Treating paraneoplastic hypercalcemia in dogs and cats
About 45% to 65% of hypercalcemic dogs and 10% to 30% of hypercalcemic cats have underlying neoplasia.
Preview
- The links: Hypercalcemia is one of the most common paraneoplastic syndromes, and cancer is the most common cause of hypercalcemia in companion animals. Hypercalcemia of malignancy is usually associated with T-cell lymphoma and apocrine gland anal sac adenocarcinoma in dogs and lymphoma, bronchogenic carcinoma, and squamous cell carcinoma in cats.
- The signs: Clinical signs of hypercalcemia include polyuria, polydipsia, lethargy, weakness, nausea, anorexia, vomiting, constipation, diarrhea, and weight loss.
- The tests: The main diagnostic tests include a CBC, a serum chemistry profile, urinalysis, a radiographic or ultrasonographic examination, a rectal examination (in dogs), and ionized calcium, PTH, and PTHrP measurements.
- The treatment: In addition to addressing the primary tumor, supportive treatment consists chiefly of fluid therapy and furosemide, as well as, in some cases, glucocorticoids and aminobisphosphonates.
Cancer accounts for about 50% of all deaths in companion animals more than 10 years of age.1 Cancer-related morbidity and mortality can result not only from neoplastic invasion of vital organs such as the pulmonary parenchyma or liver but also from neoplasm-associated alterations in bodily structure or function that occur distant to the primary tumor and any metastatic lesions. These alterations are classically referred to as paraneoplastic syndromes. Hypercalcemia is a common paraneoplastic syndrome in people and companion animals that frequently contributes to morbidity.2-6 Various tumor-related factors may lead to paraneoplastic hypercalcemia, including the release of humoral peptides, the abnormal expression of membrane-bound ligands, and dysregulated enzymatic pathways responsible for calcium homeostasis.7-9
The most common cause of hypercalcemia in companion animals is cancer, with about 45% to 65% of hypercalcemic dogs and 10% to 30% of hypercalcemic cats having underlying neoplasia.7,10-13 The cancers that most frequently lead to paraneoplastic hypercalcemia are T-cell lymphoma and apocrine gland anal sac adenocarcinoma in dogs and lymphoma, bronchogenic carcinoma, and squamous cell carcinoma in cats.7,10,14 Given the prevalence of cancer in geriatric pets and the morbidity associated with hypercalcemia, this review focuses on the diagnosis and treatment of paraneoplastic hypercalcemia in dogs and cats.
CALCIUM HOMEOSTASIS
Calcium homeostasis is a tightly regulated physiologic process whereby the body maintains steady-state concentrations of ionized calcium, the biologically active fraction of total calcium, in the plasma and extracellular fluid through a dynamic interaction among key hormones and vitamins and their respective target organs. Three principal soluble mediators balance whole body calcium concentrations: parathyroid hormone (PTH), calcitonin, and calcitriol (the biologically active form of vitamin D). PTH and calcitriol are the master regulators of calcium homeostasis, with calcitonin playing a lesser, yet essential role.

Maria Rendon
These mediators exert their biologic activities on three target organs: the kidneys, intestines, and bone matrix. If serum calcium concentrations are decreased, the parathyroid glands secrete PTH to act on 1) the distal renal tubules, causing calcium reabsorption and phosphorus excretion from the kidney; 2) the intestines indirectly through the conversion of calcidiol to highly active calcitriol in the proximal renal tubules, which will increase intestinal absorption of calcium and phosphate; and 3) the bones, either by stimulating the activity of existing bone cells (early effect) or by increasing the number of osteoclasts and their bone resorption activities (late effect) via PTH's effect on osteoblasts.
Conversely, if serum calcium concentrations are elevated, PTH secretion is down-regulated, leading to 1) a net calcium loss through the distal tubules, 2) a reduction in intestinal calcium absorption, and 3) diminished osteoclastic bone resorption. Both PTH and calcitriol promote calcium retention within the body, while calcitonin reduces calcium mobilization from the skeleton chiefly by inhibiting osteoclastic bone resorption.9,15 While PTH has a positive feedback effect on calcitriol synthesis, the main negative feedback mechanisms on calcitriol production are calcitriol itself, as well as hypercalcemia and high phosphorus concentrations.16 Calcitriol also provides a negative feedback effect on PTH secretion.
SERUM CALCIUM CONCENTRATION
Measured total serum calcium is composed of three organic forms: 1) It is bound to plasma proteins (40%); 2) it is complexed as citrates, acetates, and phosphates (10%); and 3) it is ionized or free (50%). Because only the latter form possesses biological activity, ionized calcium measurements are the most physiologically relevant values to obtain when hypercalcemia is suspected based on an elevated total serum calcium concentration.15,16 Depending on the reference laboratory, hypercalcemia is usually defined by a total serum calcium concentration of ≥ 12 mg/dl (3 mmol/L) in dogs and ≥ 11 mg/dl (2.75 mmol/L) in cats.10 True hypercalcemia is confirmed when the ionized calcium concentration is > 1.45 mmol/L in dogs or > 1.4 mmol/L in cats.7
Accurately determining the calcium concentration in critically ill patients is important. So being aware of certain factors' influence on the reliable and precise laboratory assessment of calcium is fundamental. Fasting blood samples are necessary for accurate quantification, as lipemia may falsely increase the measurement of serum calcium.17,18 Appropriate blood sampling technique is equally important to minimize laboratory errors secondary to hemolysis that may interfere with colorimetric analyzer readings.18
Furthermore, hypoproteinemia, especially from hypoalbuminemia, may lead to a relative or spurious decrease in total serum calcium. To compensate for albumin, an adjusted total calcium concentration (mg/dl) can be calculated in dogs by subtracting the measured serum albumin concentration (g/dl) from the measured total serum calcium concentration (mg/dl) and adding 3.5.15,19 However, in some disease conditions, total calcium concentrations corrected for protein may still poorly correlate with ionized calcium concentrations, so they should not be considered a substitute for assessing ionized calcium.20 Also, this formula is not valid in dogs younger than 1 year of age or in cats of any age.
In addition, although ionized calcium is physiologically active, interconversion among all three organic forms can occur and should be considered when managing a critically ill patient. Blood pH or the plasma hydrogen ion concentration may affect the protein binding of calcium, as a larger proportion of total serum calcium exists in a protein-bound form under alkalotic conditions, while acidosis favors calcium ionization.15 So samples collected and processed anaerobically ensure more accurate results, since the pH is less likely to increase from loss of carbon dioxide.15
Finally, ionized calcium and pH are more stable in serum than in whole or heparinized blood, and measured ionized calcium in serum is stable for seven days when collected anaerobically and stored at 39.2 F (4 C).15
CLINICAL SIGNS
Hypercalcemia of malignancy generally results in nonspecific signs that may be insidious and vary in severity. Regardless of the cause of the hypercalcemia, the urinary, neuromuscular, and gastrointestinal systems are most susceptible to the effects of a high calcium concentration. The clinical signs' severity correlates not only with the magnitude of the hypercalcemia but also with the rate of calcium concentration elevation.15 In addition, in cases of hypercalcemia of malignancy, certain clinical signs may be related to the underlying neoplastic disease rather than the secondary hypercalcemia. Thus, therapies should be aimed at treating the underlying cause in addition to the associated clinical consequences.
Urinary signs
The urinary system is severely affected by pathologic elevations in serum calcium concentrations, with primary polyuria and compensatory polydipsia being the most common clinical signs seen in hypercalcemic dogs. Elevated serum calcium concentrations lead to excessive production of dilute urine by inhibiting antidiuretic hormone receptors at the level of the distal renal tubules, causing a secondary nephrogenic diabetes insipidus.15,19 In addition to these functional changes, structural damage in the renal tubules such as mineralization of the basement membrane and secondary tubular degeneration with resulting interstitial fibrosis can exacerbate kidney dysfunction and predispose affected animals to progressive renal failure.
Clinically, azotemia with decreased urine specific gravity or isosthenuria is often detected, and signs of uremia may be present when renal tubule damage is severe and prolonged. Hypercalcemic nephropathy may be partially reversible with appropriate therapy, but progressive renal failure with oliguria and anuria can occur if the condition is left untreated. Overt polydipsia is a compensatory response to the hypercalcemic-induced polyuria and is one of the most common clinical signs reported by pet owners. Despite excessive water consumption, most patients are unable to replenish total body water stores, resulting in moderate to severe dehydration. In an attempt to compensate for the loss of intravascular volume associated with dehydration, an increase in sodium and calcium reabsorption occurs at the proximal tubules, further worsening the ongoing hypercalcemia.
Neurologic signs
In addition to renal tubular epithelium, neurons are also sensitive to abnormal serum calcium concentrations. High ionized calcium concentrations decrease neuronal membrane permeability to sodium, which increases action potential thresholds and reduces neuronal depolarization events.16 Lethargy and weakness are clinical signs often reported by pet owners because of this electrochemical impairment. The concomitant use of narcotics or sedatives may worsen neurologic signs, and cancer patients with central nervous system involvement will also be more severely affected by high serum calcium concentrations.15,19
Gastrointestinal signs
Hypercalcemia also affects the gastrointestinal system, leading to nonspecific signs such as nausea, anorexia, vomiting, constipation, diarrhea, and weight loss. Constipation may develop secondary to depressed contractility of the gastrointestinal smooth muscles, resulting in prolonged intestinal transit times. Furthermore, hypercalcemia may increase gastrin secretion with subsequent increases in hydrochloric acid secretion by parietal cells, leading to upper gastrointestinal irritation and mucosal ulceration.15,16,21 Gastrointestinal signs are among the most common presenting signs in cats with hypercalcemia.
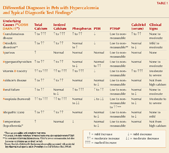
Table 1: Differential Diagnoses in Pets with Hypercalcemia and Typical Diagnostic Test Findings*
DIAGNOSTIC APPROACH TO HYPERCALCEMIC PATIENTS
This review focuses on the common causes of paraneoplastic hypercalcemia. Other important differential diagnoses associated with hypercalcemia in companion animals are presented in Table 1, using the acronym GOSH DARN IT. Once the list of differential diagnoses is understood, it is important to consider a stepwise diagnostic approach in hypercalcemic patients. Table 2 lists diagnostic tests to help you determine the underlying cause of the hypercalcemia, along with the possible findings.
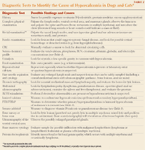
Table 2: Diagnostic Tests to Identify the Cause of Hypercalcemia in Dogs and Cats*
Obtaining a history and performing a complete and thorough physical examination, including rectal palpation in dogs, are always the first steps in evaluating hypercalcemic patients. The CBC and serum chemistry profile results may help you narrow the potential causes of hypercalcemia. For example, if hyperglobulinemia is present (with or without hypoalbuminemia), consider performing serum and urine protein electrophoresis, as well as bone survey radiography and a bone marrow aspiration and cytology, to rule out multiple myeloma.
When the history, physical examination, standard imaging (thoracic radiography, abdominal ultrasonography), and CBC and serum chemistry profile results fail to identify a potential cause, further tests can be considered, such as PTH and PTH-related peptide (PTHrP) concentration measurement and an ultrasonographic examination of the ventral cervical area, ideally by an experienced radiologist. Generally, as with other disorders, the most common conditions are ruled out first by using the least invasive techniques initially.
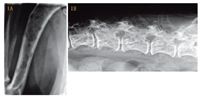
1A & 1B. A ventrodorsal radiograph of the right humerus (1A) and a right lateral radiograph of the lumbar spine (1B) of an 11-year-old female spayed mixed-breed dog presenting with signs of pain. Hypercalcemia, hypoalbuminemia, and hyperglobulinemia were noted on the serum chemistry profile. Multifocal purely lytic lesions are seen. Bone marrow cytology and protein electrophoresis confirmed a diagnosis of multiple myeloma.
Routine tests to detect tumors ("tumor hunting") or complete staging procedures are recommended to better determine the histologic origin and extent of malignancy. Bone survey, via plain radiographs of the long bones and spine (Figures 1A & 1B), or bone scan, via nuclear scintigraphy (Figures 2A & 2B) generally with technetium 99m-ethylenediamine-tetramethylenephosphonic acid (99-Tc-EDTMP), may provide diagnostic clues in cases of occult or unexplained hypercalcemia.
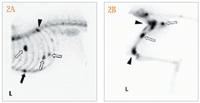
2A & 2B. Bone scintigraphy (99-Tc-EDTMP) in a 12-year-old male neutered mixed-breed dog (the dogs head is to the left) with prostate carcinoma-a tumor type not reported to be associated with hypercalcemia in this species. Increased uptake represents abnormal bone turnover and can be observed in many ribs (2A-open arrows) , in the sternum (2A-solid arrow), in the thoracic spine (2A-arrowhead), and in the femoral diaphysis and ischium (2B-open arrows). Nonspecific uptake is also observed in the coxofemoral and stifle joints from osteoarthritis (2B-arrowheads). Cytologic examination confirmed that a target bone lesion (femur) was metastatic.
HYPERCALCEMIA OF MALIGNANCY: PATHOGENESIS
Hypercalcemia of malignancy may arise through three main mechanisms. First, tumor cells may produce and liberate soluble mediators capable of acting on bone and kidneys through endocrine and paracrine pathways, a mechanism referred to as humoral hypercalcemia of malignancy.3-5,7,8,15,19 Second, cancer cells may subvert the enzymatic activity of 1 alpha-hydroxylase, thereby causing the unregulated conversion of calcidiol to active calcitriol, which enhances intestinal absorption of calcium.8,22-26 This mechanism is poorly described with tumors in companion animals. Finally, certain tumor histologies such as leukemias, lymphomas, myeloma, and certain carcinomas may directly cause osteolysis when they invade or metastasize to bones, resulting in the dissolution of hydroxyapatite crystals through an agonist effect on osteoclasts during tumor progression.9,27
Humoral hypercalcemia of malignancy
Humoral hypercalcemia of malignancy may involve the malignant secretion of PTHrP, a polypeptide structurally similar to intact PTH, as well as the liberation of cytokines such as interleukin-1, interleukin-6, or tumor necrosis factor.3-5,7,8,15,19 The production and secretion of these humoral mediators lead to pathologic increases in osteoclastic resorption, often without visible radiographic bone lesions. The most common cancers associated with humoral hypercalcemia of malignancy in dogs are T-cell lymphoma (see boxed text titled "Canine T-cell lymphoma: The most common cause of hypercalcemia of malignancy in dogs") and apocrine gland anal sac adenocarcinoma (see boxed text titled "Apocrine gland anal sac adenocarcinoma: The second most common cause of hypercalcemia of malignancy in dogs")8 ; while in cats lymphoma, bronchogenic carcinoma, and squamous cell carcinoma are most commonly reported.7,10,28,29 Other tumors such as leukemias,30,31 thymoma,32,33 malignant melanoma,34 acanthomatous ameloblastoma,35 and various carcinomas have been sporadically reported to secrete PTHrP in dogs.36-40
Like its physiologic counterpart, PTHrP binds to PTH1 receptors on osteoblasts and renal tubular cells to exert its hypercalcemic effects.9,15,16,22 Some growth factors, such as epidermal growth factor and transforming growth factor-beta, increase PTHrP expression.15,22,41 Animals with hypercalcemia due to elevated PTHrP concentrations typically exhibit moderate to marked hypercalcemia, hypophosphatemia, and hypercalciuria with decreased fractional calcium excretion and increased fractional phosphorus excretion. For a supportive diagnosis of humoral hypercalcemia of malignancy, circulating PTHrP concentrations may be assessed by sending EDTA plasma samples to commercial laboratories.8
While it may seem at first that PTHrP is an abnormal hormone produced only by certain cancer cells, this hormone is produced by normal tissues in certain conditions and participates in calcium homeostasis and metabolism. For example, PTHrP is known to function in an endocrine manner in the fetus and is produced by the fetal parathyroid glands and the placenta, permitting ionized calcium uptake by the fetus.15 It is also produced by the mammary gland in lactating dams to facilitate calcium mobilization from maternal bones and may play a role in the transport of calcium into the milk.15 Finally, although the circulating blood concentrations are low in normal adults, PTHrP has been demonstrated in some epithelial tissues, endocrine glands, muscles, bone, brain, and lymphocytes.15
Local osteolytic tumors
Metastatic carcinomas are commonly associated with malignant osteolysis in people and can lead to hypercalcemia both through humoral hypercalcemia of malignancy or direct osteolytic mechanisms. These tumors express osteotropism, or the affinity and ability to grow within bone; the exact mechanisms behind this phenomenon have yet to be fully characterized.
Tumor cells' presence within the bone microenvironment can increase the number and activity of local osteoclasts through the paracrine release of factors such as interleukin-1, interleukin-6, tumor necrosis factor-alpha and tumor necrosis factor-beta, receptor activator of nuclear factor kappa-B ligand (RANKL), and prostaglandins, leading to localized bone resorption.15 Excessive focal bone resorption can cause bone pain, predispose patients to pathologic fracture, and induce hypercalcemia. These malignant clinical consequences occur most typically in companion animals with multiple myeloma and metastatic carcinomas of urinary bladder, prostate, and mammary gland origins and occasionally with lymphoma and leukemias.19,42-44 In cats, squamous cell carcinoma and osteosarcoma have been associated with hypercalcemia, possibly resulting from local osteolysis.10
THERAPY
Fluid therapy
For any paraneoplastic syndrome, diagnosing and treating the underlying neoplastic disorder is mandatory to best manage the patient. However, pending definitive diagnosis of the primary disease, initial intervention for hypercalcemia should ideally consist of vigorous rehydration with isotonic saline solution (0.9% sodium chloride). Severe dehydration and hemoconcentration associated with hypercalcemia are common because of the anorexia, vomiting, and calcium-associated polyuria, despite the compensatory polydipsia. A decreased glomerular filtration rate leads to additional calcium retention as the kidneys attempt to conserve sodium. To reverse the established vicious cycle and increase calciuresis through an improved glomerular filtration rate, fluids devoid of calcium such as physiologic saline are usually recommended. In addition, the fluid of choice will have a high sodium concentration, since the sodium will compete with calcium for tubular reabsorption, resulting in enhanced calciuresis.15 However, the aggressive fluid therapy per se is more important than the actual type of fluid given, and lactated Ringer's solution can be used if saline solution is not available.
After adequate hydration, a patient's kidneys will first excrete sodium and then calcium, with clinical improvement usually seen within 24 hours of fluid therapy. Take the patient's hydration, renal, and cardiovascular status into consideration when determining the fluid rate. Potassium supplementation may be required in some cases to avoid hypokalemia, especially if prolonged potassium-free intravenous fluid therapy is administered. Intravenous fluid therapy should aim to correct the dehydration over four to six hours after diagnosis in patients with moderate to severe hypercalcemia.
Loop diuretics
A loop diuretic, most commonly furosemide, may be added to the therapeutic regimen once the patient is adequately rehydrated. Furosemide inhibits the renal membrane sodium-potassium-dichloride cotransporter present in the thick ascending limb of Henle's loop.45,46 The Handbook of Small Animal Therapeutics, edited by Lloyd E. Davis in 1985, is one of the first references recommending the use of furosemide for hypercalcemia treatment in dogs. The original recommended dosage was an initial bolus of 5 mg/kg followed by a constant-rate infusion (CRI) of 5 mg/kg/hr intravenously. This high dose of furosemide is based on human antihypercalcemic therapy and strictly requires a high rate of intravenous fluid administration (> three times maintenance fluid requirement) to avoid iatrogenic dehydration. We prefer using a lower dose of furosemide initially (2 to 4 mg/kg t.i.d. to q.i.d. intravenously, subcutaneously, or orally) to minimize the need for a high fluid rate.
In a recent study of six normocalcemic greyhounds, a 0.66-mg/kg loading dose of furosemide followed by a CRI of 0.66 mg/kg/hr (equivalent to 6 mg/kg over eight hours) was evaluated for its calciuretic efficacy compared with the same total dose of furosemide administered via two intravenous boluses of 3 mg/kg given four hours apart.47 Urine sodium and calcium loss as well as urine production and water intake were significantly larger in the CRI group compared with the intravenous bolus groups. The study concluded that the same total dose of furosemide over a given time frame resulted in more diuresis, natriuresis, and calciuresis, as well as less kaliuresis, compared with repeated intravenous boluses.47 Similar to the results obtained in normal greyhounds, it is our experience that the low-dose bolus followed by a CRI effectively reduces the degree of hypercalcemia.
Thiazide diuretics are absolutely contraindicated because of their hypercalcemic effect, as they cause tubular reabsorption of calcium rather than calciuresis.15,22
Glucocorticoids
The use of glucocorticoids is controversial for treating hypercalcemia and is not a component of standard therapy in people because of glucocorticoids' side effects and limited therapeutic value. The exact mechanisms of action of glucocorticoids in hypercalcemia are unknown, though it has been suggested that they increase renal calcium excretion, reduce bone resorption, and potentially decrease intestinal absorption.15,16,19 Glucocorticoids are most effective for hypercalcemia secondary to lymphoma, as they then also are part of the cytotoxic therapy aimed at the underlying cause. Prednisone at a dosage of 1 to 2.2 mg/kg given twice a day intravenously, subcutaneously, or orally or dexamethasone at a dosage of 0.1 to 0.22 mg/kg given twice a day intravenously, subcutaneously, or orally has been recommended.19,22 These high dosages should not be maintained indefinitely, and appropriate tapering is advised.
Glucocorticoids are included in most conventional lymphoma chemotherapy protocols, but their initial use should be avoided for two reasons. First, they may delay the definitive diagnosis and appropriate therapy of a malignant lymphoproliferative disease such as lymphoma. Additionally, their prolonged use may result in an increased risk of multidrug resistance (MDR phenotype), thereby negatively affecting the prognosis and chance of a long-lasting remission once appropriate multiagent cytotoxic therapy is instituted.48
Aminobisphosphonates
Together with rehydration, potent injectable aminobisphosphonates, chiefly zoledronate and pamidronate, are currently the cornerstone of therapy for malignancy-associated hypercalcemia in people.9,49,50 They are considered the safest and most effective drugs for that purpose. Human malignant hypercalcemia most commonly results from multiple myeloma and solid carcinomas (e.g. breast, lung, prostate, renal) with bone metastases.9,15 Bisphosphonates are organic pyrophosphate analogues that possess high affinity for bone hydroxyapatite crystals and, thus, highly concentrate in sites of active bone turnover.
Bisphosphonates exert their main biologic effect by inducing osteoclast apoptosis.49 The inhibition of global osteoclastic activity decreases overall bone resorption and calcium release from the bone compartment.51-53 In people, bisphosphonates are usually initiated as soon as hypercalcemia is discovered since the response is not immediate. Blood calcium concentrations normalize within four to 10 days, and the effect lasts for about one to four weeks.52,53 Either pamidronate or zoledronate is acceptable; however, zoledronate is the most potent of the two formulations and is the current best choice in human medicine.9 Bisphosphonates that do not contain a nitrogen atom in their side chain, such as etidronate and clodronate, are not as potent as aminobisphosphonates in their antiresorptive activity and are generally not recommended for hypercalcemia of malignancy.51
While zoledronate administration also appears effective in dogs and cats, it remains cost-prohibitive in veterinary medicine. On the other hand, pamidronate is less expensive and is a good choice in hypercalcemic companion animals. Its use has been demonstrated in dogs at the recommended dosage of 1.3 to 2 mg/kg given once intravenously over 20 minutes or two hours in cases of experimental vitamin D toxicosis.54-56 An alternative safe dosage we are familiar with is 1 to 2 mg/kg given intravenously over two hours every 21 to 28 days in dogs.57 A dosage we are familiar with in cats is 1 to 1.5 mg/kg given intravenously over two hours every 21 to 28 days.
Because aminobisphosphonates act strictly at the bone level, a more pronounced effect on the hypercalcemia is obtained, both in human and veterinary patients, when their use is combined with therapies acting at the kidney level (saline diuresis, a loop diuretic) or in cases of hypercalcemia resulting from pure osteolytic processes rather than hypercalcemia secondary to increased quantities of calcitriol, PTH, or PTHrP.8
Other therapies
Other therapeutic agents have been recommended but have minor use in small-animal medicine because of their cost, side effects, or scheduling of administration. These agents include mithramycin, calcitonin, and gallium nitrate.
Mithramycin, also known as plicamycin, is an antitumor antibiotic with potent inhibitory effects on osteoclasts, leading to rapid inhibition of bone resorption. In a study of dogs with cancer-associated hypercalcemia, mithramycin was used as a single infusion of 0.1 mg/kg.58 Unfortunately, patients developed clinical signs of fever, vomiting, and diarrhea shortly after administration and suffered hepatocellular injury with subsequent hepatic necrosis. Other clinical consequences such as thrombocytopenia and renal necrosis have also been reported.59 Although unacceptable toxicosis is observed at 0.1 mg/kg, the use of mithramycin at a lower dosage (25 µg/kg infused over four hours) successfully controlled hypercalcemia for 24 to 72 hours.19
Similarly to the mechanism of mithramycin, calcitonin reduces osteoclastic activity and reduces hypercalcemia in small animals with vitamin D toxicosis.60,61 Reported dosages range from 4.5 to 8 IU/kg given subcutaneously every eight hours to 5 IU/kg given subcutaneously every 12 hours.61,62 For cats with rodenticide toxicosis, a dosage of 4 IU/kg given intramuscularly every 12 hours was effective and well-tolerated.63 Unlike calcitonin's documented modest efficacy for the treatment of hypercalcemia secondary to vitamin D toxicosis, calcitonin's utility in successfully managing hypercalcemia of malignancy in companion animals remains to be investigated. Calcitonin is used in people with Paget's disease and hypercalcemia of malignancy, but the effects of treatment can be quite variable.64-66 The main side effects of calcitonin are anorexia and vomiting. Its use is limited by cost and the fact that its effects are short-lived and because resistance frequently develops in a matter of days.15
Gallium nitrate is an antineoplastic that binds to the hydroxyapatite crystals in bone, thereby reducing their solubility.67,68 In some studies, gallium nitrate was demonstrated to be more effective than bisphosphonates at reducing calcium concentrations in people with hypercalcemia.69 However, despite this apparent efficacy, it is not considered a first-line treatment option for managing hypercalcemia given its potential for nephrotoxicity.
Novel therapies targeting the intercellular communication of osteoblasts and osteoclasts are under investigation. RANKL is expressed by osteoblasts and T lymphocytes and binds to its cognate receptor, receptor activator of nuclear factor kappa-B (RANK), present on the surface of osteoclast precursors and osteoclasts, leading to their proliferation, maturation, and activation. Promising antiresorptive molecules such as osteoprotegerin analogues, a soluble decoy RANKL receptor, or RANK nonfunctional constructs are being evaluated to decrease osteoclast activity and pathologic bone resorption.9,70
CONCLUSION
Paraneoplastic hypercalcemia is a common and serious complication observed in small-animal cancer patients. Various tumor types are capable of inducing hypercalcemia in cancer patients through multiple mechanisms that subvert or dysregulate calcium homeostasis. Canine T-cell lymphoma is the most common neoplasia associated with hypercalcemia, but other less frequent cancers and non-neoplastic diseases should be considered as important differential diagnoses in any patient with pathologic serum calcium elevations. Familiarity with clinical signs associated with hypercalcemia may allow for the early detection of underlying disease processes. The timely institution of definitive treatments and supportive management strategies will minimize the morbidity, and potential mortality, in companion animals suffering from hypercalcemia of malignancy.
Pamela Lucas, DVM
Hugues Lacoste, DVM, DACVIM (oncology)
Louis-Philippe de Lorimier, DVM, DACVIM (oncology)
Timothy M. Fan, DVM, PhD, DACVIM (oncology, internal medicine)
Department of Veterinary Clinical Medicine
College of Veterinary Medicine
University of Illinois
Urbana, IL 61802
REFERENCES
1. Bronson RT. Variation in age at death of dogs of different sexes and breeds. Am J Vet Res 1982;43:2057-2059.
2. Guise TA, Mohammad KS, Clines G, et al. Basic mechanisms responsible for osteolytic and osteoblastic bone metastases. Clin Cancer Res 2006;12(20 Pt 2):6213s-6216s.
3. Rankin W, Grill V, Martin TJ. Parathyroid hormone-related protein and hypercalcemia. Cancer 1997;80(8 Suppl):1564-1571.
4. Weir EC, Norrdin RW, Matus RE, et al. Humoral hypercalcemia of malignancy in canine lymphosarcoma. Endocrinology 1988;122;602-608.
5. Weller RE. Paraneoplastic disorders in dogs with hematopoietic tumors. Vet Clin North Am Small Anim Pract 1985;15:805-816.
6. Williams LE, Gliatto JM, Dodge RK, et al. Carcinoma of the apocrine glands of the anal sac in dogs: 113 cases (1985-1995). J Am Vet Med Assoc 2003;223:825-831.
7. Bolliger AP, Graham PA, Richard V, et al. Detection of parathyroid hormone-related protein in cats with humoral hypercalcemia of malignancy. Vet Clin Pathol 2002;31:3-8.
8. Rosol TJ, Nagode LA, Couto CG, et al. Parathyroid hormone (PTH)-related protein, PTH, and 1,25-dihydroxyvitamin D in dogs with cancer-associated hypercalcemia. Endocrinology 1992;131:1157-1164.
9. Clines GA, Guise TA. Hypercalcaemia of malignancy and basic research on mechanisms responsible for osteolytic and osteoblastic metastasis to bone. Endocr Relat Cancer 2005;12:549-583.
10. Savary KC, Price GS, Vaden SL. Hypercalcemia in cats: a retrospective study of 71 cases (1991-1997). J Vet Intern Med 2000;14:184-189.
11. Sakals S, Peta HG, Fernandez NJ, et al. Determining the cause of hypercalcemia in a dog. Can Vet J 2006;47:819-821.
12. Uehlinger P, Glaus T, Hauser B, et al. Differential diagnosis of hypercalcemia—a retrospective study of 46 dogs [German]. Schweiz Arch Tierheilkd 1998;140:188-197.
13. Elliot J, Dobson JM, Dunn DK, et al. Hypercalcemia in the dog: a study of 40 cases. J Small Anim Pract 1991;32:564-571.
14. Chew DJ, Carothers M. Hypercalcemia. Vet Clin North Am Small Anim Pract 1989;19:265-287.
15. Schenck PA, Chew DJ, Nagode LA, et al. Disorders of calcium: hypercalcemia and hypocalcemia. In: DiBartola S, ed. Fluid, electrolyte, and acid-base disorders in small animal practice. 3rd Ed. St. Louis, Mo: Elsevier, 2006;122-194.
16. Guyton AC, Hall JE. Parathyroid hormone, calcitonin, calcium and phosphate metabolism, vitamin D, bone and teeth. In: Guyton AC, Hall JE. Textbook of medical physiology. 10th ed. Philadelphia, Pa: WB Saunders Co, 2000;899-910.
17. Thomas JS. Introduction to serum chemistries: artifacts in biochemical determinations. In: Willard MD, Tvedten H. Small animal clinical diagnosis by laboratory methods. 4th ed. St. Louis, Mo: Elsevier, 2004;113-116.
18. Alleman AR. The effects of hemolysis and lipemia on biochemical constituents. Vet Med 1990;85:1272-1284.
19. Morrison WB. Paraneoplastic syndromes and the tumors that cause them. In: Morrison WB. Cancer in dogs and cats: medical and surgical management. 2nd ed. Jackson, Wyo: Teton NewMedia, 2002;731-735.
20. Schenck PA, Chew DJ. Prediction of serum ionized calcium concentration by use of serum total calcium concentration in dogs. Am J Vet Res 2005;66:1330-1336.
21. Kowalewski K, Kolodej A. Effects of calcium infusion on secretion and motor activity of totally isolated canine stomach perfused with homologous blood. Pharmacology 1976;14:537-549.
22. Feldman EC, Nelson RW. Hypercalcemia and primary hyperparathyroidism. Canine and feline endocrinology and reproduction. 3rd ed. St. Louis, Mo: Saunders, 2004;660-715.
23. Seymour JF, Gagel RF. Calcitriol: the major humoral mediator of hypercalcemia in Hodgkin's disease and non-Hodgkin's lymphomas. Blood 1993;82:1383-1394.
24. Seymour JF, Gagel RF, Hagemeister FB, et al. Calcitriol production in hypercalcemic and normocalcemic patients with non-Hodgkin lymphoma. Ann Intern Med 1994;121:633-640.
25. Craanen ME, van Beugen L, Blok P. Non-Hodgkin's lymphoma and 1,25(OH)2D-related hypercalcaemia. Neth J Med 1990;37:129-131.
26. Davies M, Hayes ME, Yin JA, et al. Abnormal synthesis of 1,25-dihydroxyvitamin D in patients with malignant lymphoma. J Clin Endocrinol Metab 1994;78:1202-1207.
27. Rosol TJ. Pathogenesis of bone metastasis: role of tumor-related proteins. J Bone Miner Res 2000;15:844-850.
28. Anderson TE, Legendre AM, McEntee MM. Probable hypercalcemia of malignancy in a cat with bronchogenic adenocarcinoma. J Am Anim Hosp Assoc 2000;36:52-55.
29. Tannehill-Gregg S, Kergosien E, Rosol TJ. Feline head and neck squamous cell carcinoma cell line: characterization, production of parathyroid hormone-related protein, and regulation by transforming growth factor-beta. In Vitro Cell Dev Biol Anim 2001;37:676-683.
30. Kleiter M, Hirt R, Kirtz G, et al. Hypercalcaemia associated with chronic lymphocytic leukaemia in a Giant Schnauzer. Aust Vet J 2001;79:335-338.
31. Henry CJ, Lanevschi A, Marks SL, et al. Acute lymphoblastic leukemia, hypercalcemia, and pseudohyperkalemia in a dog. J Am Vet Med Assoc 1996;208:237-239.
32. Foley P, Shaw D, Runyon C, et al. Serum parathyroid hormone-related protein concentration in a dog with a thymoma and persistent hypercalcemia. Can Vet J 2000;41:867-870.
33. Mellanby RJ, Mellor PJ, Herrtage ME. What is your diagnosis? Thymoma. J Small Anim Pract 2004;45:589, 626-628.
34. Pressler BM, Rotstein DS, Law JM, et al. Hypercalcemia and high parathyroid hormone-related protein concentration associated with malignant melanoma in a dog. J Am Vet Med Assoc 2002;221:263-265.
35. Dhaliwal RS, Tang KN. Parathyroid hormone-related peptide and hypercalcaemia in a dog with functional keratinizing ameloblastoma. Vet Comp Oncol 2005;3:98-100.
36. Bennett PF, DeNicola DB, Bonney P, et al. Canine anal sac adenocarcinomas: clinical presentation and response to therapy. J Vet Intern Med 2002;16:100-104.
37. Bertazzolo W, Comazzi S, Roccabianca P, et al. Hypercalcaemia associated with a retroperitoneal apocrine gland adenocarcinoma in a dog. J Small Anim Pract 2003;44:221-224.
38. Konno A, Sukegawa A, Kusano M, et al. Immunohistochemistry for parathyroid hormone-related protein (PTHrP) in benign and malignant mammary mixed tumors of dogs with and without hypercalcemia. Jpn J Vet Res 2000;47:155-162.
39. Anderson GM, Lane I, Fischer J, et al. Hypercalcemia and parathyroid hormone-related protein in a dog with undifferentiated nasal carcinoma. Can Vet J 1999;40:341-342.
40. Hori Y, Uechi M, Kanakubo K, et al. Canine ovarian serous papillary adenocarcinoma with neoplastic hypercalcemia. J Vet Med Sci 2006;68:979-982.
41. Motellon JL, Jimenez FJ, de Miguel F, et al. Relationship of plasma bone cytokines with hypercalcemia in cancer patients. Clin Chim Acta 2000;302:59-68.
42. Barthez PY, Davis CR, Pool RR, et al. Multiple metaphyseal involvement of a thymic lymphoma associated with hypercalcemia in a puppy. J Am Anim Hosp Assoc 1995;31:82-85.
43. Villiers E, Dobson J. Multiple myeloma with associated polyneuropathy in a German shepherd dog. J Small Anim Pract 1998;39:249-251.
44. Matus RE, Leifer CE, MacEwen EG, et al. Prognostic factors for multiple myeloma in the dog. J Am Vet Med Assoc 1986;188:1288-1292.
45. Brater DC. Clinical pharmacology of loop diuretics. Drugs 1991;41(Suppl 3):14-22.
46. Puschett JB. Pharmacological classification and renal actions of diuretics. Cardiology 1994;84(Suppl 2):4-13.
47. Adin DB, Taylor AW, Hill RC, et al. Intermittent bolus injection versus continuous infusion of furosemide in normal adult greyhound dogs. J Vet Intern Med 2003;17:632-636.
48. Price GS, Page RL, Fischer BM, et al. Efficacy and toxicity of doxorubicin/cyclophosphamide maintenance therapy in dogs with multicentric lymphosarcoma. J Vet Intern Med 1991;5:259-262.
49. Body JJ, Coleman RE, Piccart M. Use of bisphosphonates in cancer patients. Cancer Treat Rev 1996;22:265-287.
50. Tenta R, Sourla A, Lembessis P, et al. Bone-related growth factors and zoledronic acid regulate the PTHrP/PTH.1 receptor bioregulation systems in MG-63 human osteosarcoma cells. Anticancer Res 2006;26(1A):283-291.
51. Milner RJ, Farese J, Henry CJ, et al. Bisphosphonates and cancer. J Vet Intern Med 2004;18:597-604.
52. Rogers MJ, Watts DJ, Russell RG. Overview of bisphosphonates. Cancer 1997;80(8 Suppl):1652-1660.
53. Sonnemann J, Eckervogt V, Truckenbrod B, et al. The bisphosphonate pamidronate is a potent inhibitor of human osteosarcoma cell growth in vitro. Anticancer Drugs 2001;12:459-465.
54. Rumbeiha WK, Fitzgerald SD, Kruger JM, et al. Use of pamidronate disodium to reduce cholecalciferol-induced toxicosis in dogs. Am J Vet Res 2000;61:9-13.
55. Rumbeiha WK, Kruger JM, Fitzgerald SF, et al. Use of pamidronate to reverse vitamin D3-induced toxicosis in dogs. Am J Vet Res 1999;60:1092-1097.
56. Hostutler RA, Chew DJ, Jaeger JQ, et al. Uses and effectiveness of pamidronate disodium for treatment of dogs and cats with hypercalcemia. J Vet Intern Med 2005;19:29-33.
57. Fan TM, de Lorimier LP, Charney SC, et al. Evaluation of intravenous pamidronate administration in 33 cancer-bearing dogs with primary or secondary bone involvement. J Vet Intern Med 2005;19:74-80.
58. Rosol T, Chew D, Hammer A. Effect of mithramycin on hypercalcemia in dogs. J Am Anim Hosp Assoc 1994;30:244-250.
59. Rosol TJ, Chew DJ, Couto CG, et al. Effects of mithramycin on calcium metabolism and bone in dogs. Vet Pathol 1992;29:223-229.
60. Scheftel J, Setzer S, Walser M, et al. Elevated 25-hydroxy and normal 1,25-dihydroxy cholecalciferol serum concentrations in a successfully-treated case of vitamin D3 toxicosis in a dog. Vet Hum Toxicol 1991;33:345-348.
61. Dougherty SA, Center SA, Dzanis DA. Salmon calcitonin as adjunct treatment for vitamin D toxicosis in a dog. J Am Vet Med Assoc 1990;196:1269-1272.
62. Fooshee SK, Forrester SD. Hypercalcemia secondary to cholecalciferol rodenticide toxicosis in two dogs. J Am Vet Med Assoc 1990;196:1265-1268.
63. Peterson EN, Kirby R, Sommer M, et al. Cholecalciferol rodenticide intoxication in a cat. J Am Vet Med Assoc 1991;199:904-906.
64. Inzerillo AM, Zaidi M, Huang CL. Calcitonin: physiological actions and clinical applications. J Pediatr Endocrinol Metab 2004;17:931-940.
65. Chen P, Lai JM, Deng JF, et al. Relative bioavailability of salmon calcitonin given intramuscularly. Zhonghua Yi Xue Za Zhi (Taipei) 2000;63:619-627.
66. Grauer A, Ziegler R, Raue F. Clinical significance of antibodies against calcitonin. Exp Clin Endocrinol Diabetes 1995;103:345-351.
67. Warrell RP Jr. Gallium nitrate for the treatment of bone metastases. Cancer 1997;80(8 Suppl):1680-1685.
68. Hughes TE, Hansen LA. Gallium nitrate. Ann Pharmacother 1992;26:354-362.
69. Cvitkovic F, Armand JP, Tubiana-Hulin M, et al. Randomized, double-blind, phase II trial of gallium nitrate compared with pamidronate for acute control of cancer-related hypercalcemia. Cancer J 2006;12:47-53.
70. Morony S, Warmington K, Adamu S, et al. The inhibition of RANKL causes greater suppression of bone resorption and hypercalcemia compared with bisphosphonates in two models of humoral hypercalcemia of malignancy. Endocrinology 2005;146:3235-3243.
Canine T-cell lymphoma
The most common cause of hypercalcemia of malignancy in dogs
Dogs with hypercalcemia-associated lymphoma are considered to have clinical substage B disease and more likely have a T-cell immunophenotype, both known negative prognostic variables for remission duration and survival time.1-7 These malignant cells have the potential to secrete PTHrP.8-14
Lymphoma (T-cell) is the most common underlying cause of severe hypercalcemia in dogs and should be considered a top differential diagnosis for any dog presenting with this finding on a serum chemistry profile. Palpable lymph nodes (Figure A) or skin masses should be aspirated or biopsied for cytologic or histologic evaluation, respectively. A cranial mediastinal mass can be identified on plain thoracic radiographs, which should be part of a hypercalcemia workup (Figures B-E).
Other diagnostic tests may be needed to confirm a diagnosis of mediastinal lymphoma, such as thoracic ultrasonography with fine-needle aspiration or Tru-Cut biopsies of the suspect mass. Cytologic or histologic confirmation may differentiate lymphoma from thymoma, another tumor occasionally associated with paraneoplastic hypercalcemia in dogs and cats (Figures F & G). Abdominal radiography, abdominal ultrasonography, and bone marrow aspiration and cytology are recommended in cases of hypercalcemia of unknown origin and suspected lymphoid tumors. Humoral hypercalcemia of malignancy with normal PTHrP concentrations may be identified in some lymphoma cases and may occur because PTHrP can be sporadically released by the tumor or because some lymphoma cells possess 1 alpha-hydroxylase activities that lead to a syndrome of dysregulated 1,25-dihydroxycholecalciferol (calcitriol) formation, although this mechanism of paraneoplastic hypercalcemia has been rarely reported in companion animals.9,15-19
REFERENCES
1. Barthez PY, Davis CR, Pool RR, et al. Multiple metaphyseal involvement of a thymic lymphoma associated with hypercalcemia in a puppy. J Am Anim Hosp Assoc 1995;31:82-85.
2. Wilkerson MJ, Dolce K, Koopman T, et al. Lineage differentiation of canine lymphoma/leukemias and aberrant expression of CD molecules. Vet Immunol Immunopathol 2005;106:179-196.
3. Garrett LD, Thamm DH, Chun R, et al. Evaluation of a 6-month chemotherapy protocol with no maintenance therapy for dogs with lymphoma. J Vet Intern Med 2002;16:704-709.
4. Chun R, Garrett LD, Vail DM. Evaluation of a high-dose chemotherapy protocol with no maintenance therapy for dogs with lymphoma. J Vet Intern Med 2000;14:120-124.
5. Greenlee PG, Filippa DA, Quimby FW, et al. Lymphomas in dogs. A morphologic, immunologic, and clinical study. Cancer 1990;66:480-490.
6. Sarmiento UM, Valli VE. Lymphocyte 5'-nucleotidase activities in normal dogs and in dogs with malignant lymphoma. Vet Immunol Immunopathol 1986;13:281-288.
7. Ruslander DA, Gebhard DH, Tompkins MB, et al. Immunophenotypic characterization of canine lymphoproliferative disorders. In Vivo 1997;11:169-172.
8. Weir EC, Norrdin RW, Matus RE, et al. Humoral hypercalcemia of malignancy in canine lymphosarcoma. Endocrinology 1988;122;602-608.
9. Rosol TJ, Nagode LA, Couto CG, et al. Parathyroid hormone (PTH)-related protein, PTH, and 1,25-dihydroxyvitamin D in dogs with cancer-associated hypercalcemia. Endocrinology 1992;131:1157-1164.
10. Clines GA, Guise TA. Hypercalcaemia of malignancy and basic research on mechanisms responsible for osteolytic and osteoblastic metastasis to bone. Endocr Relat Cancer 2005;12:549-583.
11. Schenck PA, Chew DJ, Nagode LA, et al. Disorders of calcium: hypercalcemia and hypocalcemia. In: DiBartola S, ed. Fluid, electrolyte, and acid-base disorders in small animal practice. 3rd Ed. St. Louis, Mo: Elsevier, 2006;122-194.
12. Feldman EC, Nelson RW. Canine and feline endocrinology and reproduction. 3rd ed. St. Louis, Mo: Saunders, 2004;660-715.
13. Fournel-Fleury C, Ponce F, Felman P, et al. Canine T-cell lymphomas: a morphological, immunological, and clinical study of 46 new cases. Vet Pathol 2002;39:92-109.
14. Grone A, Werkmeister JR, Steinmeyer CL, et al. Parathyroid hormone-related protein in normal and neoplastic canine tissues: immunohistochemical localization and biochemical extraction. Vet Pathol 1994;31:308-315.
15. Morrison WB. Paraneoplastic syndromes and the tumors that cause them. In: Morrison WB. Cancer in dogs and cats: medical and surgical management. 2nd ed. Jackson, Wyo: Teton NewMedia, 2002;731-735.
16. Schenck PA, Chew DJ. Prediction of serum ionized calcium concentration by use of serum total calcium concentration in dogs. Am J Vet Res 2005;66:1330-1336.
17. Kowalewski K, Kolodej A. Effects of calcium infusion on secretion and motor activity of totally isolated canine stomach perfused with homologous blood. Pharmacology 1976;14:537-549.
18. Sakals S, Peta HG, Fernandez NJ, et al. Determining the cause of hypercalcemia in a dog. Can Vet J 2006;47:819-821.
19. Uehlinger P, Glaus T, Hauser B, et al. Differential diagnosis of hypercalcemia—a retrospective study of 46 dogs [German]. Schweiz Arch Tierheilkd 1998;140:188-197.
A. A 10-year-old intact female American bulldog presenting with pronounced peripheral lymphadenopathy, eventually diagnosed as diffuse large T-cell lymphoma on histologic examination. Markedly enlarged superficial cervical (prescapular) and mandibular lymph nodes are easily visible.

B & C. Lateral and ventrodorsal thoracic radiographs of a 6-year-old spayed female boxer presenting with dyspnea, polyuria, and polydipsia. Severe hypercalcemia (20.4 mg/dl) and azotemia were noted on the serum chemistry profile. Note the pleural effusion and a large soft tissue opacity in the cranial mediastinum displacing the lungs caudodorsally.
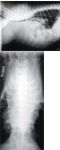
D & E. Lateral and ventrodorsal thoracic radiographs of the same dog five weeks after a standard combination chemotherapy protocol was initiated. Dyspnea and hypercalcemia rapidly resolved after supportive therapy and cytotoxic chemotherapy were initiated.
F & G. Cytologic preparations of fine-needle aspirates from cranial mediastinal masses in two different dogs. Figure F shows a monomorphic population of intermediate to large lymphocytes, with large nuclei, prominent nucleoli (arrowheads), and an open chromatin pattern, consistent with lymphoma (Wright's-Giemsa, 1,000x). Figure G shows a mixed population of small and intermediate lymphocytes, with occasional mast cells (arrowheads), suggestive of thymoma despite the absence of epithelial cells on this sample (Wright's-Giemsa, 400x). (Photomicrographs courtesy of Dr. Laura D. Garrett.)


Apocrine gland anal sac adenocarcinoma
The second most common cause of hypercalcemia of malignancy in dogs
In dogs, apocrine gland anal sac adenocarcinomas are the second most common neoplastic cause of hypercalcemia of malignancy.1 The secretion of pthrp by carcinoma cells is generally the cause of calcium elevations.1-3 It is reported that 25% to 51% of dogs with apocrine gland anal sac adenocarcinomas are hypercalcemic,4-6 and the identification of elevated calcium concentrations at diagnosis has been inconsistently associated with shorter survival times.4,5
Given the relatively high incidence of serum calcium elevations in patients with apocrine gland anal sac adenocarcinoma, a careful rectal examination should be an integral part of the physical examination in dogs with hypercalcemia (see figure). Primary anal sac tumors may be small, so thorough and careful palpation of the anal sacs may be necessary for tumor detection. In addition, because it is not uncommon for apocrine gland anal sac adenocarcinomas to have regional metastatic disease in the iliac lymph nodes that may be much larger than the primary tumor, abdominal ultrasonography with special attention to the sublumbar area is recommended when an anal sac mass is palpated or in cases of hypercalcemia of unknown origin.
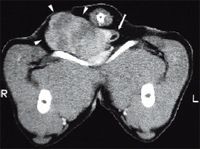
A transverse computed tomography image of a 9-year-old male neutered Siberian husky demonstrating a contrast-enhancing mass (arrowheads) originating from the right anal sac area and extending in the pelvic canal, pushing the rectum (arrow) laterally toward the left. This dog was treated with multimodality therapy consisting of surgical excision of the primary tumor and regional lymph nodes, followed by megavoltage radiation therapy and systemic chemotherapy. The dog was lost to follow-up more than two years later. Hypercalcemia rapidly resolved after supportive therapy and surgical excision of the primary and regional metastatic lesions.
REFERENCES
1. Rosol TJ, Nagode LA, Couto CG, et al. Parathyroid hormone (PTH)-related protein, PTH, and 1,25-dihydroxyvitamin D in dogs with cancer-associated hypercalcemia. Endocrinology 1992;131:1157-1164.
2. Morrison WB. Paraneoplastic syndromes and the tumors that cause them. In: Morrison WB. Cancer in dogs and cats: medical and surgical management. 2nd ed. Jackson, Wyo: Teton NewMedia, 2002;731-735.
3. Grone A, Weckmann MT, Blomme EA, et al. Dependence of humoral hypercalcemia of malignancy on parathyroid hormone-related protein expression in the canine anal sac apocrine gland adenocarcinoma (CAC-8) nude mouse model. Vet Pathol 1998;35:344-351.
4. Williams LE, Gliatto JM, Dodge RK, et al. Carcinoma of the apocrine glands of the anal sac in dogs: 113 cases (1985-1995). J Am Vet Med Assoc 2003;223:825-831.
5. Bennett PF, DeNicola DB, Bonney P, et al. Canine anal sac adenocarcinomas: clinical presentation and response to therapy. J Vet Intern Med 2002;16:100-104.
6. Rosol TJ, Capen CC, Danks JA, et al. Identification of parathyroid hormone-related protein in canine apocrine adenocarcinoma of the anal sac. Vet Pathol 1990;27:89-95.