Dont let ringworm run rings around your veterinary patients
Are you caught up on the latest veterinary developments for managing ringworm? (Hint: Theres a new diagnostic test and new drug at your dermatophytosis-demolishing disposal.)

Typical ringworm lesion on the face of a cat. (All images courtesy of Dr. Anthea Schick)Dermatophytosis, or ringworm, is a fungal infection caused by protein-eating fungi that invade the hair shaft and the surface of the skin. There are many species of ringworm, but the fungi you are most likely to encounter are Microsporum canis in cats and Microsporum gypseum and Trichophyton species in dogs.
Predisposing factors
Ringworm is much more common in cats than in dogs, and Persian cats appear to be predisposed. Dogs with ringworm likely became infected through digging. Boston terriers, Yorkshire terriers and Jack Russell terriers are all prone to ringworm.
Both young and old patients are predisposed to ringworm, as are immunosuppressed patients and those with allergies.
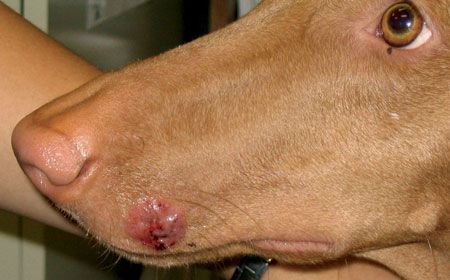
This ringworm lesion on the muzzle of a young dog is typical of a fungal kerion, which is ringworm with an exuberant inflammatory response, resembling an abscess.
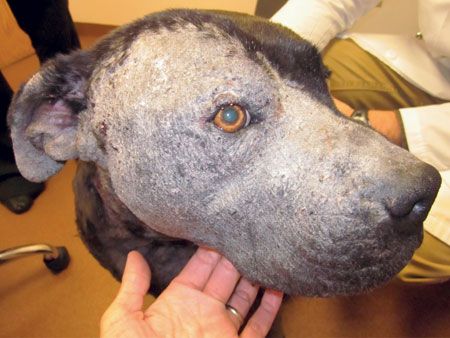
A pit bull with generalized dermatophytosis. Note the border between affected and normal skin.Clinical signs
Dermatophytosis has come to be called ringworm because of the characteristic circular area of hair loss with a red, raised outer rim. These lesions result from an inflammatory reaction to the fungus. The face, ears, feet and tail are the most commonly affected areas. Ringworm can be more extensive, causing well-demarcated alopecia, erythema, pruritus and scale. In dogs, there is often a clearly defined border of affected versus nonaffected skin. Cats, especially longhaired breeds, have a more generalized form of infection than dogs. These animals can be chronic carriers of a fungus even though they may not show any signs of infection themselves.
Diagnosis
A fungal culture (using a dermatophyte test medium [DTM]) or fungal polymerase chain reaction (PCR) test is needed to determine the species of ringworm that is infecting your patient. However, a Wood's lamp examination or direct examination of hairs can help you identify and manage ringworm cases.

A cat infected with M. canis demonstrating the fluorescence of individual hairs under the Wood's lamp.Wood's lamp
In patients with a known M. canis infection-or ones in which an M. canis infection is likely-you can use a Wood's lamp examination to help identify which hairs to sample for a culture or PCR test or to examine under the microscope. M. canis fluorescence is bright apple green, and infected hairs glow from the bulb to the tip. Not all ringworm species will fluoresce, so negative fluorescence doesn't rule out dermatophytosis.
A Wood's lamp examination can also help you monitor the patient's response to treatment. If a patient is receiving antifungal therapy, there should be fewer Wood's lamp-positive hairs, and the location of fluorescence should progress from the base of the hair to the tip as the hair grows out.

Oil immersion magnification of a ringworm-infected hair. Note the irregular appearance of the hair cuticle caused by hyphae and microconidia.Direct examination
For direct examination, place hairs plucked from near an affected area (or Wood's lamp-positive hairs) in mineral oil, cover with a cover slip and examine under 10x magnification. Infected hairs may have fungal hyphae within the hair shaft or small, round microconidia on the outside of the infected hair. You can make a tape prep of a suspicious area and stain it with either lactophenol cotton blue or the purple modified Wright's stain (Diff-Quik-Dade Behring).
Ringworm spores will appear round or ovoid and look a bit like nonbudding Malassezia species. They also often look like they have clear capsules around them.
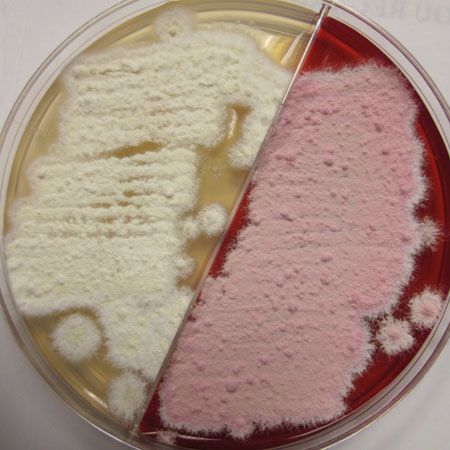
Sab-Duet from Hardy Diagnostics showing positive growth for M. canis.Culturing
To grow ringworm species in a DTM, grasp individual, grossly abnormal hairs (or Wood's lamp-positive hairs) in the direction of growth and tug gently, trying to get the root bulb. Then gently press the hair into the DTM.
You can also use the Mackenzie brush technique, in which you rub a new toothbrush or clean gauze over the entire affected site until hair is clearly visible in the brush bristles or on the gauze surface. Be sure to sample near the eyes, in the ears and between the toes. Then gently stab the bristles or press the gauze over the entire surface of the culture plate.
Ideally, incubation temperature should remain between 75 F (23.9 C) and 80 F (26.7 C), and you should check the plates daily for fungal culture growth.
Ringworm growth will appear white or buff-colored (never dark) and will develop a red color around it as it grows. Most ringworm species will grow and sporulate within seven to 10 days, but Trichophyton species cultures often take up to 21 days. Plates should be kept for at least 14 days, but 21 days is preferable.
Collect a tape sample from suspicious colonies, stain with lactophenol cotton blue or the purple modified Wright's stain (Diff-Quik-Dade Behring), and then examine at 10x magnification and then 40x to look for macroconidia.
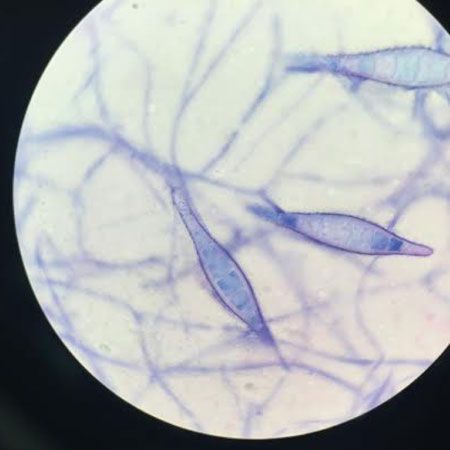
M. canis macroconidia
Ringworm RealPCR Panel
The Ringworm RealPCR Panel (Idexx Laboratories) includes Microsporum and Trichophyton species real-time PCR tests and performs with greater than 95% sensitivity and 99% specificity. Results are available in one to three working days, so it may be helpful for diagnosis in patients you want to start treating immediately.
You have a few options for submitting samples.
Use a soft-bristle toothbrush to comb the suspect lesion, then submit the toothbrush in a plastic, reusable storage bag.
Pluck hair with follicles, lift or remove crusts, or perform skin scrapings from the active border of a suspect lesion, and then place the collected items in a red top tube.
Submit nail bed scrapings or clippings in a sealed fungal envelope or sterile container.
False positive results are possible when monitoring during ringworm treatment since the PCR is sensitive enough to pick up spores from environmental contamination. Use a Wood's lamp to identify appropriate hair samples to help decrease the possibility of a false positive result.
I've recently seen several cases of ringworm in which the fungal PCR result was negative and the DTM result was positive. These discrepancies could've been caused by differences in sampling, but for now, we are performing both ringworm PCR and fungal cultures.
Treatment
Treating ringworm requires a combination of systemic or topical therapy and environmental management. This means that you, your team and the owners will all need to work together.
To monitor treatment progress, perform a repeat culture one to three weeks after beginning therapy and every one to three weeks thereafter. Continue treatment until you obtain two or three negative cultures. Treatment duration is variable and may take between 14 days and six months. In healthy patients, spontaneous resolution may occur within three months.
Drugs
Fluconazole
Dogs: 5 to 10 mg/kg orally, twice a day
Cats: 50 mg/cat orally, once a day
Itraconazole
Dogs and cats: 5 mg/kg orally, once a day for seven days, then stop for seven days; repeat pattern three times
Itraconazole tips:
Avoid alkalinizing agents.
Alanine aminotransferase and serum alkaline phosphatase activities may rise without liver disease signs, although hepatotoxicity is rare.
Generic and compounded itraconazole are not recommended.
I have been impressed with the efficacy and ease of administration of the new formulation, Itrafungol (Elanco).
Terbinafine
Dogs: 30 to 35 mg/kg orally, once a day
Cats: 20 mg/kg orally, once a day
Terbinafine tips:
Some dogs may have hepatotoxicity with terbinafine, but cats do not.
A study showed that terbinafine therapy combined with a weekly lime-sulfur dip resolved ringworm in cats in three weeks.1
No efficacy comparison studies between itraconazole and terbinafine have been done.
Topicals
These dips or washes can be applied or performed once or twice a week:
Lime-sulfur (1:16)
Enilconazole (1:100)
Accelerated hydrogen peroxide rinse (1:20)
Climbazole mousse
Ketoconazole (1% or 2%) shampoo
Miconazole (1% or 2%) shampoo
Environmental control
Ringworm is zoonotic, so instruct owners to wash their hands after handling their pets. If possible, owners should isolate infected animals from noninfected animals. Other pets in the household should either be tested or, if non-symptomatic, can be bathed once weekly with an antifungal shampoo.
To decontaminate their homes, owners should clean all nonporous surfaces with diluted bleach (1:10), Rescue (accelerated hydrogen peroxide), Lysol All-Purpose Cleaner or Formula 409 All-Purpose Cleaner twice a week. Carpeted areas where the ringworm-positive animals are kept should be vacuumed daily. All other floor surfaces, as well as the walls, should be cleaned with Swiffer Sweeper Dry Sweeping Cloths weekly as their electrostatic nature helps attract spores. Any bedding or upholstered items that are difficult to clean, including cat trees, should be thrown out. If the bedding is easy to clean, wash it once a week with hot water and a small amount of bleach or Oxyclean.
For complete instructions on how owners can decontaminate their homes, check out this client handout.
For patients infected with Trichophyton mentagrophytes, reduced exposure to heavily-populated rodent habitats or rodent control is recommended. If rodents are kept as household pets, you can screen them for carriage using the toothbrush technique.
Owners of patients infected with M. canis should have all their cats and dogs assessed as potential carriers. If positive, their pets can be treated with topicals, with or without oral medications. If the owner is able to treat the affected dog, perform adequate environmental control; nonclinical positive pets may have negative cultures/PCRs after weekly antifungal bathing.
Keep your clinic ringworm-free
Prevent contamination in your clinic by isolating dermatophyte-positive patients from other patients. Wear gloves during the examination and change scrubs or laboratory coats before seeing other patients. Clean all nonporous surfaces in the examination rooms with 1:10 bleach, Rescue (accelerated hydrogen peroxide), Lysol All-Purpose Cleaner or Formula 409 All-Purpose cleaner.2
References
1. Moriello KA, Coyner K, Trimmer A, et al. Treatment of shelter cats with oral terbinafine and concurrent lime sulphur rinses. Vet Dermatol 2013;24(6):618-620.
2. Moriello KA, Coyner K, Paterson S, et al. Diagnosis and treatment of dermatophytosis in dogs and cats.: Clinical Consensus Guidelines of the World Association for Veterinary Dermatology. Vet Dermatol 2017;28(3):266-e68.
Anthea Schick DVM, DACVD, practices at Dermatology for Animals in Tempe, Arizona.
UN, WHO address public health concern over avian flu transmission to humans
April 18th 2024Veterinary professionals working with certain animals are advised to take precautionary steps to minimize risk of infection, while researchers in Texas study potential H5N1 vaccines, antivirals, and antibody therapies for humans
Read More