed-wave Doppler echocardiography, and pulsed-wave tissue Doppler imaging in healthy Beagles. Am J Vet Res 2010;71(8):891-897.
5. Guyton AC, Hall JE. Textbook of medical physiology. 11th ed. Philadelphia, Pa: Elsevier Inc, 2006;161-179.
6. Young B, Heath JW. Wheater's functional histology. 4th ed. Edinburgh: Harcourt Publishers Limited, 2001;144-155.
7. Tuder RM, Abman SH, Braun T, et al. Development and pathology of pulmonary hypertension. J Am Coll Cardiol 2009;54(Suppl 1):S3-S9.
8. McLaughlin VV, Archer SL, Badesch DB, et al. ACCF/AHA 2009 expert consensus document on pulmonary hypertension a report of the American College of Cardiology Foundation Task Force on Expert Consensus Documents and the American Heart Association developed in collaboration with the American College of Chest Physicians; American Thoracic Society, Inc.; and the Pulmonary Hypertension Association. J Am Coll Cardiol 2009;53(17):1573-1619.
9. Christman BW, McPherson CD, Newman JH, et al. An imbalance between the excretion of thromboxane and prostacyclin metabolites in pulmonary hypertension. N Engl J Med 1992;327:70-75.
10. Ichinose F, Roberts JD Jr, Zapol WM. Inhaled nitric oxide: a selective pulmonary vasodilator: current uses and therapeutic potential. Circulation 2004;109(25):3106-3111.
11. Rubens C, Ewert R, Halank M, et al. Big endothelin-1 and endothelin-1 plasma levels are correlated with the severity of primary pulmonary hypertension. Chest 2001;120(5):1562-1569.
12. Uchide T, Saida K. Elevated endothelin-1 expression in dogs with heartworm disease. J Vet Med Sci 2005;67(11):1155-1161.
13. Simonneau G, Robbins IM, Beghetti M, et al. Updated clinical classification of pulmonary hypertension. J Am Coll Cardiol 2009;54(Suppl 1):S43-S54.
14. Simonneau G, Galie N, Rubin LJ, et al. Clinical classification of pulmonary hypertension. J Am Coll Cardiol 2004;43(12 Suppl S):S5-S12.
15. Kellihan HB, Stepien RL. Pulmonary hypertension in dogs: diagnosis and therapy. Vet Clin North Am Small Anim Pract 2010;40(4):623-641.
16. Vongpatanasin W, Brickner ME, Hillis LD, et al. The Eisenmenger syndrome in adults. Ann Intern Med 1998;128(9):745-755.
17. Beghetti M, Galie N. Eisenmenger syndrome: a clinical perspective in a new therapeutic era of pulmonary hypertension. J Am Coll Cardiol 2009;53(9):733-740.
18. Hirano Y, Kitagawa H, Sasaki Y. Relationship between pulmonary arterial pressure and pulmonary thromboembolism associated with dead worms in canine heartworm disease. J Vet Med Sci 1992;54(5):897-904.
19. Nicolle AP, Chetboul V, Tessier-Vetzel D, et al. Severe pulmonary arterial hypertension due to Angiostrongylosus vasorum in a dog. Can Vet J 2006;47(8):792-795.
20. Serres F, Chetboul V, Gouni V, et al. Diagnostic value of echo-Doppler and tissue Doppler imaging in dogs with pulmonary arterial hypertension. J Vet Intern Med 2007;21(6):1280-1289.
21. Serres FJ, Chetboul V, Tissier R, et al. Doppler echocardiography-derived evidence of pulmonary arterial hypertension in dogs with degenerative mitral valve disease: 86 cases (2001-2005). J Am Vet Med Assoc 2006;229(11):1772-1778.
22. Borgarelli M, Zini E, D'Agnolo G, et al. Comparison of primary mitral valve disease in German shepherd dogs and in small breeds. J Vet Cardiol 2004;6(2):27-34.
23. Johnson L, Boon J, Orton EC. Clinical characteristics of 53 dogs with Doppler-derived evidence of pulmonary hypertension: 1992-1996. J Vet Intern Med 1999;13(5):440-447.
24. Schober KE, Baade H. Doppler echocardiographic prediction of pulmonary hypertension in West Highland white terriers with chronic pulmonary disease. J Vet Intern Med 2006;20(4):912-920.
25. Rubin LJ, American College of Chest Physicians. Diagnosis and management of pulmonary arterial hypertension: ACCP evidence-based clinical practice guidelines. Chest 2004;126(Suppl 1);S7-S10.
Podcast CE: Canine cardiology: the practical guide to the mitral valve patient
July 19th 2023Learn about the prevalence of myxomatous mitral valve disease, guidelines for staging heart disease, proactive diagnostic workup, the importance of spironolactone and aldosterone blocking, and the benefits of combination therapy for improved outcomes in canine patients
Listen