Dental Corner: Feline gingivostomatitis: How to relieve the oral discomfort
Feline gingivostomatitis is probably the most frustrating oral disease seen in veterinary practice. Cats with this chronic, painful inflammatory disease can be severely compromised, and medical treatment can cause adverse effects.
Feline gingivostomatitis is probably the most frustrating oral disease seen in veterinary practice. Cats with this chronic, painful inflammatory disease can be severely compromised, and medical treatment can cause adverse effects.

Daniel T. Carmichael, DVM, DAVDC
Affected cats exhibit a variety of clinical signs including partial to complete anorexia (often avoiding the hard portions of the diet), ptyalism, halitosis, weight loss, abnormal swallowing, and oral pain. Physical examination results show gingivitis, stomatitis, and possibly palatitis, glossitis, cheilitis, pharyngitis, and mandibular lymphadenopathy. Oral inflammation is often extensive, and affected tissues are typically ulcerated, proliferative, and hyperemic (Figures 1A & 1B). When gingivostomatitis was first described, purebred cats were reported to be at an increased risk,1 but all breeds of cat have the potential to develop the disease, including domestic shorthaired cats. And cats can become affected at any age.

Figure 1A. Gingivostomatitis in a cat. The cat is missing some teeth, but gingivitis is evident at the maxillary fourth premolar (arrow).
The good news is that most patients with feline gingivostomatitis can be cured or at least show marked improvement with treatment. But, unfortunately, some patients will require lifelong therapy.
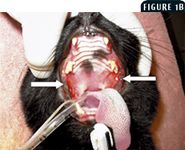
Figure 1B. A thorough examination of the caudal oral cavity is performed while the cat is anesthetized. Stomatitis is especially severe in the caudal pharyngeal area (arrows).
ETIOLOGY
The oral lesions associated with feline gingivostomatitis are often mistaken for an oral infection; however, gingivostomatitis is not an infection but rather an inflammation. The inflammatory lesions associated with feline gingivostomatitis are thought to be the result of a highly reactive immune system. The specific antigen that the immune system is reacting to is not easily identified and is often unknown. The fact that most of these lesions will resolve when the teeth are removed suggests the involvement of an antigen that is intimately associated with the teeth (i.e. bacteria). However, because not all inflammation resolves when the teeth are removed, it must be conceded that multiple antigens may be involved. Other antigens that may have a role in triggering the oral inflammation associated with feline gingivostomatitis include viral, food, or environmental antigens. Autoimmunity may also be a component of the disease.
DIAGNOSIS
Differential diagnoses for oral inflammation in a cat include feline gingivostomatitis, periodontal disease, inflammation secondary to feline odontoclastic resorptive lesions (FORLs), certain viral diseases (infection with feline herpesvirus or feline calicivirus) that can cause oral inflammation and ulceration, eosinophilic granuloma, oral ulceration secondary to uremia, and neoplasia. A complete patient evaluation is paramount to making a correct diagnosis and embarking down a specific treatment path.
To begin this evaluation, perform a physical examination, a complete blood count and serum chemistry profile, and serologic testing for feline leukemia virus and feline immunodeficiency virus infections. Perform additional testing and imaging as indicated. The results of these tests in cats with feline gingivostomatitis are usually unremarkable except for oral lesions, mandibular lymphadenopathy, and hyperglobulinemia.
Next, administer an inhalation anesthetic, and perform a dental prophylaxis. Perform a gross and radiographic examination of the oral cavity. Extract all teeth exhibiting FORLs and all teeth with advanced or end-stage periodontal disease. Also, remove any root fragments (best identified radiographically). Finally, obtain samples of the inflamed oral tissue by using a 4-mm skin biopsy punch at several locations of actively inflamed tissue, and submit them for histologic examination. A common site of inflammation is lateral to the palatoglossal folds (caudal stomatitis) (Figure 2).
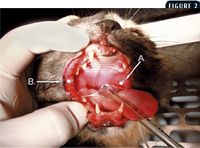
Figure 2. A common site from which to obtain a biopsy sample is lateral to the palatoglossal fold (A). If lip commissures are involved, obtain a sample of this area (B) as well.
Histologic examination results in cats with feline gingivostomatitis show plasmacytic stomatitis or lymphocytic-plasmacytic stomatitis. There may be concurrent neutrophilic inflammation or even a superficial bacterial component, but the predominant population of cells will be plasmacytes and lymphocytes.
TREATMENT
In rare cases, simply maintaining excellent oral hygiene will keep this condition under control. A home-care program may include daily tooth brushing and chlorhexidine (topical) application and long-term or long-term intermittent (pulse) antibiotic therapy. Antibiotics whose spectrum of activity includes gram-negative anaerobic bacteria are good empirical choices. Antibiotic therapy often produces favorable results initially; however, the benefits of antibiotic therapy seem to diminish over time. The Catch-22 of feline gingivostomatitis is that the cats that have had sore mouths for a long time are usually the poorest candidates to cooperate with a home-care regimen. When home care alone is not working or not possible, consider medical or surgical treatment.
Medical treatment
Unfortunately, the medical treatment options include either drugs with poor chances of success or drugs with serious side effects (e.g. corticosteroids). Many drugs have been used to treat feline gingivostomatitis with varying degrees of success. The most effective drug appears to be methylprednisolone acetate given at a dosage of 20 mg/cat injected subcutaneously every three weeks as needed. Other corticosteroids, such as oral prednisone, have also been used to successfully control feline gingivostomatitis. The goal is to find the lowest every-other-day oral dose that provides clinical control of the disease. Long-term corticosteroid treatment is not ideal because cats can develop serious side effects, including diabetes mellitus and iatrogenic hyperadrenocorticism. Avoiding corticosteroids is especially important when treating cats infected with feline leukemia virus or feline immunodeficiency virus.2
Nonsteroidal drugs that have been used to treat feline gingivostomatitis with limited success include interferon, cyclosporine, bovine lactoferrin, piroxicam, azathioprine, and gold salts. Many of these drugs are not labeled for use in cats and may have marked side effects.
Surgical treatment
Extracting all teeth (or sometimes just the teeth behind the canines) has cured feline gingivostomatitis. In one study, 60% of feline gingivostomatitis patients treated with extraction were clinically cured, and another 20% were significantly improved.3 This procedure is labor-intensive and will not be successful if any root fragments are left behind. In some patients, areas of abnormally appearing alveolar and perialveolar bone may also need to be removed. Having the proper dental radiography equipment and a high-speed drill before performing the extractions is highly recommended. Perioperative and postoperative patient monitoring and support, as well as appropriate analgesia, cannot be overemphasized. Patients with gingivostomatitis requiring surgical treatment are commonly referred to veterinary dental specialists (Figures 3A & 3B).
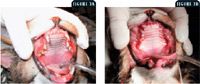
Figure 3A & 3B. A cat before and immediately after surgical treatment for gingivostomatitis. Providing postoperative supportive care and proper analgesia is essential in these patients. The patient should remain in the hospital until it is stable and eatingâÂÂusually one or two days.
When extracting teeth to treat feline gingivostomatitis, the question arises whether to extract canine and incisor teeth. A suggested approach is to extract canine and incisor teeth if they are diseased or if the surrounding tissues are markedly inflamed. If canine and incisor teeth are sound and inflammation is limited to the caudal portion of the oral cavity, the canine and incisor teeth may be spared.
REFRACTORY STOMATITIS
Even after having all teeth and roots removed, about 20% of patients with feline gingivostomatitis will continue to experience signs of oral inflammation (Figure 4).3 These cases are refractory, and the patients may require treatment for life. In refractory cases, no therapies work consistently, but several treatments can be used. The goal of treatment is to minimize corticosteroid use while markedly reducing or eliminating oral discomfort.
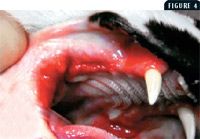
Figure 4. Refractory stomatitis in a cat that previously had its caudal dentition extracted.
Perform a radiographic re-examination of the dental arches to rule out retained root fragments or reactive periodontal tissue. If a patient's canine or incisor teeth were initially spared, extract these teeth now.
In some cases of refractory stomatitis, nonsteroidal anti-inflammatory drugs (NSAIDs) will provide relief. One NSAID that has shown effectiveness in cats with refractory stomatitis is piroxicam,4 which can be compounded into a liquid and administered at a dosage of 1 mg/cat orally every 72 hours. Side effects of piroxicam include gastrointestinal ulceration. Meloxicam (Metacam—Boehringer Ingelheim) is another NSAID that is not labeled for oral administration in cats but that may help control pain and inflammation. Avoid combining piroxicam, meloxicam, or any other NSAID with corticosteroids because it increases the probability of gastrointestinal ulceration.
Immunosuppressive and immunomodulatory drugs, such as cyclosporine, interferon, and azathioprine, can be used instead of NSAIDS to reduce oral inflammation, although the response varies and can take weeks to produce favorable results. To avoid serious or potentially fatal side effects, appropriate patient monitoring is paramount, especially when using azathioprine.
Laser ablation of the inflamed oral tissue has also been recommended. Tissue that has been treated with a laser has a reduced blood supply and may be less likely to become inflamed.5
REFERENCES
1. Harvey CE, Emily PP. Small animal dentistry. St. Louis, Mo: Mosby, 1993;151.
2. Wiggs RB, Lobprise HB. Domestic feline oral and dental disease. In: Wiggs RB, Lobprise HB, eds. Veterinary dentistry principles and practice. Philadelphia, Pa: Lippincott-Raven, 1997;482-517.
3. Hennet P. Chronic gingivo-stomatitis in cats: long-term follow-up of 30 cases treated by dental extractions. J Vet Dent 1997;14:15-21.
4. Manfra S, Urbana Ill: Personal communication, 2002.
5. Lyon KF. Gingivostomatitis. Vet Clin North Am Small Anim Pract 2005;35:891-911.
The information and photographs for "Dental Corner" were provided by Daniel T. Carmichael, DVM, DAVDC, Veterinary Medical Center, 75 Sunrise Highway, West Islip, NY 11795.