Clinical Exposures: Hemophilia A in a Maltese dog
An approximately 1-year-old male Maltese dog was presented to the Veterinary Clinic of East Hampton for a routine castration.
An approximately 1-year-old male Maltese dog was presented to the Veterinary Clinic of East Hampton for a routine castration. The dog had been adopted from a shelter three months before and had an unknown medical history. Physical examination findings and the results of a preanesthetic complete blood count and serum chemistry profile revealed no abnormalities. A routine open orchiectomy was performed, and the surgery was uneventful.
POSTOPERATIVE FINDINGS
An hour after surgery, severe bleeding from the incision site and into the scrotum was noted (Figure 1). Attempts to stop the bleeding with ice and pressure bandages were unsuccessful. The differential diagnoses included ligature failure, bleeding disorders (e.g. von Willebrand's disease, hemophilia A [factor VIII deficiency], hemophilia B [factor IX deficiency]), and rodenticide toxicosis. Because the bleeding was delayed, severe, and uncontrolled, thrombocytopathia (e.g. due to a tick-borne disease or toxicosis from an antiplatelet drug such as clopidogrel) was considered unlikely.
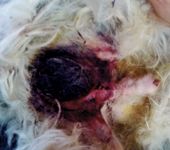
Figure 1. A scrotal hematoma and inguinal bruising in a 1-year-old dog one hour after routine orchiectomy.
A prothrombin time (PT) was measured, and the result was normal (7.7 seconds; reference range = 6 to 12 seconds). The result of a partial thromboplastin time (PTT) was 49.2 seconds (reference range = 10 to 25 seconds), so a problem with the intrinsic hemostatic pathway was suspected, such as a coagulation factor deficiency. The dog was given 6 ml/kg of fresh frozen plasma, and the bleeding stopped.
Rodenticide toxicosis was ruled out because of the normal PT and the lack of exposure to rodenticides, according to the owner. The results of a tick-borne and heartworm disease screening test (SNAP 4Dx—Idexx) were negative. The packed cell volume and total solids results were normal before discharge. Twenty-four hours later, the dog was discharged, and the owner was instructed to keep the dog strictly confined for 14 days.
DIAGNOSIS AND FOLLOW-UP
The dog was reexamined 14 days after the surgery, and the scrotal hematoma had resorbed. Blood samples to measure von Willebrand factor and factors VIII and IX activities were sent to Cornell University's Animal Health Diagnostic Center via Antech Diagnostics. The von Willebrand factor and factor IX activities were normal, and factor VIII activity was 1.5 % (reference range = 50% to 200%), so hemophilia A was diagnosed.
The owner was instructed to change the dog's lifestyle to a quieter one and to seek medical help in any case of trauma or bruising. The dog was seen two months later for its annual examination and was doing well.
DISCUSSION
Hemophilia A is the most common inherited coagulation factor deficiency in dogs1,2 and is one of the primary rule- outs for abnormal bleeding in young male dogs and in cats.3 In dogs, von Willebrand's disease is the most common inherited bleeding disorder and is one of the primary rule-outs as well. Factor VIII deficiency, or hemophilia A, is an X-linked recessive disease, so clinical bleeding is seen almost exclusively in young males, while affected females are usually asymptomatic heterozygous carriers.1,2 It is more common in purebred dogs, with a higher prevalence in German shepherds.1,3 Once this disorder is diagnosed in a puppy, it means that the dam is heterozygous and should not be used for breeding. Affected dogs should also never be bred.
Factor VIII is a cofactor that has an important role in the intrinsic pathway of the coagulation cascade. Factor VIII deficiency leads to insufficient fibrin formation, so the primary platelet plug is washed away once vasoconstriction diminishes and the vessel is reperfused. Thus, factor VIII deficiency results in delayed and often uncontrolled bleeding.2
Common clinical signs of hemophilia A and other secondary hemostatic disorders (coagulation factor abnormalities, except von Willebrand factor deficiency) include hematoma formation, bleeding into body cavities and joints (hemarthrosis), and prolonged bleeding after surgery or trauma.4 Clinical signs of primary hemostatic disorders (platelet or vascular abnormalities and von Willebrand's disease) include petechiae, ecchymoses, hyphema, epistaxis, oral bleeding, melena, and hematochezia. In puppies with hemophilia A, prolonged bleeding from the umbilical vessels may occur after birth (which can be fatal) and from the gingiva in association with erupting teeth.1 Bleeding episodes are more frequent and severe in individuals suffering from a greater degree of factor deficiency (patients with a lower in vitro residual factor VIII coagulant activity).4
Since factor VIII is involved in the intrinsic coagulation pathway, activated clotting time (ACT) and PTT are usually prolonged, while PT is normal.1 Hemophilia A is definitively diagnosed by measuring the factor VIII activity. The factor activity in affected animals varies between 0% to 25%, and the disease is classified as mild (> 5% factor activity), moderate (1% to 5% factor activity), and severe (< 1% factor activity).1 It is not easy to detect carrier females since their factor VIII activities are usually normal.5
Treating bleeding episodes requires repeated transfusions of fresh whole blood, fresh plasma, or fresh frozen plasma concentrates until bleeding has been controlled. It is better to use plasma instead of whole blood because of the possible sensitization of the animal to red blood cell antigens. Whole blood transfusions are better reserved for patients with life-threatening anemia.1
REFERENCES
1. Carr PA, Nibblett BM, Panciera DL. Von Willebrand's disease and other hereditary coagulopathies. In: Bonagura DJ, Twedt DC, eds. Kirk's current veterinary therapy XIV. St. Louis, Mo: Saunders, 2009;277-280.
2. Thompson MS, Kreeger JM. Acute paraplegia in a puppy with hemophilia A. J Am Anim Hosp Assoc 1999;35(1):36-37.
3. Brooks MB. Hemophilias and other hereditary coagulation factor deficiencies. In: Coté E, ed. Clinical veterinary advisor: dogs and cats. St. Louis, Mo: Mosby Elsevier, 2007;482-483.
4. Brooks MB, MacNguyen R, Hall R, et al. Indirect carrier detection of canine haemophilia A using factor VIII microsatellite markers. Anim Genet 2008;39(3):278-283.
5. Mackin A. Bleeding disorders. http://www.vin.com/Members/SearchDB/misc/m05000/m02102.htm; 2002. Accessed Oct. 15, 2009.