What to do when you see a tooth of a different color
If your patient has a gray, pink, purple or blue tooth, dont just tell the owner to keep an eye on it. An intrinsically stained tooth is more than just a cosmetic issue, and the associated disease is often painful.
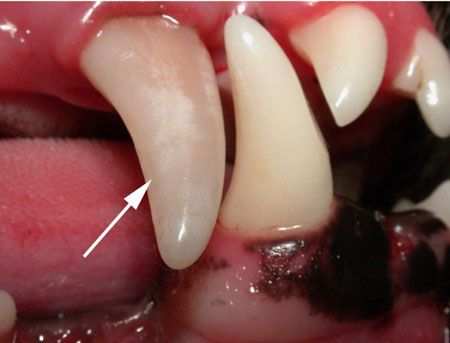
Discolored (nonvital) right maxillary canine tooth. All images courtesy of Dr. Barden Greenfield.We've all seen patients with stained teeth, and when we do, there's often an inclination to tell owners to simply “keep an eye on it.” But because these pets are often in pain, a wait-and-see approach won't cut it if you're striving to provide high-quality patient care.
The cause of discoloration
When the blood supply to a tooth is interrupted, either temporarily or permanently, hemoglobin in the pulp cavity is degraded into byproducts that leach into the dentin wall and give it a pink or purple hue. If these hemocomponents continue to break down, the tooth will appear blue or gray.
In one study of dogs with intrinsically stained teeth, more than 92% of the stained teeth were nonvital (i.e. had partial or total pulp necrosis).1 Teeth often become nonvital through trauma, which causes tooth subluxation, luxation or avulsion. In addition, anachoresis, a blood-borne infection, can affect a tooth at the apex and cause it to become nonvital.
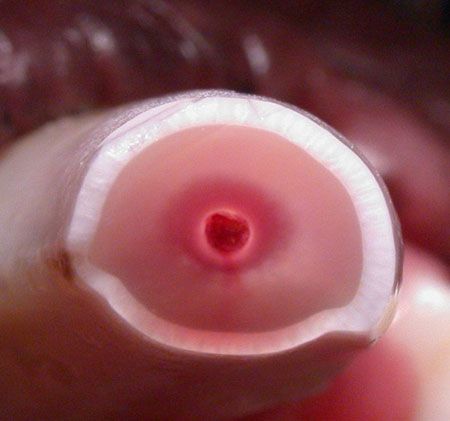
Cross-section of a nonvital canine tooth. Notice the intrinsic staining of the dentinal wall.Reversible pulpitis
Sometimes the tooth discoloration is nonpermanent, as is the case with reversible pulpitis, which is caused by inflammation or trauma. If treated appropriately, the pulp cavity can become viable again and the tooth discoloration may lessen and return to normal. Pain is common in people with acute periapical periodontitis or acute periapical abscess, so we should assume the same in our patients.
In an ideal world, we would know the exact time the trauma occurred or the inflammation began, but that's rare. If a tooth tip or the coronal one-fourth of a crown becomes acutely discolored, you can initially assume it is reversible pulpitis. Administer antibiotics (amoxicillin-clavulanate or clindamycin) and NSAIDs (provided the patient's renal and hepatic function is normal) for seven days. If the tooth's color doesn't return to normal after two or three months, you can assume it's experiencing irreversible pulpitis.
Irreversible pulpitis
Irreversible pulpitis can be a sterile event or bacteria-related. It can also be acute, subacute or chronic. If a bacterial infection combines with the hemoglobin breakdown products, iron sulfide is formed and causes teeth to turn dark gray or blue-colors that are practically pathognomonic for irreversible pulpitis. The condition may be acutely painful for the patient in the early stages but can diminish to a dull pain over time.1
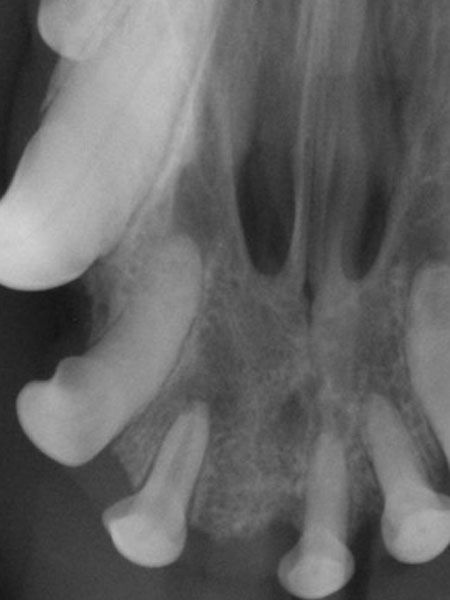
Intraoral digital dental radiograph of the right maxillary 2nd incisor tooth. A wide pulp cavity compared to the contralateral left 2nd incisor indicates premature maturation (tooth death). Radiography
Radiographic evidence of a nonvital tooth includes:
A wide pulp cavity in relation to the contralateral tooth
Apical rarefaction (apical lucency)
Narrowing of the pulp cavity because of pulp calcification (localized or generalized)
Root resorption
Although dental radiography can help you diagnose irreversible pulpitis, a lack of radiographic evidence does not rule it out. In one study, only 42.9% of nonvital teeth showed radiographic evidence of endodontic disease.1
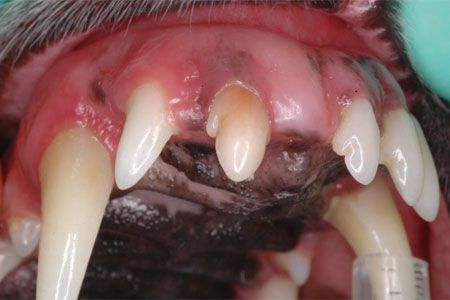
Discolored (nonvital) right maxillary 2nd incisor.Treating irreversible pulpitis
There are two options for treating irreversible pulpitis: root canal therapy and tooth extraction.
The former is highly recommended for strategic teeth (i.e. maxillary and mandibular canines, maxillary fourth premolars and mandibular first molars) as well as for the lateral incisors in large-breed patients. Root canal therapy removes the necrotic pulp and hermetically seals the canal with materials that allow the tooth to remain in the mouth for the life of the patient. The success rate of root canal therapy is over 90%. In many cases, a full-coverage crown is recommended.
While the success rate for surgical extraction is 100% (provided dental radiography is performed after the procedure to confirm complete extraction), it does have limitations and consequences. First, extractions can cause more pain than endodontic therapy and require a longer recovery period. If the patient likes to retrieve objects or chew, removing a strategic tooth may compromise that aspect of its life. Removing a mandibular canine tooth has its own unique set of risks involved as well, such as mandibular fracture or trauma to adjacent incisors and premolars. The tongue may also loll or fall to one side once the canine is removed.
Patients with intrinsically stained teeth deserve better than a wait-and-see approach. Give these pets high-quality care by giving their teeth a closer look.
Reference
1. Hale FA. Localized intrinsic staining of teeth due to pulpitis and pulp necrosis in dogs. J Vet Dent 2001;18(1):14-20.









